Immunocompromised Child - Weakened Shields
- Opportunistic Infection (OI): Infection by organisms typically non-pathogenic in healthy individuals.
- Causes of Weakened Shields:
- HIV/AIDS
- CD4 <1500 or <25% (<1yr)
- CD4 <750 or <20% (1-5yr)
- CD4 <500 or <15% (>5yr) indicates severe suppression.
- Primary Immunodeficiencies (SCID, DiGeorge)
- Malignancy & Chemotherapy
- Transplant Recipients (Solid Organ/Stem Cell)
- Immunosuppressive Drugs (e.g., corticosteroids)
- Malnutrition
- HIV/AIDS
- General Approach: Prophylaxis, early diagnosis, prompt treatment.
⭐ Severe Combined Immunodeficiency (SCID) often presents in the first few months of life with failure to thrive, persistent diarrhea, and recurrent severe opportunistic infections (e.g., PJP, Candida, CMV) often after administration of live vaccines.
Fungal Foes - PJP & Candida
-
Pneumocystis jirovecii Pneumonia (PJP)
- Risk: CD4 < 200/µL (older children/adults), age-specific pediatric criteria.
- Sx: Insidious fever, tachypnea, dyspnea, non-productive cough, hypoxia.
- CXR: Bilateral interstitial infiltrates ('ground-glass').
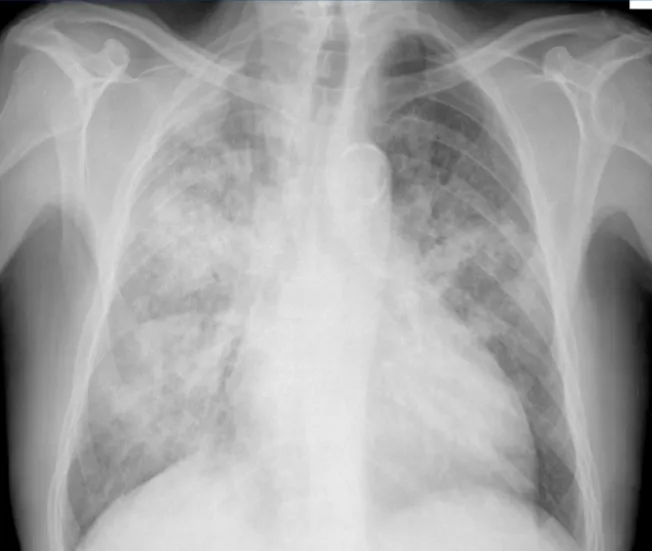
- Dx: Organism in BAL/sputum. LDH ↑.
- Rx: TMP-SMX (21 days). Steroids if PaO2 < 70mmHg.
- Prophylaxis: TMP-SMX. 📌 PJP: Pneumo Jiroveci = Just Juice (TMP-SMX).
-
Candidiasis
- Oral thrush: Creamy white plaques.
