RLDs Overview - Lungs Under Pressure
RLDs: Group of disorders causing ↓ lung expansion & ↓ Total Lung Capacity (TLC).
- Pathophysiology: ↑ Lung stiffness (↓ compliance) or chest wall/neuromuscular dysfunction.
- Key PFTs:
- Hallmark: ↓ TLC (<80% predicted)
- ↓ FVC, ↓ FEV1
- FEV1/FVC ratio: Normal or ↑ (typically >0.7 as both ↓ proportionally or FVC ↓ more)
- ↓ DLCO (common in parenchymal RLDs)
- Types:
- Intrinsic (Parenchymal): IPF, Sarcoidosis
- Extrinsic: Kyphoscoliosis, Myasthenia Gravis
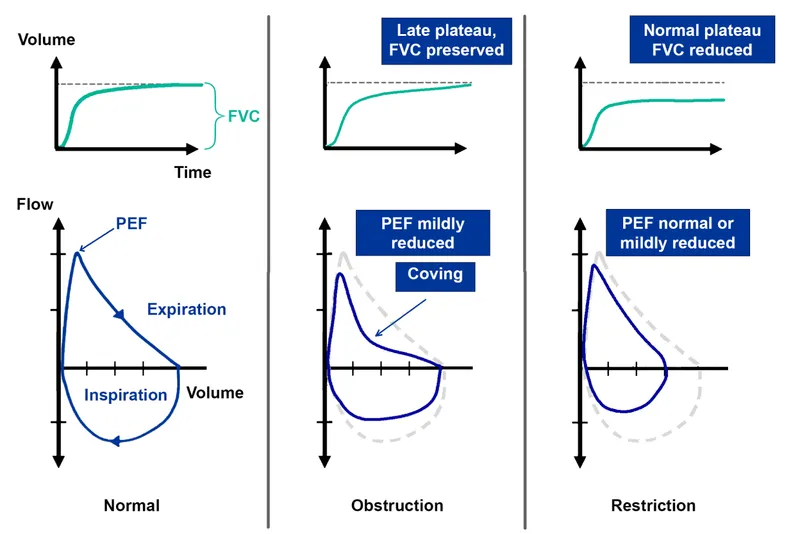
⭐ Hallmark of RLDs is a decreased Total Lung Capacity (TLC) with a normal or increased FEV1/FVC ratio.
IIPs Deep Dive - Mysterious Fibrosis
Idiopathic Interstitial Pneumonias (IIPs): Group of diffuse parenchymal lung diseases of unknown cause, characterized by varying degrees of inflammation and fibrosis. Focus on IPF.
- Idiopathic Pulmonary Fibrosis (IPF): Most common and severe IIP.
- Etiology: Unknown; associations: smoking, genetics (e.g., MUC5B, TERT, TERC).
- Pathology: Usual Interstitial Pneumonia (UIP) pattern is the hallmark.
- Key features: Temporal heterogeneity (old & new fibrosis), spatial heterogeneity (patchy), fibroblastic foci (active fibrosis), architectural distortion.
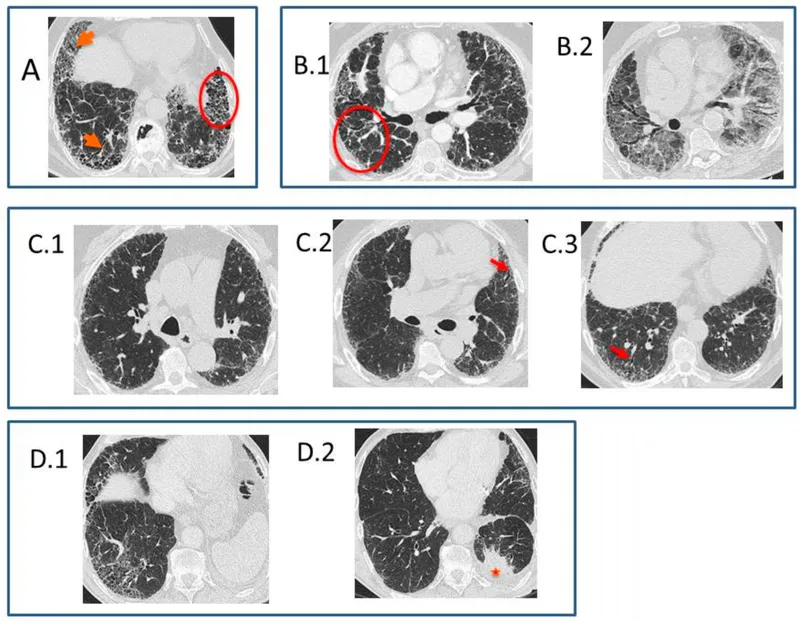
- Gross/CT: Honeycomb lung (esp. subpleural, basal).
- Clinical: Insidious onset dyspnea, dry cough, digital clubbing, bibasilar inspiratory crackles ("velcro rales").
