Definitions & Classification - Seizure Starters
- Seizure: Transient event from abnormal, excessive/synchronous brain neuronal activity.
- Epilepsy: ≥2 unprovoked seizures >24h apart; or 1 unprovoked seizure + high recurrence risk (e.g., >60% over 10 yrs).
- ILAE 2017 Classification:
- Focal Onset: Networks limited to one hemisphere.
- Aware / Impaired Awareness.
- Motor / Non-motor onset.
- Generalized Onset: Bilaterally distributed networks.
- Motor (e.g., Tonic-clonic, Atonic).
- Non-motor (Absence).
- Unknown Onset.
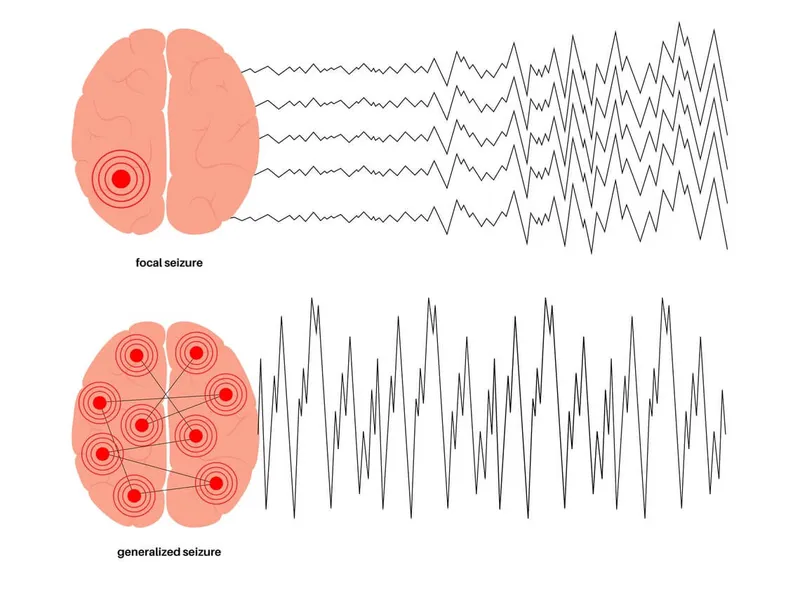
- Focal Onset: Networks limited to one hemisphere.
⭐ Simple febrile seizures do NOT increase risk of epilepsy. Complex febrile seizures do.
Etiology & Pathophysiology - Brainstorm Triggers
- Pathophysiology: ↑Excitatory (Glutamate) vs. ↓Inhibitory (GABA) neurotransmission.

- General Triggers:
- Fever (children 6m-5y)
- Sleep loss, stress
- Metabolic: ↓Glucose, ↓Na+, ↓Ca2+
- CNS Infections, Trauma, Hypoxia
- Toxins, Drug withdrawal
- Structural: Tumor, Stroke
- Genetic factors
- Age-Specific:
- Neonatal: HIE, ICH, Infection, Metabolic (Pyridoxine def.), IEM.
- Infancy: Febrile seizures, Infection, Genetic (West, Dravet).
- Childhood: Idiopathic, Infection, Trauma, Tumor. ⭐ > Pyridoxine (B6) deficiency: rare, treatable cause of neonatal/infant seizures. Trial IV pyridoxine 100mg.
Clinical Features & Diagnosis - Detective Workup
- History: Aura, LOC, motor features (type, duration), post-ictal state, triggers, FHx, developmental milestones.
- Examination: Neurocutaneous markers (e.g., ash-leaf spots), dysmorphism, focal neurological deficits.
- Key Investigations (1st unprovoked seizure):
- EEG: Essential for classification & prognosis.
- Neuroimaging (MRI preferred over CT): Indicated for focal seizures, abnormal neurological exam, or focal EEG findings.
- Labs: Blood glucose, electrolytes (Ca, Mg, Na). Lumbar Puncture (LP) if CNS infection suspected (e.g., fever, meningismus).
⭐ Todd's paralysis: A postictal focal weakness (e.g., hemiparesis) that can last for minutes to 48 hours after a focal seizure, mimicking a stroke.

Management Principles - Taming the Storm
- Status Epilepticus (SE): 📌 BZDs → AEDs → Anesthesia!
- 0-5 min: ABCs, IV access, Glucose.
- 5-20 min (1st line): IV Lorazepam (0.1mg/kg), Diazepam (0.2mg/kg), IM Midazolam (0.2mg/kg).
- 20-40 min (2nd line): IV Fosphenytoin (20mgPE/kg), Valproate (20-40mg/kg), Levetiracetam (30-60mg/kg), Phenobarbital (20mg/kg).
- >40 min (Refractory SE): Anesthesia (Midazolam/Propofol).
- Epilepsy (Long-Term):
- Goal: Monotherapy. Choice by seizure type.
- Key AEDs:
- Valproate (VPA): Broad; SE: Hepatotoxic, Teratogenic.
- Levetiracetam (LEV): Broad; SE: Behavioral.
- Ethosuximide (ESM): Absence.
⭐ Phenobarbital is often first-line for neonatal seizures.
Pediatric Epilepsy Syndromes - Kid-Specific Cases
| Syndrome | Age Onset | Seizure Types | EEG Pattern | Tx Highlights | Prognosis |
|---|---|---|---|---|---|
| West Syndrome | 3-12 mo | Infantile spasms | Hypsarrhythmia | ACTH, Vigabatrin | Poor |
| Lennox-Gastaut (LGS) | 1-8 yr | Multiple (tonic, atonic, atypical absence) | Slow spike-wave (<2.5 Hz) | Valproate, Clobazam | Poor |
| Childhood Absence (CAE) | 4-10 yr | Typical absence | 3 Hz spike-wave | Ethosuximide | Good |
| Benign Rolandic (BRE) | 3-13 yr | Nocturnal focal motor, oro-pharyngeal | Centrotemporal spikes | Often none, Levetiracetam | Excellent |
⭐ Vigabatrin is first-line for infantile spasms in Tuberous Sclerosis.
High‑Yield Points - ⚡ Biggest Takeaways
- Febrile seizures: common; complex (focal, >15 min, recurrent in 24h) needs EEG/imaging.
- Infantile spasms: hypsarrhythmia on EEG; treat with ACTH or vigabatrin.
- Absence seizures: 3 Hz spike-wave on EEG; ethosuximide is first-line.
- Lennox-Gastaut syndrome: multiple seizure types, slow spike-wave EEG, intellectual disability.
- Status epilepticus: seizure >5 min; benzodiazepines first, then fosphenytoin/levetiracetam.
- JME: morning myoclonus, GTCs; valproate (caution: teratogenic).
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

