PNETs Overview - Pancreatic Powerhouses
- Pancreatic Neuroendocrine Tumors (PNETs): Originate from pancreatic islet cells.
- WHO 2019/2022 Classification & Grading:
- Well-differentiated PNET (morphology preserved):
- G1: Mitoses <2/10 HPF AND Ki-67 <3%
- G2: Mitoses 2-20/10 HPF OR Ki-67 3-20%
- G3: Mitoses >20/10 HPF OR Ki-67 >20%
- Poorly-differentiated Neuroendocrine Carcinoma (NEC G3): High grade, poor morphology, Ki-67 often >55%.
- MiNEN (Mixed Neuroendocrine-Non-neuroendocrine Neoplasm).
- Well-differentiated PNET (morphology preserved):
- Functional (hormone-secreting, e.g., Insulinoma, Gastrinoma) vs. Non-functional (more common, present with mass effects).
⭐ Most PNETs are well-differentiated tumors (G1/G2), but Ki-67 index and mitotic count are crucial for grading and prognosis.
Functional PNETs: Insulinoma & Gastrinoma - Sweet & Sour Syndromes
-
Insulinoma ("Sweet")
- Most common PNET; β-cell origin; secretes insulin → hypoglycemia.
- Whipple's Triad:
- Hypoglycemic symptoms.
- Plasma glucose <50 mg/dL.
- Relief with glucose.
- Dx: ↑Insulin, ↑C-peptide with hypoglycemia (72-hr fast).
- ~90% benign, solitary. Tx: Surgery.
-
Gastrinoma ("Sour") - Zollinger-Ellison Syndrome (ZES)
- G-cell origin (pancreas/duodenum); secretes gastrin → ↑HCl.
- Clinical: Refractory/multiple peptic ulcers (PUDs), diarrhea.
- Dx:
- ↑Fasting gastrin (>1000 pg/mL with gastric pH <2).
- Positive Secretin stimulation test (paradoxical ↑gastrin).
- ~25% MEN1 associated. >60% malignant.
- Tx: PPIs, surgery.
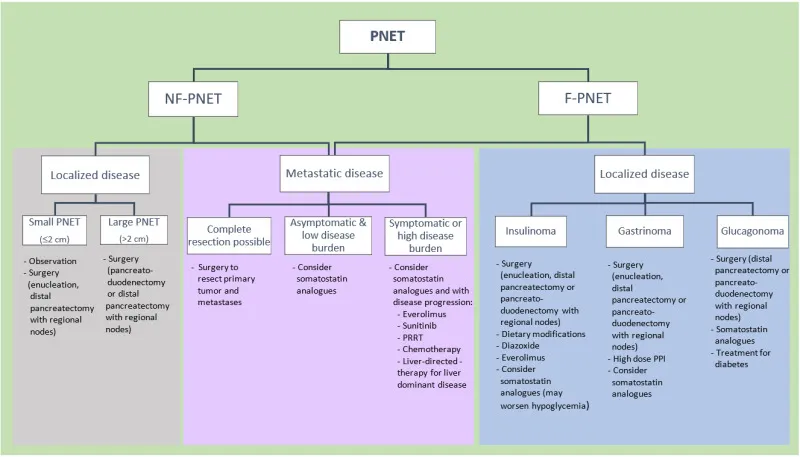
⭐ Insulinomas are typically benign (~90%) and solitary, presenting with Whipple's triad, while gastrinomas (ZES) are often malignant, multiple, and associated with MEN1.
Other Functional PNETs - Rare Hormone Havoc
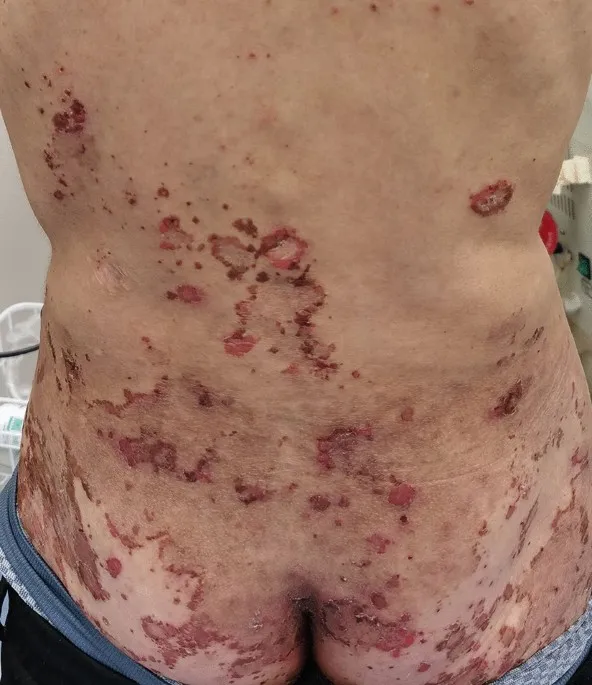
- Glucagonoma:
- Presents with syndrome: Diabetes, Dermatitis (necrolytic migratory erythema), DVT, Depression (📌 4Ds).
