Development of Immune System - Tiny Defender Kickstart
- Primary Lymphoid Organs: Bone Marrow (B-cells), Thymus (T-cells).
- Hematopoiesis Sites: Yolk Sac (3 wks) → Liver (6 wks) → Bone Marrow (BM) (20 wks).
- Thymus: From 3rd pharyngeal pouch; T-cell education. Max size at puberty.
- B-cells: Develop in fetal liver, then primarily in BM.
- Immunoglobulins (Ig):
- Fetal IgM: First Ig produced by fetus (around 20 weeks).
- Maternal IgG: Crosses placenta (starts ~16-20 weeks); provides passive immunity.
- IgA: Low at birth; secretory IgA (sIgA) acquired via breast milk.
- Complement System: Present at birth, but at ↓ levels (50-70% of adult).
⭐ Maternal IgG is the only antibody class to significantly cross the placenta, providing crucial passive immunity to the newborn for the first few months of life.
Development of Immune System - Ready-Set-Go Guards
- Innate Immunity: Immediate, non-specific defense. "Ready-Set-Go!"
- Barriers: Skin, mucous membranes.
- Cellular Guards:
- Phagocytes: Neutrophils (1st responders), Macrophages.
- Natural Killer (NK) cells: Virus/tumor surveillance.
- Mast cells, Eosinophils, Basophils.
- Humoral Factors:
- Complement system.
- Lysozyme, Interferons, Acute Phase Proteins (CRP).
- Neonatal Nuances:
- Phagocytosis: Present; chemotaxis & killing may be ↓.
- NK cell function: Matures postnatally.
-
⭐ Complement components are lower in newborns, reaching adult levels by 6-18 months (esp. alternative pathway).
- TLR expression: Develops with age.

Development of Immune System - Memory Makers March
- Primary Lymphoid Organs: Bone marrow (B-cells), Thymus (T-cells).
- B-cells: Mature in B_one marrow.
- T-cells: Mature in T_hymus. 📌 Mnemonic: B in Bone marrow, T in Thymus.
- T-Cell Development (Thymus):
- Positive selection: Selects T-cells recognizing self-MHC.
- Negative selection: Eliminates self-reactive T-cells (central tolerance).
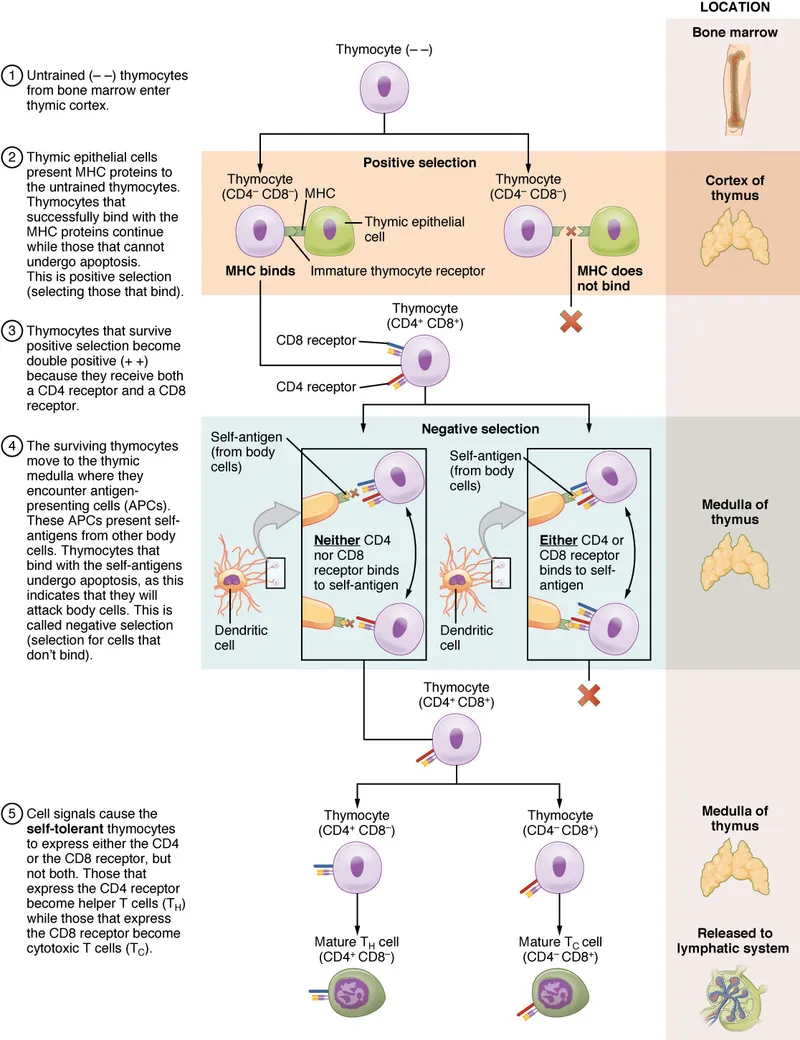
- B-Cell Development (Bone Marrow):
- Antigen-independent phase: Ig gene rearrangement (VDJ recombination).
- Mature naive B-cells co-express IgM & IgD on surface.
- Immunoglobulin Timeline & Maternal Transfer:
- Key Immunoglobulins:
- IgM: First Ab produced by fetus; indicates intrauterine infection if elevated at birth.
- IgG: Crosses placenta (passive immunity); smallest Ig, most abundant in serum.
- IgA: Secretory IgA in breast milk protects neonatal gut.
⭐ DiGeorge syndrome (22q11.2 deletion) causes thymic aplasia/hypoplasia, leading to deficient T-cell numbers and impaired cell-mediated immunity, recurrent viral/fungal infections.
Development of Immune System - Growth Factors & Glitches
- Immune Growth Factors:
- Cytokines: IL-7 (T/B cell dev), IL-2 (T-cell prolif), IL-4/5/6 (B-cell diff, Ig).
- Hormones: Thymic hormones (T-cell maturation).
- Nutrition: Zinc, Iron, Vit A/C/D/E. PEM causes severe impairment.
- Factors Impairing Development:
- Genetic: e.g., SCID, DiGeorge.
- Intrauterine: TORCH, maternal malnutrition, drugs (steroids).
- Neonatal: Prematurity (↓IgG, poor T-indep. response), sepsis.
- Other: Environmental toxins, chronic stress.
⭐ Neonates show ↓ opsonic activity & complement; highly susceptible to encapsulated bacteria (e.g., S. pneumoniae, H. influenzae). Maternal IgG wanes by 3-6 months.
High‑Yield Points - ⚡ Biggest Takeaways
- Fetal liver is the primary hematopoietic site, later shifting to bone marrow.
- Thymus is crucial for T-cell maturation; well-developed at birth, peak size in early adolescence.
- B-cells initiate development in the fetal liver, then mature in bone marrow.
- IgM is the first immunoglobulin produced by the fetus, indicating intrauterine infection if elevated.
- Maternal IgG crosses the placenta providing passive immunity; levels nadir at 3-6 months (physiologic hypogammaglobulinemia).
- Secretory IgA, primarily from breast milk, offers vital mucosal protection.
- The spleen is immunologically active at birth, crucial for defense against encapsulated bacteria.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

