GER: Definition & Pathophysiology - Reflux Rundown
- Gastroesophageal Reflux (GER):
- Physiological passage of gastric contents into esophagus.
- Affects >50% infants <3 months; peaks at ~4 months (~70%).
- Usually resolves by 12-18 months.
- Gastroesophageal Reflux Disease (GERD):
- GER causing troublesome symptoms (e.g., FTT, cry/fuss, esophagitis) or complications.
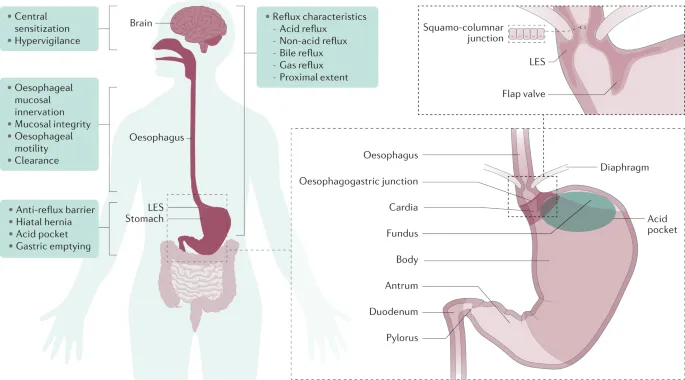
- Pathophysiology - Multifactorial:
- TLESRs (Transient Lower Esophageal Sphincter Relaxations): Primary cause; inappropriate LES relaxation.
⭐ TLESRs, not chronically low basal LES tone, are the predominant mechanism of GER in most infants and children.
- LES Dysfunction: ↓ basal LES pressure, shorter intra-abdominal LES.
- Impaired Esophageal Clearance: Ineffective peristalsis.
- Delayed Gastric Emptying: ↑ gastric volume.
- TLESRs (Transient Lower Esophageal Sphincter Relaxations): Primary cause; inappropriate LES relaxation.
GER: Clinical Features - Spit Happens
- Infants ("Happy Spitters"):
- Effortless, non-bilious regurgitation.
- Normal growth. Resolves by 12-18 months.
- Older Children/Adolescents:
- Heartburn, regurgitation, epigastric pain.
- Extraesophageal: chronic cough, hoarseness.
- ⚠️ Alarm Signs (Suspect GERD/Other):
- Forceful, bilious, bloody vomiting.
- FTT, weight loss.
- Feeding refusal, irritability.
- Hematemesis, melena.
- Respiratory: apnea, recurrent pneumonia.
- Onset >6mo / persists >18mo.
- Dysphagia/odynophagia.
⭐ Sandifer syndrome: A rare manifestation of GERD in infants, characterized by abnormal posturing of the head, neck, and trunk (opisthotonus, torticollis).
GER: Diagnostic Workup - Scope It Out?
- Clinical diagnosis for uncomplicated GER.
- Investigate if RED FLAGS:
- FTT, forceful/bilious vomit, hematemesis.
- Dysphagia, apnea/ALTE.
- Onset >6mo, persists >12-18mo, failed therapy.
- Investigations:
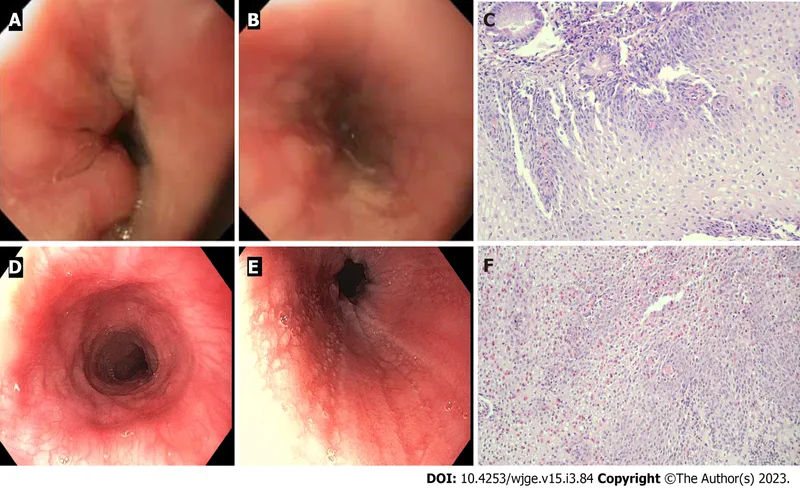
- EGD + Biopsy: For esophagitis, complications (strictures), alarm symptoms. Visualizes mucosa, histology.
- 24-hr pH-metry/MII-pH:
- pH-metry: Quantifies acid reflux (RI >7% infants, >4% children).
- MII-pH: Detects acid & non-acid reflux.
- Barium Swallow: Rules out anatomical defects. Not for GER dx.
⭐ Endoscopy + biopsy: key for esophagitis, complications, or alarm symptoms if empiric therapy fails.
GER: Management & Complications - Tummy Tamers
Management Strategy: Stepwise approach.
Complications:
- Esophagitis (can lead to bleeding, anemia)
- Peptic stricture (dysphagia)
- Failure to thrive (FTT)
- Respiratory:
- Recurrent aspiration pneumonia
- Chronic cough, wheeze
- Apnea / BRUE (Brief Resolved Unexplained Event)
- Sandifer syndrome
- Dental erosions
- Barrett's esophagus (rare in children)
⭐ Sandifer syndrome: characterized by abnormal, dystonic posturing of the head, neck, and trunk (arching, torticollis) associated with GERD episodes.
High‑Yield Points - ⚡ Biggest Takeaways
- Physiologic GER: Common in infants, resolves by 12-18 months; "happy spitters".
- GERD: Pathologic, causes poor weight gain, irritability, respiratory complications.
- Sandifer syndrome: GER with torticollis and abnormal posturing.
- Diagnosis: Primarily clinical; 24-hr pH monitoring is gold standard if needed.
- Management: Step-up approach - lifestyle (thickened feeds, positioning) then PPIs.
- Red flags: Bilious vomiting, GI bleeding, forceful vomiting, FTT.
- Consider cow's milk protein allergy as a mimic or contributor_._
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

