Neuronal Responses - Neuron Under Siege
- Acute Neuronal Injury (Ischemic Cell Change):
- "Red neurons": Eosinophilic cytoplasm, pyknotic nucleus, Nissl loss. Irreversible hypoxic/ischemic injury.
- Cell body, nucleus, nucleolus shrink.
⭐ Red neurons are visible by LM approx. 12‑24 hours post irreversible hypoxic/ischemic insult.
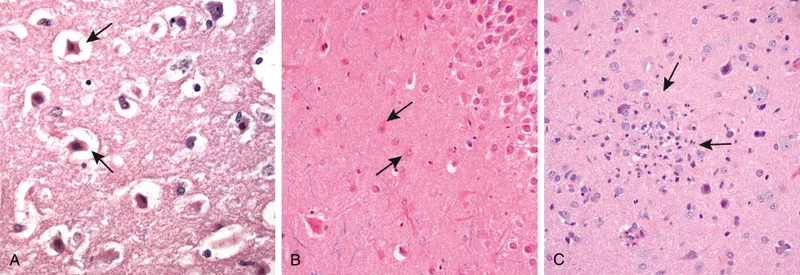
- Subacute & Chronic Neuronal Injury (Degeneration):
- Selective neuronal loss; reactive gliosis (astrocytosis).
- Apoptosis or necrosis.
- Axonal Reaction (Central Chromatolysis):
- Response to axonal injury.
- Cell body swells; Nissl disperses peripherally; nucleus eccentric.
- Neuronal Inclusions:
- Markers of aging, viral infections, neurodegenerative diseases.
- E.g., Lipofuscin (aging), Negri bodies (Rabies), Cowdry bodies (HSV), Lewy bodies (Parkinson's), Neurofibrillary tangles (Alzheimer's).
Glial Reactions - Support Crew's Crisis
- Astrocytes (Astrogliosis/Gliosis): Key CNS injury responders; form glial scars.
- Hypertrophy & hyperplasia; ↑ GFAP.
- Gemistocytic astrocytes: reactive; plump, eosinophilic cytoplasm, eccentric nucleus.
- Corpora amylacea: PAS+, basophilic, laminated polyglucosan bodies; age-related or chronic conditions.
- Alzheimer type II astrocytes: large, clear nucleus (NOT Alzheimer's disease; metabolic encephalopathies e.g., hepatic, Wilson's).
- Oligodendrocytes: Myelin production (CNS).
- Injury → demyelination (MS, PML), apoptosis.
- Inclusions: Glial cytoplasmic inclusions (GCIs) in MSA (α-synuclein).
- Microglia: CNS macrophages (mesodermal).
- Activation: proliferate, rod cells (neurosyphilis, viral encephalitis).
- Form microglial nodules (aggregates around injury/inflammation).
- Phagocytosis → Gitter cells (lipid-laden foamy macrophages).
- Ependymal Cells: Line ventricles & central canal.
- Reaction: ependymal granulations (subependymal astrocyte proliferation), lining loss.
- Viral inclusions (e.g., CMV).
⭐ Rosenthal fibers, thick, eosinophilic, irregular structures in astrocytic processes, are characteristic of long-standing gliosis, pilocytic astrocytoma, and Alexander disease.
Cerebral Edema & Herniation - Brain Under Pressure
-
Cerebral Edema: Abnormal brain fluid.
- Types:
Type Pathophysiology Key Feature Common Causes Vasogenic BBB disruption, ↑ permeability Extracellular fluid Tumors, inflammation, trauma, late ischemia Cytotoxic Cellular swelling (Na⁺/K⁺ pump failure) Intracellular fluid Ischemia, toxins, hyponatremia Interstitial CSF seepage (obstructive hydrocephalus) Periventricular WM Obstructive hydrocephalus Osmotic ↓ Plasma osmolality Global swelling SIADH, rapid dialysis - Clinical: Headache, vomiting, papilledema, altered sensorium.
- Imaging (CT/MRI): Sulcal effacement, ventricular compression.
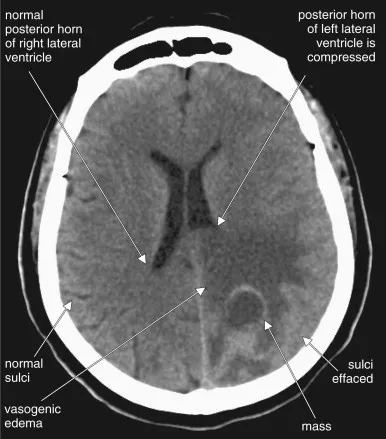
- Types:
-
Brain Herniation: Brain displacement from ↑ ICP.
- Types & Critical Sequelae:
> ⭐ Uncal herniation classically compresses **CN III**, leading to ipsilateral pupillary dilation and oculomotor palsy ('down and out' gaze), and can cause Duret hemorrhages in the brainstem.
High‑Yield Points - ⚡ Biggest Takeaways
- Red neurons: Eosinophilic change, pyknosis; signify acute irreversible neuronal injury (12-24h).
- Central chromatolysis: Axonal reaction; cell body swells, Nissl disperses peripherally.
- Gliosis: CNS scarring; astrocyte hypertrophy/hyperplasia (GFAP+), forms glial scar.
- Rosenthal fibers: Eosinophilic, corkscrew astrocytic processes; seen in pilocytic astrocytoma, Alexander disease.
- Microglial nodules/Neuronophagia: Microglia cluster around dying neurons; common in viral encephalitis.
- Key Inclusions: Negri bodies (rabies), Lewy bodies (Parkinson's), Neurofibrillary tangles (Alzheimer's).
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