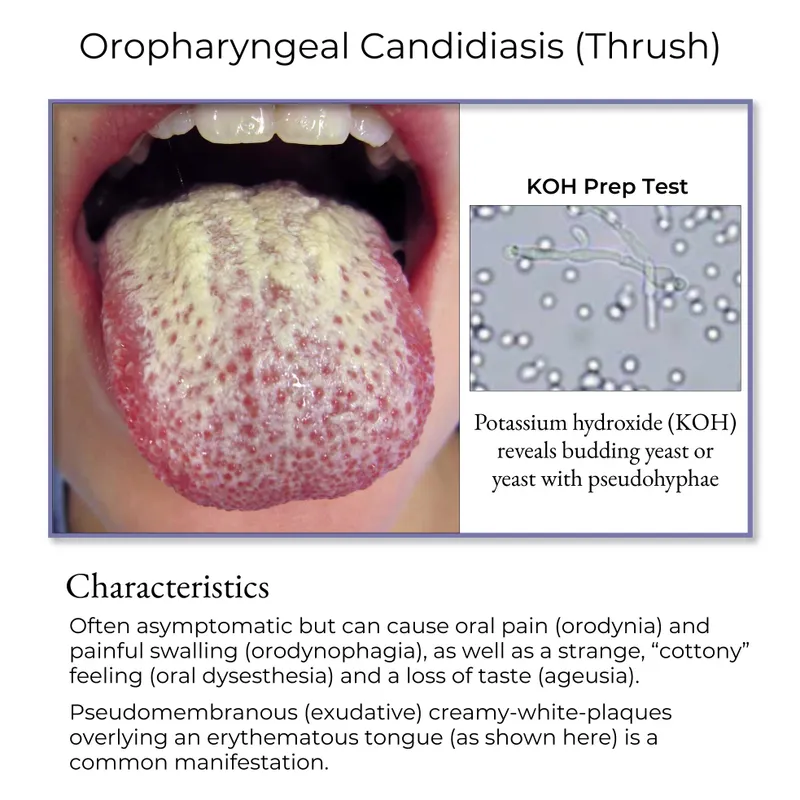
- Esophagitis: Dysphagia, odynophagia.
- Disseminated: Hepatosplenic, endocarditis.
- Dx: KOH prep (pseudohyphae, yeasts), culture.
- Rx: Oral (Nystatin), Esophageal/Systemic (Fluconazole, Amphotericin B).
- Oral thrush: Creamy white plaques.
⭐ PJP prophylaxis with TMP-SMX is indicated for all infants born to HIV-infected mothers starting at 4-6 weeks of age and continued until HIV infection is reliably excluded (two negative virologic tests, one at ≥1 month and one at ≥4 months, or two negative antibody tests at ≥6 months).
Viral Villains - CMV & Friends
- Cytomegalovirus (CMV): Most common Opportunistic Infection (OI) in Solid Organ Transplant (SOT) recipients.
-
Manifestations: Retinitis ('pizza-pie' or 'cotton-wool spots'), colitis (diarrhea, hematochezia), pneumonitis, hepatitis, esophagitis, bone marrow suppression.
-
Diagnosis: CMV DNA PCR (blood, CSF, BAL), biopsy with 'owl's eye' intranuclear inclusions.
-
Treatment: Ganciclovir (IV), Valganciclovir (PO). Foscarnet/Cidofovir for resistant strains.
-
Prophylaxis/Pre-emptive therapy in high-risk.
⭐ CMV retinitis is a sight-threatening OI, particularly in children with advanced HIV/AIDS or post-transplant; fundoscopy reveals characteristic hemorrhages and exudates often described as a 'pizza-pie' appearance.
-
- Herpes Simplex Virus (HSV) & Varicella-Zoster Virus (VZV): Can cause severe, disseminated, or recurrent disease.
- HSV: Mucocutaneous lesions, esophagitis, encephalitis.
- VZV: Severe chickenpox, disseminated zoster, chronic VZV.
