Overview & Components - First Line Defenders
- Nature: Rapid, non-specific, immediate defense. Present from birth; no memory.
- Function: Prevents pathogen entry/colonization. Recognizes PAMPs (Pathogen-Associated Molecular Patterns) via PRRs (Pattern Recognition Receptors).
- First Line Barriers:
- Physical/Mechanical:
- Intact skin (keratin, desquamation) & mucous membranes (mucus, cilia).
- Flushing actions: Tears, saliva, urine, coughing, sneezing.
- Chemical:
- Lysozyme: In tears, saliva, nasal secretions; targets peptidoglycan.
- Gastric acid: Low pH (e.g., pH 1.5-3.5) in stomach.
- Defensins & Cathelicidins: Antimicrobial peptides on epithelial surfaces.
- Sebum & Lactic acid: Skin surface.
- Biological:
- Normal flora (microbiota): Competitive exclusion, produce bacteriocins.
- Physical/Mechanical:
⭐ Toll-like Receptors (TLRs), a major PRR family, recognize diverse PAMPs: LPS (Gram-negative bacteria) by TLR4, flagellin by TLR5, viral dsRNA by TLR3.

Recognition & Signaling - Stranger Danger Detectors
- Pattern Recognition Receptors (PRRs): Detect conserved microbial molecules (PAMPs) & endogenous danger signals (DAMPs).
- PAMPs (Pathogen-Associated Molecular Patterns): E.g., LPS (Gram -ve bacteria), peptidoglycan, viral RNA.
- DAMPs (Damage-Associated Molecular Patterns): E.g., HMGB1, ATP, uric acid from stressed/necrotic cells.
- Major PRR Families & Key Examples:
- TLRs (Toll-like Receptors): Cell surface & endosomes. E.g., TLR4 recognizes LPS; TLR3, 7, 8, 9 recognize nucleic acids.
- NLRs (NOD-like Receptors): Cytosolic. Some form inflammasomes (e.g., NLRP3).
- RLRs (RIG-I-like Receptors): Cytosolic. Detect viral RNA.
- CLRs (C-type Lectin Receptors): Cell surface. Bind fungal glycans.
- Signaling Outcomes: PRR activation → triggers intracellular signaling (e.g., NF-κB, IRFs) → production of:
- Pro-inflammatory cytokines (e.g., TNF, IL-1, IL-6)
- Type I Interferons (IFN-α/β)
- Chemokines

⭐ NLRP3 inflammasome (an NLR complex) is activated by diverse stimuli including microbial products, crystals (e.g., uric acid in gout), and other DAMPs, leading to caspase-1 activation and secretion of IL-1β and IL-18.
Phagocytosis & Inflammation - The Clean-Up Crew
- Phagocytosis: Cell eating by phagocytes (Neutrophils, Macrophages).
- Process:
- Chemotaxis/Adherence: Opsonins (C3b, IgG Fc) enhance.
- Ingestion: Pseudopods → Phagosome.
- Fusion: Phagosome + Lysosome → Phagolysosome.
- Killing/Digestion:
- Oxygen-dependent: Respiratory burst (NADPH oxidase: $O_2 \rightarrow O_2^-$); Myeloperoxidase (MPO): $H_2O_2 + Cl^- \rightarrow HOCl$.
- Oxygen-independent: Lysozyme, lactoferrin, defensins.
- Process:
- Inflammation: Response to eliminate cause & consequence of injury.
- Cardinal Signs: Rubor (redness), Tumor (swelling), Calor (heat), Dolor (pain), Functio laesa (loss of function). 📌 PRISH.
- Key Vascular Events: Vasodilation (histamine, NO), ↑ permeability (histamine, leukotrienes).
- Key Cellular Events: Leukocyte recruitment (margination, rolling, adhesion, transmigration). Chemotaxins: C5a, LTB4, IL-8.
