Neural Tube Defects - Tube Trouble Tales
- Failure of neural tube closure (3rd-4th week gestation).
- Key risk: Maternal folate deficiency. Others: valproate, maternal diabetes.
- Types:
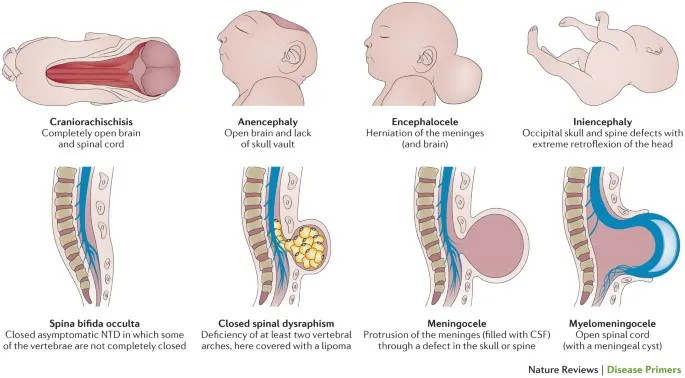
- Anencephaly: Anterior neuropore. "Frog-like" appearance. Polyhydramnios.
- Spina Bifida (posterior neuropore):
- Occulta: Vertebral defect, tuft of hair. AFP normal.
- Meningocele: Meninges herniate.
- Meningomyelocele: Meninges + neural tissue. Neurological deficits.
- Encephalocele: Brain/meninges herniation through skull defect.
- Diagnosis: ↑ maternal serum AFP (MSAFP), ↑ amniotic fluid AFP & AChE (except occulta). Ultrasound.
- Prevention: Folic acid (0.4 mg/day; 4 mg/day high-risk).
⭐ Maternal folate deficiency is a major risk factor for Neural Tube Defects.
Forebrain Anomalies - Brain Building Blocks
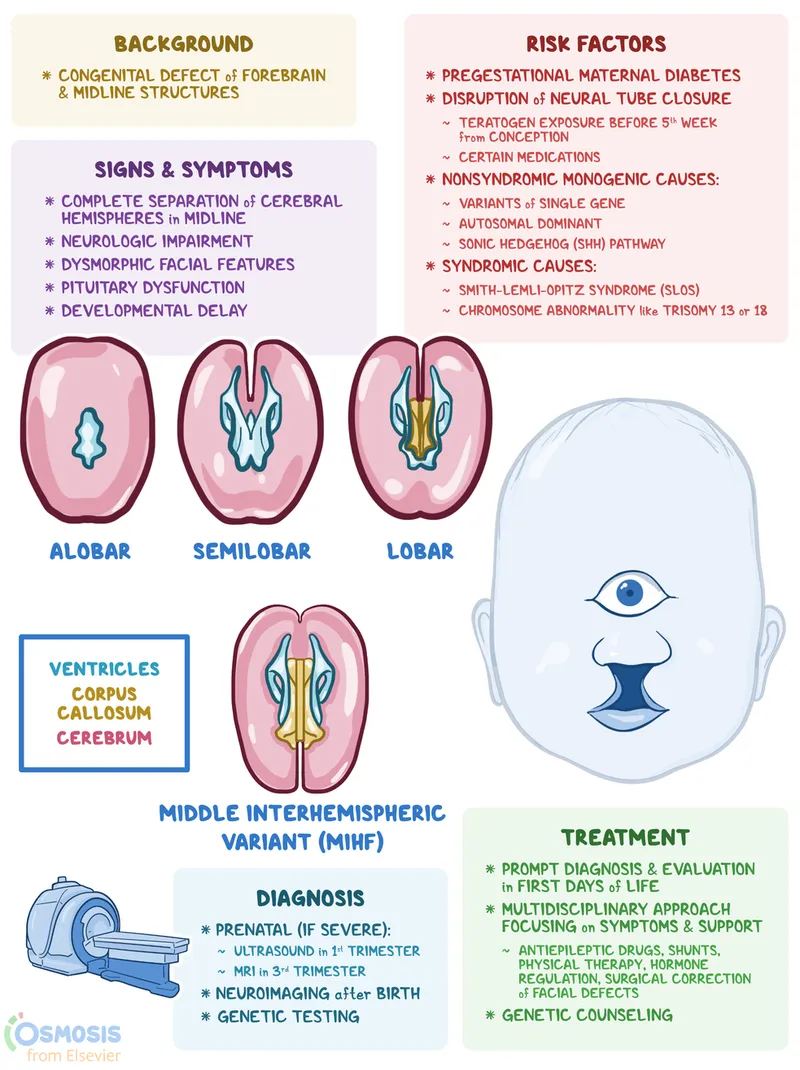
- Holoprosencephaly (HPE): Failure of forebrain (prosencephalon) cleavage.
