Glomerular Structure & Injury - Filtration Fortress Facts
- Components: Endothelium (fenestrated), GBM (collagen IV, negative charge), Podocytes (foot processes, slit diaphragms - nephrin), Mesangium (support).
- Filtration Barrier: Size & charge selective (restricts albumin).

- Injury Mechanisms:
- Immune Complexes: Subepithelial (MN), subendothelial (LN, MPGN), mesangial (IgAN).
- Anti-GBM Disease: Linear IgG (Goodpasture's).
- Pauci-immune: ANCA-associated.
- Cell-mediated.
⭐ The GBM's negative charge (heparan sulfate) is crucial for repelling albumin.
Nephrotic Syndrome - The Great Protein Leak
-
Hallmarks:
- Proteinuria ($>$ 3.5g/24h)
- Hypoalbuminemia ($<$ 3 g/dL)
- Edema
- Hyperlipidemia/Lipiduria
- 📌 PALE H: Proteinuria, Albumin low, Lipids high, Edema, Hypercoagulability.
-
Key Diseases & Biopsy:
-
Minimal Change Disease (MCD):
- Children; excellent steroid response.
- LM: Normal. IF: Negative.
- EM: Diffuse podocyte foot process effacement.
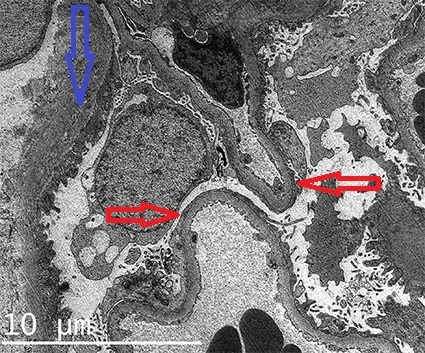
-
Focal Segmental Glomerulosclerosis (FSGS):
- LM: Segmental sclerosis. IF: Often negative (may be IgM, C3).
- EM: Foot process effacement.
- Assoc: HIV, heroin, obesity.
-
Membranous Nephropathy (MN):
- Adults; PLA2R Ab.
- LM: Thick GBM. IF: Granular IgG, C3.
- EM: Subepithelial deposits ("spike & dome").
- Assoc: HBV, HCV, SLE, malignancy.
-
Diabetic Nephropathy:
- LM: Mesangial expansion, Kimmelstiel-Wilson nodules.
- EM: Thick GBM.
- Most common ESRD cause.
-
⭐ Kimmelstiel-Wilson nodules are pathognomonic for diabetic nephropathy.
Nephritic Syndrome - Fiery Filter Fight
-
Definition: Hematuria (RBC casts, cola-urine), Oliguria, Hypertension (HTN), Azotemia, Mild proteinuria (<3.5g/d).
-
Post-Streptococcal GN (PSGN):
- LM: Diffuse proliferative GN, hypercellular.
- IF: Granular IgG, C3 ("lumpy-bumpy").
- EM: Subepithelial humps.
- Clinical: Post-strep infection (pharyngitis/impetigo), ↓C3.
- ⭐ > PSGN: Classic subepithelial humps on EM; C3 typically recovers in 6-8 weeks.
-
IgA Nephropathy (Berger's Disease):
- LM: Mesangial proliferation.
- IF/EM: Mesangial IgA deposits.
- Clinical: Episodic gross hematuria, often with URI/GI infection. Most common GN. Normal C3.

-
Rapidly Progressive GN (RPGN):
- LM: Crescent formation in Bowman's space. Rapid renal failure.
- 📌 RPGN Types (1-2-3):
- Type I: Anti-GBM (Goodpasture's) - Linear IF.
- Type II: Immune Complex (e.g., PSGN, IgA, Lupus) - Granular IF.
- Type III: Pauci-Immune (ANCA-associated) - Negative IF.
-
%%{init: {'flowchart': {'htmlLabels': true}}}%% flowchart TD
Start["🩺 RPGN Diagnosis
• Crescents on LM• Rapid renal loss"]
IF["🔬 IF Pattern
• Immunofluorescence• Staining pattern"]
Type1["🩺 Type I Disease
• Anti-GBM disease• Goodpasture synd."]
Type2["🩺 Type II Disease
• Immune complexes• PSGN, IgA, Lupus"]
Type3["🩺 Type III Disease
• ANCA-associated• GPA or MPA"]
Start --> IF IF -->|Linear IgG| Type1 IF -->|Granular| Type2 IF -->|Pauci-Immune| Type3
style Start fill:#F7F5FD, stroke:#F0EDFA, stroke-width:1.5px, rx:12, ry:12, color:#6B21A8 style IF fill:#FFF7ED, stroke:#FFEED5, stroke-width:1.5px, rx:12, ry:12, color:#C2410C style Type1 fill:#F7F5FD, stroke:#F0EDFA, stroke-width:1.5px, rx:12, ry:12, color:#6B21A8 style Type2 fill:#F7F5FD, stroke:#F0EDFA, stroke-width:1.5px, rx:12, ry:12, color:#6B21A8 style Type3 fill:#F7F5FD, stroke:#F0EDFA, stroke-width:1.5px, rx:12, ry:12, color:#6B21A8
* **Lupus Nephritis (LN):** (Nephritic forms)
- Class III (Focal Proliferative GN), Class IV (Diffuse Proliferative GN - most common/severe).
- LM (Class IV): "Wire-loop" lesions.
- IF: "Full house" (IgG, IgA, IgM, C3, C1q). EM: Subendothelial deposits.
## Glomerular Biopsy Interpretation - Glomerular Detective Work
* **Immunofluorescence (IF)**:
* Linear: IgG along GBM (e.g., Anti-GBM disease).
* Granular (Immune complexes):
+ Mesangial (e.g., IgA Nephropathy).
+ Subepithelial (e.g., Membranous Nephropathy - "spikes & domes").
+ Subendothelial (e.g., Lupus Nephritis - "wire loops").
* **Electron Microscopy (EM)**:
* Deposits: Location (subepithelial, subendothelial, mesangial, intramembranous), density.
* Foot process effacement (common in proteinuria).
* GBM: Thickening, thinning, splitting (e.g., "basket-weave" in Alport).
* **Alport Syndrome**: ***COL4A5*** defect (Type IV collagen); hematuria, sensorineural deafness, ocular defects (lenticonus). EM: GBM splitting/lamellation ("basket-weave" appearance).
* **Thin Basement Membrane Disease**: Benign familial hematuria; diffuse GBM thinning on EM.
> ⭐ Pauci-immune glomerulonephritis (e.g., ANCA-associated vasculitis) shows minimal or no immune deposits on IF, despite active glomerular inflammation (glomerular crescents may be present).
## High‑Yield Points - ⚡ Biggest Takeaways
> * **Nephrotic Syndrome**: **Proteinuria >3.5g/day**, hypoalbuminemia, edema, hyperlipidemia.
> * **Minimal Change Disease**: Top nephrotic cause in **children**; **podocyte effacement** on EM.
> * **FSGS**: Key nephrotic syndrome in **adults**; linked to **HIV, sickle cell, obesity**.
> * **Membranous Nephropathy**: **Subepithelial "spike and dome" deposits**; common adult nephrotic cause.
> * **Nephritic Syndrome**: **Hematuria (RBC casts)**, oliguria, hypertension, mild proteinuria.
> * **PSGN**: Post-strep nephritic syndrome; EM shows **subepithelial "humps"**.
> * **IgA Nephropathy**: **World's most common GN**; **mesangial IgA deposits** on IF.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