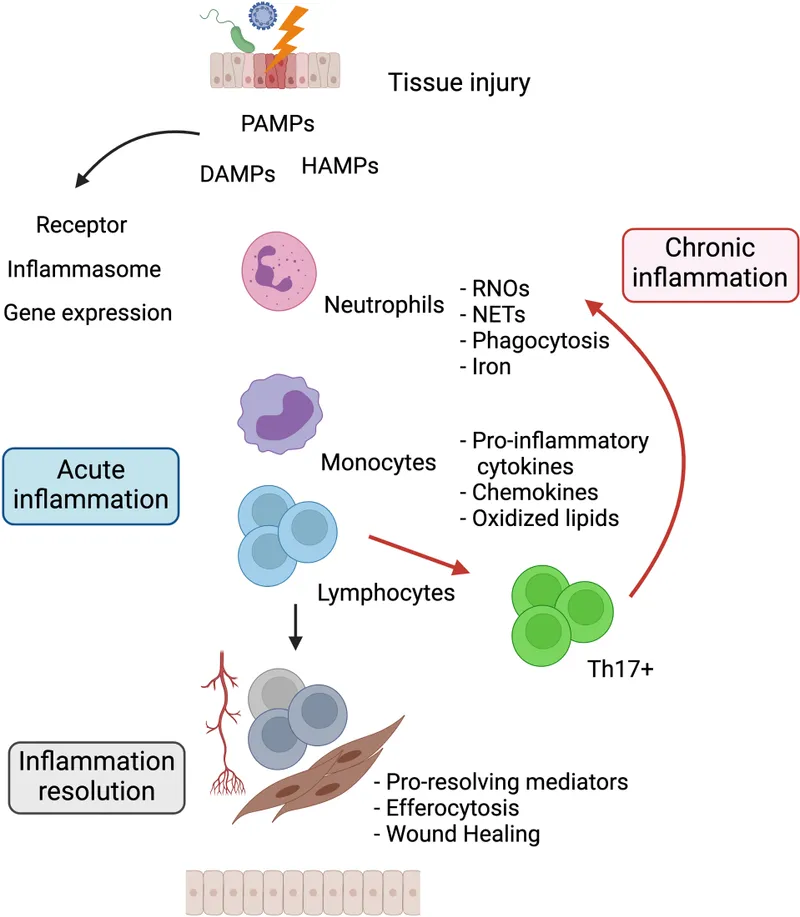
⭐ Chronic Granulomatous Disease (CGD): Defect in NADPH oxidase (impaired oxygen killing). Recurrent infections by catalase-positive organisms (e.g., S. aureus, Aspergillus).
NK Cells, IFN & Complement - Special Ops & Body Alarms
- NK Cells (CD16/CD56+): Innate lymphoid cells; cytotoxic.
- Target: Virus-infected & tumor cells (↓MHC-I - "missing self" or stress ligand expression).
- Kill via: Perforin, Granzymes.
- ADCC: CD16 (FcγRIII) binds IgG.
- Interferons (IFN): Cytokine alarms.
- Type I (α, β): By most cells. Induce antiviral state; ↑MHC I.
- Type II (γ): By NK, T cells. Activates macrophages; ↑MHC expression.
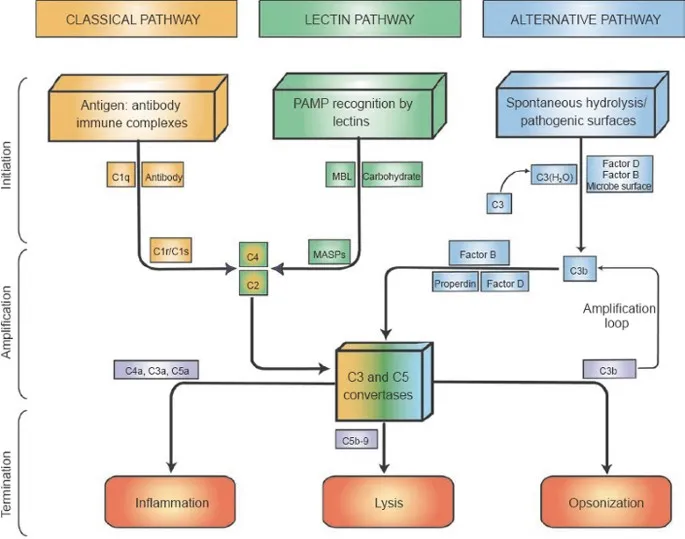
- Complement System: Plasma protein cascade.
- Pathways converge at C3 convertase:
- Key Functions:
- Opsonization: **C3b**.
- Lysis: MAC (**C5b-C9**).
- Inflammation/Chemotaxis: **C3a, C5a** (anaphylatoxins).
- 📌 **Mnemonic (Functions):** O-L-I-C (Opsonization, Lysis, Inflammation, Clearance).
> ⭐ **C3b** is the central molecule and major opsonin of the complement system.
High‑Yield Points - ⚡ Biggest Takeaways
- Innate immunity: First line of defense, rapid, non-specific, no immunological memory.
- Key cells: Neutrophils, macrophages (phagocytosis); NK cells (cytotoxicity); dendritic cells, mast cells.
- PRRs (e.g., TLRs, NLRs) recognize PAMPs (e.g., LPS from bacteria) & DAMPs.
- Mediators: Cytokines (TNF-α, IL-1, IL-6), chemokines, interferons; complement system.
- NK cells kill virus-infected/tumor cells without prior sensitization using perforins/granzymes.
- Acute Phase Reactants (e.g., CRP, SAA) are systemic markers of acute inflammation.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

