Initial Assessment - Bleed Detectives
- Focused History:
- Onset & Type: Spontaneous vs. post-trauma/surgery? Neonatal onset?
- Sites: Mucocutaneous (epistaxis, gum bleed, menorrhagia) vs. deep tissue (hemarthrosis, muscle hematoma).
- Severity & Frequency: Quantify if possible.
- Family History: Bleeding disorders? Consanguinity?
- Drug History: NSAIDs, anticoagulants.
- Systemic Illness: Liver/renal disease, infections.
- Clinical Examination:
- Skin/Mucosa: Petechiae (<2mm), purpura (2mm-1cm), ecchymoses (>1cm), hematomas.
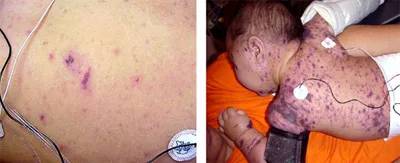
- Joints: Hemarthrosis (swelling, pain, restricted movement).
- General: Pallor, jaundice, hepatosplenomegaly.
- Skin/Mucosa: Petechiae (<2mm), purpura (2mm-1cm), ecchymoses (>1cm), hematomas.
⭐ Mucocutaneous bleeding (gums, nose, GI, menorrhagia) suggests platelet disorders or von Willebrand disease; deep tissue bleeding (joints, muscles, CNS) suggests coagulation factor deficiencies.
Lab Investigations - Initial Clues
- Initial Screening Tests:
- CBC: Platelet count.
- PT: Extrinsic & common pathways.
- aPTT: Intrinsic & common pathways.
- BT/PFA-100: Platelet function, vWD screen.
⭐ A mixing study (patient plasma + normal plasma) helps differentiate factor deficiency (correction of PT/aPTT) from a factor inhibitor (no correction).
Primary Hemostasis Disorders - Plug Problems
Mucocutaneous bleeds (petechiae, epistaxis). Labs: PT/aPTT normal, ↑BT/PFA-100.
-
Immune Thrombocytopenic Purpura (ITP)
- Patho: Anti-GpIIb/IIIa Abs → ↓platelets.
- Features: Isolated ↓Plt, post-viral (kids).
- BM: ↑Megakaryocytes.
-
von Willebrand Disease (vWD)
- Patho: vWF def./defect (binds FVIII).
- Labs: ↑BT/PFA, ↓vWF:Ag, ↓Risto. Cof; Plt N/↓; aPTT often ↑.
⭐ von Willebrand Disease is the most common inherited bleeding disorder, typically presenting with mucocutaneous bleeding and often a normal platelet count but prolonged PFA-100/Bleeding Time.
-
Bernard-Soulier Syndrome (BSS)
- Patho: GpIb defect (adhesion); AR.
- Features: Thrombocytopenia, GIANT platelets.
- Labs: ↓Plt (giant), ↑BT. No Ristocetin agg.
-
Glanzmann Thrombasthenia (GT)
- Patho: GpIIb/IIIa defect (aggregation); AR.
- Features: Normal platelet count.
- Labs: Normal Plt, ↑BT. No ADP/collagen/epi agg.
-
Drug-induced Platelet Dysfunction
- Aspirin (irreversible), NSAIDs (reversible): ↓TXA2 → impaired aggregation.
Secondary Hemostasis Disorders - Factor Fumbles
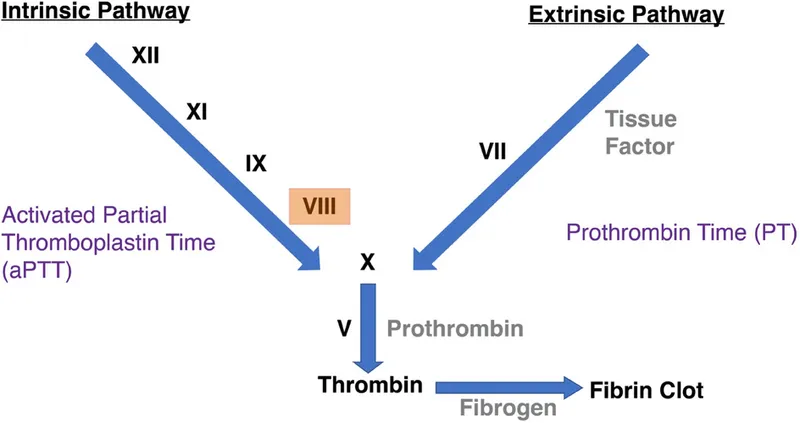
- Hemophilia A: Factor VIII↓. X-linked recessive. Deep bleeds (joints, muscles). Lab: ↑aPTT; Normal PT, Platelet count, BT.
- Hemophilia B (Christmas Disease): Factor IX↓. X-linked recessive. Clinically like Hemophilia A. Lab: ↑aPTT; Normal PT, Platelet count, BT.
⭐ Hemophilia A (Factor VIII deficiency) and Hemophilia B (Factor IX deficiency) are X-linked recessive disorders characterized by prolonged aPTT with normal PT and platelet count.
- Vitamin K Deficiency: Factors II, VII, IX, X, Protein C, S↓. Acquired (e.g., antibiotics, warfarin). Lab: ↑PT (early, due to FVII short half-life), then ↑aPTT.
- Von Willebrand Disease (vWD): vWF↓ (stabilizes FVIII). Autosomal Dominant (most common type). Mucocutaneous bleeding. Lab: Often ↑BT, may have ↑aPTT (due to FVIII↓). Normal PT, Platelet count usually normal.
High‑Yield Points - ⚡ Biggest Takeaways
- Initial screening: CBC (platelets), PT, aPTT are crucial first steps.
- Isolated thrombocytopenia often suggests Immune Thrombocytopenic Purpura (ITP).
- Prolonged aPTT with normal PT points to Hemophilia A/B or vWD (severe).
- Von Willebrand Disease (vWD) is the most common inherited bleeding disorder; presents variably.
- Mixing studies differentiate factor deficiency (corrects) from inhibitors (no correction).
- Vitamin K deficiency classically prolongs PT more than aPTT.
- Platelet function defects (e.g., Glanzmann's) show normal platelet count but abnormal function tests.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