- Diagnosis: HRCT (typical UIP: subpleural, basal predominant reticulation, honeycombing, traction bronchiectasis). Biopsy if HRCT atypical.
- Prognosis: Poor, median survival ~3-5 years post-diagnosis.
⭐ Fibroblastic foci are crucial microscopic findings in UIP, representing sites of ongoing, active collagen deposition by myofibroblasts.
- Other notable IIPs:
- Non-Specific Interstitial Pneumonia (NSIP): Better prognosis than IPF; cellular or fibrotic patterns.
- Cryptogenic Organizing Pneumonia (COP): Good response to steroids.
Occupational & Environmental RLDs - Inhaled Insults
- Pneumoconioses: Inorganic dust inhalation → macrophage activation → fibrosis.
-
Coal Worker's Pneumoconiosis (CWP): Coal dust. Simple (macules/nodules <1cm, upper lobes); Complicated (Progressive Massive Fibrosis, PMF >2cm). Caplan Syndrome (CWP + RA nodules).
-
Silicosis: Silica dust (mining, sandblasting). ↑ TB risk (impaired macrophage function). Eggshell calcification of hilar lymph nodes. Apical fibronodules.
-
Asbestosis: Asbestos fibers. Ferruginous bodies. Pleural plaques (most common manifestation, parietal). Basilar predominant fibrosis. ↑ Risk: Bronchogenic carcinoma (most common cancer), mesothelioma.
-
Berylliosis: Beryllium exposure. Non-caseating granulomas; mimics sarcoidosis.
-
- Hypersensitivity Pneumonitis (HP): Immune-mediated (Type III/IV hypersensitivity) response to inhaled organic antigens.
- Examples: Farmer's lung (Saccharopolyspora rectivirgula), Bird fancier's lung (avian proteins).
- Acute: Fever, cough, dyspnea 4-8 hrs post-exposure; reversible. Chronic: Insidious onset, progressive dyspnea, irreversible fibrosis; non-caseating granulomas.
⭐ In asbestosis, bronchogenic carcinoma is a more common malignancy than mesothelioma, especially with co-existing smoking (synergistic effect).
Systemic & Other RLDs - Wider Connections
- Connective Tissue Diseases (CTDs) causing RLD:
- Systemic Sclerosis (Scleroderma): Most common CTD to cause ILD (NSIP pattern common).
- Rheumatoid Arthritis (RA): Usual Interstitial Pneumonia (UIP) pattern common; Caplan syndrome (RA + pneumoconiosis).
- Systemic Lupus Erythematosus (SLE): Pleuritis, pleural effusions, acute lupus pneumonitis, diffuse alveolar hemorrhage, shrinking lung syndrome.
- Polymyositis/Dermatomyositis: NSIP, organizing pneumonia.
- Sjögren's Syndrome: Lymphocytic interstitial pneumonia (LIP).
- Drug-Induced RLDs:
- Amiodarone: Pneumonitis, fibrosis.
- Bleomycin: Dose-dependent pneumonitis, fibrosis.
- Methotrexate: Hypersensitivity pneumonitis.
- Nitrofurantoin: Acute pneumonitis, chronic fibrosis.
- 📌 Mnemonic: "Bad Air Makes No Lungs Happy" (Bleomycin, Amiodarone, Methotrexate, Nitrofurantoin, Lomustine (CCNU), Heroin)
- Radiation-Induced Lung Disease:
- Radiation Pneumonitis: Acute (1-6 months post-radiation); lymphocytic alveolitis.
- Radiation Fibrosis: Chronic (>6-12 months post-radiation); dense fibrosis.

⭐ Amiodarone lung toxicity classically shows foamy macrophages on BAL or biopsy due to phospholipidosis, and high-attenuation areas on CT scan due to iodine content.
- Other Causes:
- Neurofibromatosis
- Tuberous Sclerosis (LAM - Lymphangioleiomyomatosis)
- Graft-versus-Host Disease (GVHD) post-transplant (Bronchiolitis Obliterans).
High‑Yield Points - ⚡ Biggest Takeaways
- Restrictive diseases: ↓ lung volumes (↓TLC, ↓FVC), normal/↑ FEV1/FVC ratio.
- IPF: Usual Interstitial Pneumonia (UIP) pattern, honeycomb lung on HRCT.
- Sarcoidosis: Non-caseating granulomas, bilateral hilar lymphadenopathy, ↑ACE.
- Pneumoconioses: Caused by inorganic dust inhalation (e.g., silica, asbestos), leading to fibrosis.
- Asbestosis: Associated with pleural plaques, ↑ risk of mesothelioma and bronchogenic carcinoma.
- Hypersensitivity Pneumonitis: Immune reaction to inhaled organic antigens (e.g., farmer's lung).
- ARDS: Characterized by Diffuse Alveolar Damage (DAD) and hyaline membrane formation.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