- Spectrum: Alobar (severe) → Semilobar → Lobar.
- Associations: Trisomy 13, SHH gene, maternal diabetes.
- Facial: Cyclopia, proboscis.
⭐ Holoprosencephaly is strongly associated with Trisomy 13 (Patau syndrome).
- Lissencephaly (Smooth Brain): Agyria/Pachygyria.
- Neuronal migration defect.
- Type 1: LIS1, DCX. Type 2 (Cobblestone): e.g., Walker-Warburg.
- Polymicrogyria: Multiple small gyri; neuronal migration issue.
- Causes: Genetic, CMV.
- Schizencephaly: Gray matter-lined clefts in hemispheres. EMX2 gene.
- Megalencephaly/Hemimegalencephaly: Enlarged brain/hemisphere; mTOR pathway.
Posterior Fossa Anomalies - Hindbrain Headaches
- Chiari Malformations: Cerebellar tissue herniation. Often cause occipital headaches.
- Type I: Tonsils >5mm below foramen magnum. Adults. Syringomyelia, headaches.
- Type II (Arnold-Chiari): Vermis, tonsils, medulla, 4th ventricle herniation. Infants. Hydrocephalus.
⭐ Chiari II malformation is almost invariably associated with a lumbar myelomeningocele.
- Type III: Rare. Occipital/cervical encephalocele + cerebellar herniation.
- Type IV: Severe cerebellar hypoplasia/aplasia.
- Dandy-Walker Malformation (DWM):
- Agenesis/hypoplasia of cerebellar vermis.
- Cystic dilation of 4th ventricle; enlarged posterior fossa.
- Hydrocephalus common. 📌 DWM: Dilated 4th, Water (hydrocephalus), Missing vermis.
- Joubert Syndrome:
- Vermis agenesis/hypoplasia.
- "Molar tooth sign" on MRI (superior cerebellar peduncles).
- Hypotonia, ataxia, developmental delay, abnormal breathing.

Hydrocephalus & Syringomyelia - Fluid Flow Faults
- Hydrocephalus: Increased CSF volume leading to ventricular dilation.
- Communicating: Impaired CSF absorption (e.g., post-meningitis scarring).
- Non-communicating (Obstructive): CSF flow blocked within ventricular system or its outlets (e.g., aqueductal stenosis).
⭐ Congenital aqueductal stenosis is the most common cause of non-communicating hydrocephalus in newborns.
- Normal Pressure Hydrocephalus (NPH): Affects elderly; triad: Wet (urinary incontinence), Wobbly (gait ataxia), Wacky (dementia). 📌
- Clinical (Infants): Bulging fontanelles, rapidly increasing head circumference, sunsetting eyes.
- Clinical (Adults): Headache, nausea, vomiting, papilledema.
- Syringomyelia: Fluid-filled cavity (syrinx) within the spinal cord, typically cervical; involves central canal dilation.
- Associations: Chiari I malformation, trauma, tumors.
- Clinical: Classic "cape-like" bilateral loss of pain and temperature sensation in upper extremities (damage to spinothalamic fibers crossing in anterior white commissure); preserved touch. Late: motor deficits (LMN signs).
High‑Yield Points - ⚡ Biggest Takeaways
- Neural tube defects (NTDs) like anencephaly and spina bifida are linked to folate deficiency.
- Arnold-Chiari II involves cerebellar herniation, hydrocephalus, and myelomeningocele.
- Dandy-Walker malformation shows absent cerebellar vermis and a cystic 4th ventricle.
- Syringomyelia (spinal cord syrinx) is often associated with Chiari I and "cape-like" sensory loss.
- Holoprosencephaly (failed forebrain division) is linked to Trisomy 13 and SHH mutations.
- Lissencephaly ("smooth brain") results from defective neuronal migration.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

