Proximal Tubule Pathologies - First-Stop Fumbles
- Fanconi Syndrome: Generalized proximal tubule defect. 📌 Impaired reabsorption of: Glucose, Amino acids, Phosphate ($PO_4^{3-}$), Bicarbonate ($HCO_3^-$), Uric acid, Potassium ($K^+$), Low Molecular Weight Proteins.
- Causes (Inherited): Cystinosis (commonest), Wilson's disease, Lowe syndrome, Galactosemia.
- Causes (Acquired): Heavy metals (Pb, Hg), Drugs (Ifosfamide, Tenofovir, outdated Tetracyclines), Multiple Myeloma.
- Features: Polyuria, growth failure, rickets/osteomalacia (due to ↓$PO_4^{3-}$), proximal RTA.
- Labs: Glucosuria (normal blood glucose), aminoaciduria, phosphaturia (↓$PO_4^{3-}$), hypokalemia.
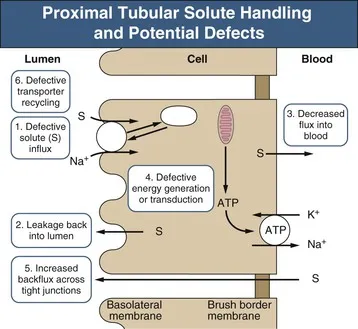
- Proximal Renal Tubular Acidosis (Type 2 RTA): Isolated defect in $HCO_3^-$ reabsorption.
- ↓ $HCO_3^-$ reabsorption threshold (serum $HCO_3^-$ often 15-18 mEq/L).
- Urine pH: > 5.5 if serum $HCO_3^-$ is normal/high; < 5.5 if serum $HCO_3^-$ is low (steady state).
- Fractional Excretion of $HCO_3^-$ (FE$HCO_3^-$) > 15% when plasma $HCO_3^-$ normalized.
- Features: Growth failure, mild non-anion gap metabolic acidosis (NAGMA), hypokalemia.
- Treatment: High-dose alkali (e.g., $NaHCO_3$ or K-citrate, 10-15 mEq/kg/day), thiazides.
⭐ Cystinosis is the most common inherited cause of Fanconi Syndrome in children, characterized by intralysosomal cystine accumulation in proximal tubular cells.
Loop & Distal Tubule Disorders - Mid-Stream Mayhem
- General: Inherited channelopathies causing hypokalemia, metabolic alkalosis. Blood pressure (BP) varies.
- Bartter Syndrome (Loop - NKCC2 defect; Autosomal Recessive - AR)
- Mimics loop diuretic; severe salt-wasting from birth/infancy.
- Hypokalemia, metabolic alkalosis, polyuria, polydipsia.
- Hypercalciuria → nephrocalcinosis, kidney stones.
- Normal/↓ BP, ↑ Renin & Aldosterone. Prostaglandin E2 often ↑ (target for NSAIDs).
- 📌 "BarTTer = Thick ascending limb, Terrible K+ loss, Too much Ca2+ in urine."
- Gitelman Syndrome (Distal Tubule - NCC defect; AR)
- Mimics thiazide diuretic; milder salt-wasting, presents later (childhood/adulthood).
- Hypokalemia, metabolic alkalosis, often less severe.
- Hypocalciuria (key diagnostic), hypomagnesemia (→ tetany, muscle cramps, weakness).
- Normal/↓ BP, ↑ Renin & Aldosterone. Better prognosis than Bartter.
- 📌 "GiTelman = Thiazide-like, Tiny Ca2+ in urine."
- Liddle Syndrome (Distal Tubule/Collecting Duct - ENaC Gain-of-Function; Autosomal Dominant - AD)
- Pseudoaldosteronism: ENaC hyperactivity mimics ↑ aldosterone effects.
- Presents early: severe hypertension, hypokalemia, metabolic alkalosis.
- Key: ↓ Renin & ↓ Aldosterone (due to Na+ retention & volume expansion).
- Tx: Amiloride or Triamterene (ENaC blockers); low salt diet. Avoid spironolactone.
⭐ Bartter vs. Gitelman: Urinary calcium is the key. Bartter = Hypercalciuria (like loop diuretics). Gitelman = Hypocalciuria (like thiazide diuretics).
Collecting Duct & K+ Imbalances - End-Pipe Enigmas
-
Principal Cells: Na+ reabsorption (ENaC), K+ secretion (ROMK), H2O reabsorption (Aquaporin-2 via ADH).
-
Intercalated Cells: Acid-base balance, K+ reabsorption.
-
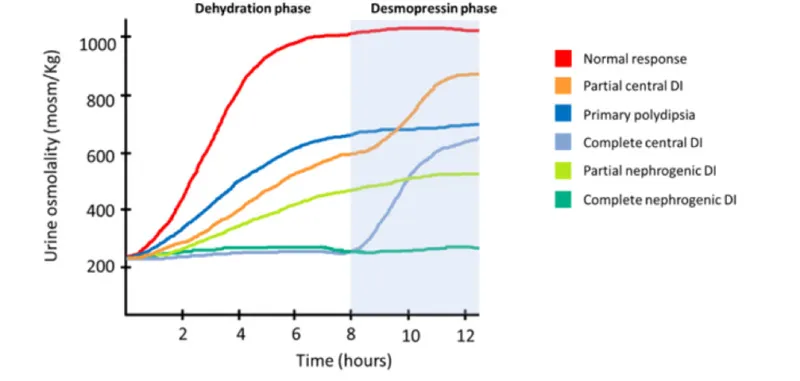
Diabetes Insipidus (DI): Polyuria, dilute urine.
- Central: ↓ADH. Tx: Desmopressin.
- Nephrogenic: ADH resistance (Lithium, V2R/AQP2 defect). Tx: Thiazides, Amiloride.
-
SIADH: ↑ADH → Euvolemic hyponatremia. Tx: Fluid restriction.
-
Liddle Syndrome: ENaC gain-of-function. Hypertension, ↓K+, ↓Aldo, ↓Renin. Tx: Amiloride. 📌 Liddle = Low Aldo.
-
Pseudohypoaldosteronism Type 1 (PHA-1): ENaC/MR defect. Salt wasting, ↑K+, ↑Aldo, ↑Renin.
-
K+ Imbalances:
- Hyperkalemia: ECG: Peaked T. Tx: Ca-gluconate, Insulin+Dextrose.
- Hypokalemia: ECG: U wave. Tx: K+ repletion.
⭐ Liddle syndrome: hypertension, hypokalemia, with suppressed renin and aldosterone.
High‑Yield Points - ⚡ Biggest Takeaways
- Fanconi syndrome: Generalized proximal tubule defect (glycosuria, phosphaturia, aminoaciduria, RTA Type 2).
- Bartter syndrome: TALH defect (NKCC2); hypokalemia, metabolic alkalosis, hypercalciuria, normal BP.
- Gitelman syndrome: DCT defect (NCC); hypokalemia, metabolic alkalosis, hypomagnesemia, hypocalciuria, normal BP.
- Liddle syndrome: ENaC gain-of-function; hypertension, hypokalemia, metabolic alkalosis (pseudoaldosteronism).
- RTA Type 1 (Distal): Impaired H+ secretion (distal); hypokalemia, urine pH >5.5, nephrocalcinosis.
- RTA Type 2 (Proximal): Impaired HCO3- reabsorption (proximal); hypokalemia, self-limiting acidosis.
- Nephrogenic DI: ADH resistance; polyuria, dilute urine, hypernatremia if poor water access.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

