Peripheral Nerve Disorders: Injury Patterns - Shocking Revelations
- Nerve Fiber Components: Axon, Myelin sheath (Schwann cells in PNS), Connective tissues (Endoneurium, Perineurium, Epineurium).
- Key Injury Responses:
- Wallerian Degeneration: Occurs distal to axonal transection or severe crush.
- Axon & myelin breakdown; phagocytosis by macrophages.
- Central chromatolysis (cell body swelling, Nissl dispersion).
- Proximal stump attempts regeneration (axonal sprouting).
- Segmental Demyelination: Myelin loss with axon preservation.
- Caused by Schwann cell dysfunction/damage (e.g., Guillain-Barré Syndrome, diphtheria toxin).
- Results in ↓ conduction velocity; remyelination is possible.
- Axonal Degeneration (Dying-back Neuropathy): Distal parts of axon degenerate first, progressing proximally.
- Often due to metabolic derangements or toxic exposures.
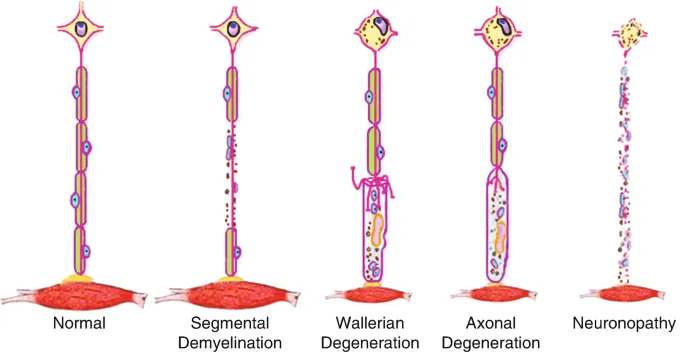
- Often due to metabolic derangements or toxic exposures.
- Wallerian Degeneration: Occurs distal to axonal transection or severe crush.
⭐ Sunderland Classification (Grades I-V) is crucial for categorizing nerve injury severity, directly impacting prognosis and guiding management. Grade I (neurapraxia) involves temporary conduction block with full recovery.
Peripheral Nerve Disorders: Inflammatory - Immune System Mayhem
- Guillain-Barré Syndrome (GBS)
- Acute inflammatory demyelinating polyradiculoneuropathy (AIDP).
- Rapidly progressive, ascending symmetrical weakness/paralysis; often post-infectious (e.g., Campylobacter jejuni due to molecular mimicry).
- CSF: ↑ Protein (albuminocytologic dissociation), normal cells after 1st week.
- Variant: Miller Fisher Syndrome (ophthalmoplegia, ataxia, areflexia).
- Treatment: IVIg, plasmapheresis. Steroids NOT effective.
- Chronic Inflammatory Demyelinating Polyneuropathy (CIDP)
- Chronic (>8 weeks), progressive or relapsing-remitting sensorimotor neuropathy.
- Symmetrical proximal & distal weakness, sensory loss.
- Nerve biopsy:
Peripheral Nerve Disorders: Metabolic & Hereditary - Sweet & Inherited Woes
-
Diabetic Neuropathy: Most common metabolic neuropathy.
- Pathogenesis: Advanced glycation end-products (AGEs), sorbitol accumulation, oxidative stress, microangiopathy.
- Patterns:
- Distal Symmetrical Polyneuropathy (DSPN): "Stocking-glove" sensory loss (most common).
- Autonomic Neuropathy: Gastroparesis, orthostatic hypotension.
- Mononeuropathies: Cranial nerves (CN III, VI), focal limb.
- Morphology: Axonal degeneration, segmental demyelination, endoneurial arteriolar hyalinization.
-
Hereditary Sensory & Motor Neuropathies (HSMN) / Charcot-Marie-Tooth (CMT):
- CMT1 (AD): Demyelinating. PMP22 gene duplication (1A) most common.
- Features: ↓ Nerve Conduction Velocity (NCV), palpable nerves, pes cavus, "stork leg" deformity.
- Morphology: "Onion bulb" formations (repetitive demyelination & remyelination).
- CMT2 (AD): Axonal. Normal/mildly ↓ NCV. MFN2 mutations common.
- CMTX (X-linked): Demyelinating. GJB1 (connexin-32) mutations.
- Hereditary Neuropathy with liability to Pressure Palsies (HNPP): PMP22 deletion. Recurrent focal neuropathies. Tomacula ("sausage-like" myelin thickenings).
- CMT1 (AD): Demyelinating. PMP22 gene duplication (1A) most common.