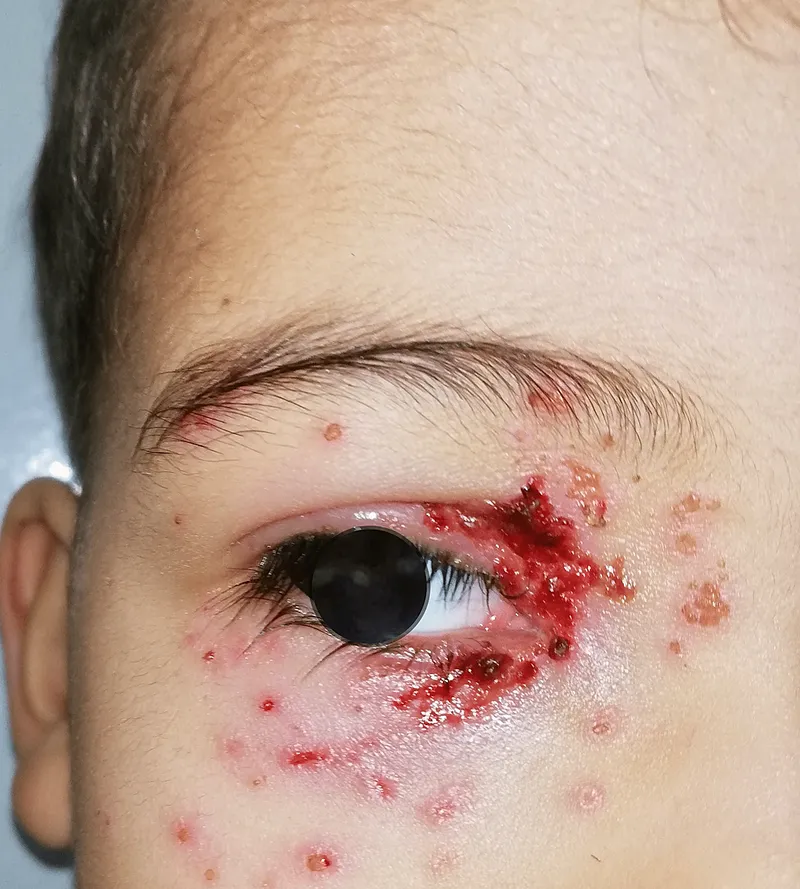
- Diagnosis: PCR, Direct Fluorescent Antibody (DFA) from lesions.
- Treatment: Acyclovir (IV for severe/disseminated).
- Epstein-Barr Virus (EBV):
- Associated with Post-Transplant Lymphoproliferative Disorder (PTLD).
- Diagnosis: EBV DNA PCR, biopsy.
- Management: Reduce immunosuppression, Rituximab, chemotherapy.
Bacterial & Parasitic Pathogens - Sneaky Invaders
- TB (Mycobacterium tuberculosis):
- Risk: Disseminated/extrapulmonary.
- Dx: Standard (TST may be anergic, IGRA, Xpert).
- Rx: Standard anti-TB drugs, longer duration may be needed.
- MAC (Mycobacterium Avium Complex):
- Risk: Advanced HIV (CD4 < 50/µL).
- Sx: Systemic (fever, sweats, weight loss), diarrhea.
- Dx: Blood culture, biopsy.
- Prophylaxis: Azithromycin/Clarithromycin.
- Toxoplasma gondii:
- CNS: Encephalitis, ring-enhancing lesions (CT/MRI).

- Risk: HIV (CD4 < 100/µL, IgG+).
- Prophylaxis: TMP-SMX.
⭐ In HIV-infected children, primary prophylaxis against Toxoplasma gondii encephalitis is recommended with TMP-SMX when CD4 count falls below 100/µL (or equivalent age-specific %CD4) if the child is Toxoplasma IgG seropositive.
- CNS: Encephalitis, ring-enhancing lesions (CT/MRI).
- Cryptosporidium parvum:
- Sx: Severe chronic diarrhea, wasting.
- Dx: Stool (modified acid-fast).
- Rx: Supportive, Nitazoxanide.
High‑Yield Points - ⚡ Biggest Takeaways
- PCP prophylaxis (TMP-SMX) for HIV-exposed infants from 4-6 weeks, guided by CD4 counts.
- CMV retinitis: major cause of blindness in AIDS; characteristic "pizza-pie" fundoscopy.
- Disseminated MAC (CD4 < 50): fever, weight loss, anemia; requires multi-drug therapy.
- Cryptococcal meningitis: diagnose with India ink or CrAg (CSF/serum).
- Cerebral toxoplasmosis: multiple ring-enhancing lesions on CT/MRI; TMP-SMX prophylaxis (CD4 < 100 & IgG+).
- PML (JC virus): progressive neurological deficits, poor prognosis, no specific cure.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