- ↑ Glucagon. Often in pancreatic tail. High malignant potential.
⭐ Glucagonoma syndrome classically presents with the '4Ds': Dermatitis (necrolytic migratory erythema), Diabetes, DVT, and Depression.
- VIPoma (Verner-Morrison Syndrome):
- Causes WDHA syndrome: Watery Diarrhea, Hypokalemia, Achlorhydria ("Pancreatic Cholera").
- ↑ VIP. Often in pancreatic tail. ~50% malignant.
⭐ VIPomas cause WDHA syndrome (Watery Diarrhea, Hypokalemia, Achlorhydria).
- Somatostatinoma:
- Syndrome: Diabetes mellitus, cholelithiasis, steatorrhea, hypochlorhydria.
- ↑ Somatostatin. Often duodenal or pancreatic. Psammoma bodies common.
- PPoma (Pancreatic Polypeptide-oma):
- Often clinically silent or presents with vague symptoms. ↑ Pancreatic Polypeptide.
PNETs: Diagnosis & Management - Spotting & Stopping
-
Diagnosis
- Clinical Suspicion: Symptoms (hormonal/mass) or incidental finding.
- Biochemical Markers:
- Specific hormone assays.
- General: Chromogranin A (CgA), Synaptophysin (IHC markers).
- Imaging:
- CT/MRI (initial).
- EUS-FNA (biopsy).
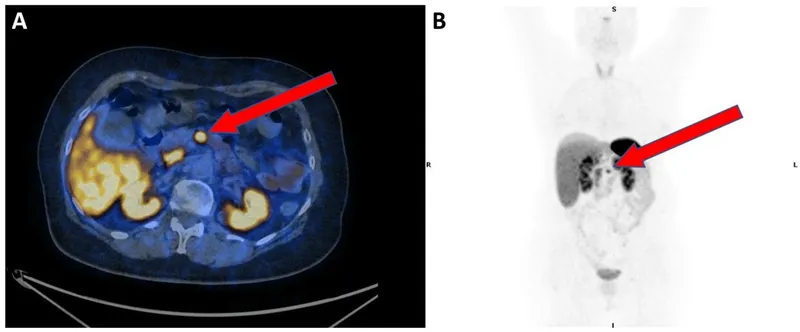
- Functional: Ga-68 DOTATATE PET/CT (best for staging/localization) or Octreoscan.
⭐ Chromogranin A and Synaptophysin are key immunohistochemical markers for PNETs. Somatostatin receptor scintigraphy (Octreoscan) or Ga-68 DOTATATE PET/CT are crucial for localization and staging.
-
Management
- Surgery: Primary treatment for localized PNETs; curative intent.
- Medical Management (for unresectable/metastatic disease):
- SSAs (Octreotide, Lanreotide): Control symptoms, inhibit growth.
- Targeted Therapy: Everolimus (mTORi), Sunitinib (TKI).
- PRRT: Lu-177 DOTATATE for SSTR-positive tumors.
- Chemotherapy (e.g., Streptozocin, Temozolomide): Poorly differentiated/high-grade.
High‑Yield Points - ⚡ Biggest Takeaways
- Insulinoma: Most common PNET, causes hypoglycemia (Whipple's triad); often benign.
- Gastrinoma (ZES): Leads to multiple, refractory peptic ulcers; strong MEN 1 association.
- Glucagonoma: Presents with necrolytic migratory erythema, diabetes, DVT, depression (4Ds).
- VIPoma: Characterized by WDHA syndrome (Watery Diarrhea, Hypokalemia, Achlorhydria).
- Somatostatinoma: Causes inhibitory effects: diabetes, cholelithiasis, steatorrhea, hypochlorhydria.
- MEN 1 syndrome is frequently linked with gastrinomas, insulinomas, and glucagonomas.
- Chromogranin A & Synaptophysin are key immunohistochemical markers for PNETs.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more