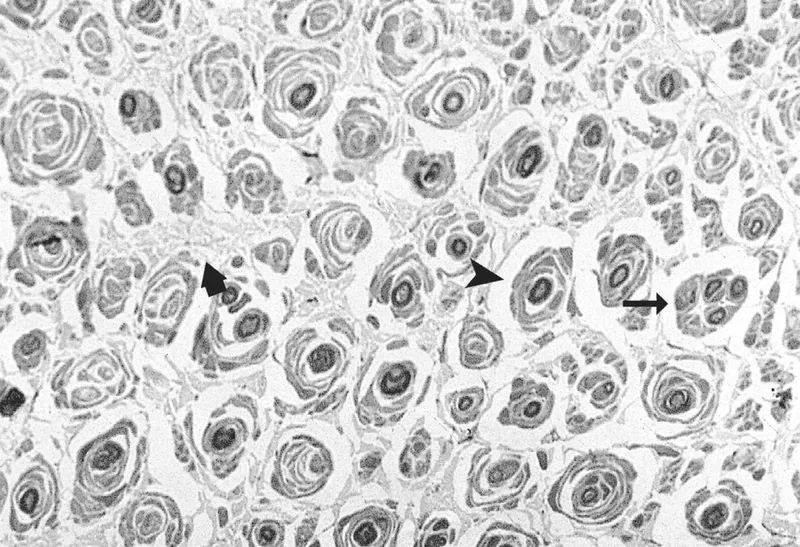
⭐ CMT1A, due to PMP22 gene duplication, is the most common inherited neuropathy, characterized by hypertrophic "onion bulb" Schwann cell changes visible on biopsy.
Peripheral Nerve Disorders: Other Key Types - Traps, Toxins & Bugs
- Entrapment Neuropathies (Traps):
- Carpal Tunnel Syndrome (CTS): Median nerve at wrist; Phalen's, Tinel's signs.
- Saturday Night Palsy: Radial nerve compression (spiral groove); wrist drop.
- Meralgia Paresthetica: Lateral femoral cutaneous nerve under inguinal ligament.
- Tarsal Tunnel Syndrome: Tibial nerve compression at ankle.
- Toxic Neuropathies:
- Lead: Predominantly motor neuropathy; wrist drop, foot drop.
- Arsenic: Painful sensorimotor neuropathy; Mees' lines on nails.
- Alcohol: Chronic use; axonal degeneration, painful sensory > motor.
- Drugs: Isoniazid (give B6), Vincristine, Amiodarone.
- Infectious Neuropathies (Bugs):
- Leprosy (Hansen's Disease): M. leprae; affects cool areas, palpable thickened nerves, sensory loss.
⭐ Leprosy is a major global cause of peripheral neuropathy, with characteristic anaesthetic skin patches and thickened nerves.
- Diphtheria: C. diphtheriae exotoxin; bulbar palsy, polyneuropathy.
- Lyme Disease: B. burgdorferi; facial nerve palsy (often bilateral).
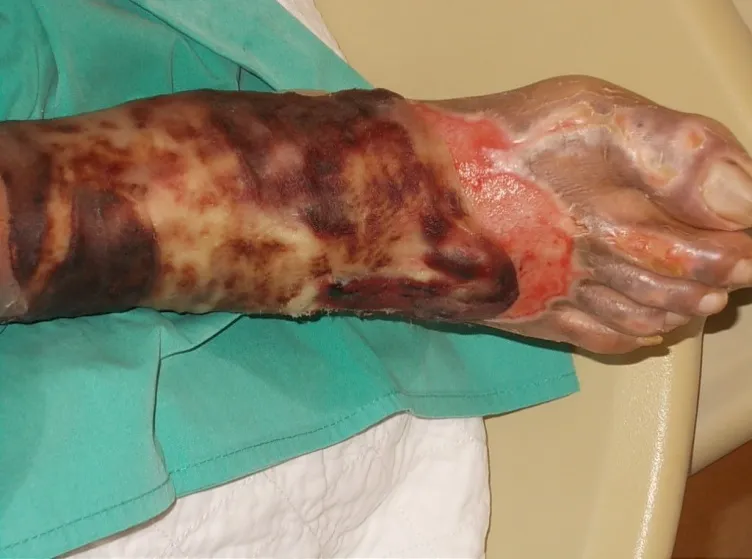
- Leprosy (Hansen's Disease): M. leprae; affects cool areas, palpable thickened nerves, sensory loss.
High‑Yield Points - ⚡ Biggest Takeaways
- Guillain-Barré syndrome: Acute inflammatory demyelinating polyradiculoneuropathy (AIDP), ascending paralysis, albumino-cytological dissociation in CSF.
- Charcot-Marie-Tooth disease (CMT1A): PMP22 duplication, hereditary demyelinating neuropathy, pes cavus, onion bulbs.
- Diabetic neuropathy: Most common; distal symmetric polyneuropathy ("stocking-glove"), axonal degeneration and demyelination.
- Leprosy: M. leprae infects Schwann cells; Tuberculoid (localized) vs. Lepromatous (widespread anesthesia).
- Wallerian degeneration: Anterograde axonal degeneration distal to injury; forms myelin ovoids.
- Lead neuropathy: Predominantly motor neuropathy, causing wrist drop and foot drop.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

