Introduction to Carcinogenesis - The Bad Seed
- Carcinogenesis: The complex, multistep process transforming normal cells into cancer cells.
- Driven by accumulated genetic (DNA mutations) & epigenetic alterations.
- Key Stages:
- Initiation: Rapid, irreversible genetic damage (mutation) by a carcinogen.
- Promotion: Reversible, prolonged clonal expansion of initiated cells; non-mutagenic.
- Progression: Irreversible; further mutations yield malignant phenotype (invasion, metastasis).
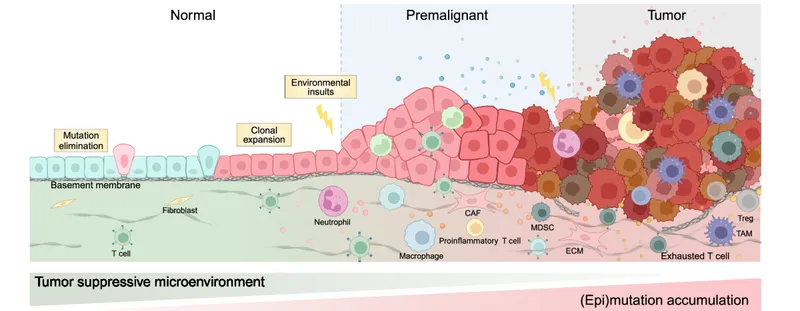
⭐ Most human cancers are of clonal origin, arising from a single genetically altered precursor cell.
Molecular Basis of Cancer - Blueprint for Disaster
- Core principle: Cancer arises from non-lethal genetic damage, leading to uncontrolled cell proliferation.
- Key targets of this damage - four classes of normal regulatory genes:
- Proto-oncogenes: Promote cell growth (e.g., RAS, MYC, HER2). Activation (gain-of-function mutations) converts them to oncogenes.
- Tumor Suppressor Genes (TSGs): Inhibit cell growth or promote DNA repair (e.g., RB, TP53, APC). Inactivation (loss-of-function mutations) contributes to cancer.
- Apoptosis Regulating Genes: Control programmed cell death (e.g., BCL2 family). Alterations lead to evasion of apoptosis (e.g., overexpression of anti-apoptotic BCL2).
- DNA Repair Genes: Maintain genomic integrity (e.g., BRCA1/2, MSH/MLH genes). Inactivation leads to genomic instability (mutator phenotype), accelerating mutation accumulation.
- Carcinogenesis: A multistep process involving accumulation of multiple genetic (mutations) & epigenetic (e.g., methylation) alterations.

⭐ TP53 ("guardian of the genome") is the most commonly mutated gene in human cancers (involved in >50% of cases), critical for cell cycle arrest, DNA repair, and apoptosis induction upon DNA damage. Its inactivation is a major step in many cancers.
Chemical Carcinogenesis - Toxic Triggers
- Direct-acting: No metabolic conversion needed (e.g., alkylating agents).
- Indirect-acting (Procarcinogens): Require metabolic activation, primarily by cytochrome P-450 enzymes.
- Activated forms (ultimate carcinogens) bind DNA, forming DNA adducts → mutations.
- Key Examples & Associated Cancers:
- Polycyclic Aromatic Hydrocarbons (PAHs) (e.g., benzopyrene in tobacco smoke, soot): Lung, skin.
- Aromatic Amines (e.g., $\beta$-naphthylamine): Bladder.
- Aflatoxin B1 (Aspergillus flavus on improperly stored grains): Hepatocellular carcinoma (HCC).
- Nitrosamines (from nitrites in preserved foods): Gastric.
- Vinyl chloride (plastics industry): Liver angiosarcoma.
- Arsenic (contaminated water, pesticides): Skin (squamous cell carcinoma), lung, liver angiosarcoma.
- Asbestos: Lung carcinoma, mesothelioma.
- Nickel, Chromium: Lung.
⭐ Aflatoxin B1, a product of Aspergillus, is a potent natural hepatocarcinogen strongly associated with G:C → T:A transversions in codon 249 of the TP53 gene.
oka
Radiation & Microbial Carcinogenesis - Invisible Invaders
- Radiation:
- UV (Sunlight): Pyrimidine dimers (NER). Cancers: SCC, BCC, Melanoma. Xeroderma Pigmentosum ↑ risk.

- Ionizing (X-rays, nuclear): DNA ds-breaks. Cancers: Leukemia, Thyroid (children), Breast, Lung.
- UV (Sunlight): Pyrimidine dimers (NER). Cancers: SCC, BCC, Melanoma. Xeroderma Pigmentosum ↑ risk.
- Microbial:
- Viruses:
- HPV (16, 18): Cervical Ca (E6→p53↓, E7→Rb↓).
- EBV: Burkitt's (t(8;14)), Nasopharyngeal Ca, Hodgkin's.
- HBV/HCV: HCC (chronic inflammation).
- HTLV-1: ATLL (Tax protein).
- HHV-8: Kaposi Sarcoma.
- Bacteria:
- H. pylori: Gastric AdenoCa, MALT Lymphoma (CagA).
- Viruses:
⭐ EBV links to Burkitt lymphoma via t(8;14) c-myc translocation.
High‑Yield Points - ⚡ Biggest Takeaways
- Chemical carcinogenesis: initiation (DNA damage), promotion (clonal expansion), progression (malignancy).
- Aflatoxin B1 (Aspergillus) causes HCC via TP53 mutation (codon 249).
- HPV 16, 18: E6 degrades p53; E7 inhibits Rb, causing cervical cancer.
- EBV is linked to Burkitt's lymphoma and nasopharyngeal carcinoma.
- UVB radiation causes skin cancer (SCC, BCC, melanoma) via pyrimidine dimers.
- H. pylori is a risk for gastric adenocarcinoma and MALT lymphoma.
- Vinyl chloride → hepatic angiosarcoma; Asbestos → mesothelioma, lung cancer.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

