Hypersensitivity Intro - Immune Overdrive
- Definition: Exaggerated immune response to an antigen (allergen), causing inflammation and host tissue damage.
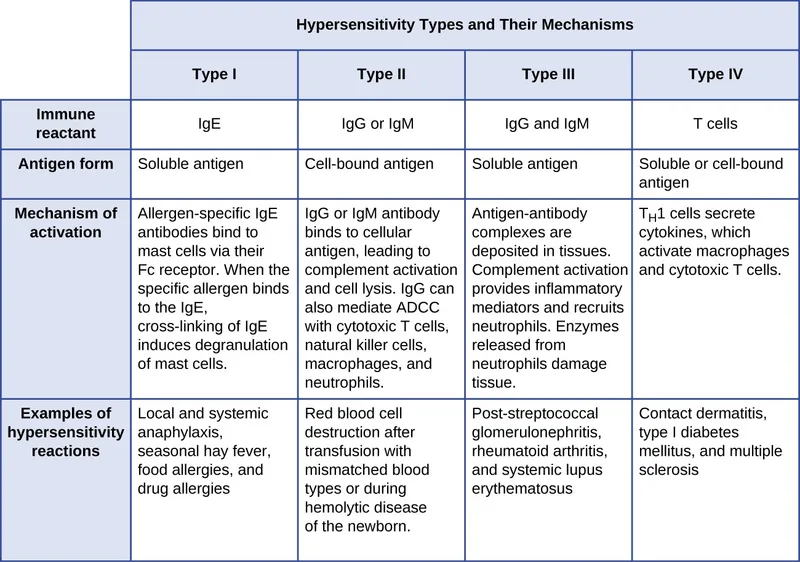
- Gell & Coombs Classification (1963): Divides reactions into four main types. 📌 ACID
Type Name (ACID) Key Mediator(s) Type I Allergic IgE, mast cells Type II Cytotoxic IgG/IgM (vs cell Ag) Type III Immune Complex IgG/IgM complexes, complement Type IV Delayed-type T-lymphocytes
⭐ Gell and Coombs classification (1963) is based on the primary mechanism of immune-mediated injury.
Type I Rxns - Allergic Alarms
📌 Mnemonic: 'First and Fast' (ACID: Allergic)
-
Mediator: IgE antibodies produced by plasma cells.
-
Key Cells: Mast cells (tissue) and basophils (circulation).
-
Key Chemical Mediators:
- Pre-formed: Histamine, proteases (e.g., tryptase).
- Newly synthesized: Leukotrienes ($LTC_4, LTD_4, LTE_4$), prostaglandins ($PGD_2$), cytokines.
-
Onset: Immediate, typically within minutes of allergen re-exposure.
-
Mechanism:
-
Clinical Examples: Anaphylaxis, Allergic Asthma, Hay fever (Allergic Rhinitis), Urticaria (hives), Atopic Eczema.

⭐ Type I hypersensitivity involves IgE antibodies coating mast cells; re-exposure to the allergen causes rapid degranulation and release of histamine and other potent mediators.
Type II Rxns - Cytotoxic Chaos
📌 Cy-2-toxic IgG/IgM antibodies target cell surface or extracellular matrix antigens, causing damage.
- Mechanisms & Examples:
- Opsonization & Phagocytosis: Cells coated with Ab/C3b are phagocytosed. E.g., Autoimmune hemolytic anemia (AIHA), Idiopathic Thrombocytopenic Purpura (ITP).
- Complement-mediated Lysis/Inflammation: Ab activates complement → MAC formation & inflammation. E.g., Goodpasture's syndrome, Rheumatic fever.
- Antibody-Dependent Cell-mediated Cytotoxicity (ADCC): NK cells bind Fc of Ab on target cell → lysis.
- Antibody-mediated Cellular Dysfunction:
- Receptor antagonism: Myasthenia Gravis (anti-AChR).
- Receptor agonism: Graves' disease (anti-TSHR).
- Blocking vital molecules: Pernicious anemia (anti-Intrinsic Factor).

⭐ Goodpasture syndrome involves antibodies against Type IV collagen (specifically the alpha-3 chain) in glomerular and alveolar basement membranes.
Type III Rxns - Immune Complex Clutter
- Mediator: Soluble Antigen-Antibody (Ag-Ab) immune complexes (ICs); primarily IgG, also IgM.
- Mechanism: "Complexes Clutter & Cause Chaos"
- ICs form in circulation (Ag excess) & deposit in tissues (e.g., vessel walls, glomeruli, joints, skin).
- Complement system activation (classical pathway: C3a, C5a anaphylatoxins) → ↑vascular permeability, neutrophil chemotaxis.
- Recruited neutrophils release lysosomal enzymes & Reactive Oxygen Species (ROS) → tissue damage (e.g., vasculitis, glomerulonephritis, arthritis).
- 📌 Mnemonic: 3 things make a complex (Antigen, Antibody, Complement).
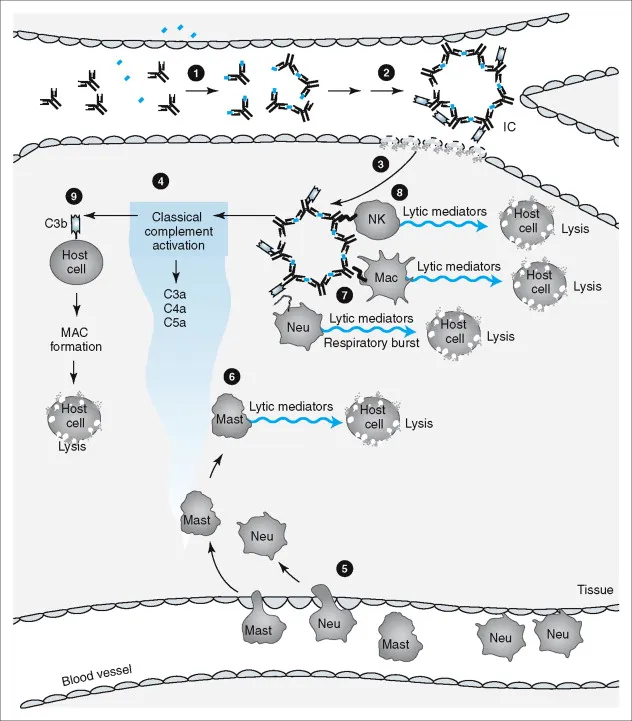
⭐ Serum sickness (systemic) and Arthus reaction (local) are classic examples of Type III hypersensitivity.
Type IV Rxns - Delayed Drama
- Mediators: T-lymphocytes (CD4+ Th1/Th17, CD8+ CTLs).
- Mechanism: Sensitized T-cells → cytokines → macrophage activation OR direct T-cell cytotoxicity.
- Onset: Delayed (24-72 hours). 📌 Mnemonic: "4 T's: T-cells, Transplant rejection, TB skin test, Touching (contact dermatitis)".
- Examples:
- CD4+ (Cytokine-mediated):
- Contact dermatitis (poison ivy).
- Tuberculin test (Mantoux): Induration ≥15mm (immunocompetent).
- Granulomas (TB, sarcoidosis).
- CD8+ (Direct cytotoxicity):
- Type 1 Diabetes.
- Multiple Sclerosis.
- Hashimoto's thyroiditis.
- Graft rejection.
- CD4+ (Cytokine-mediated):
⭐ The Mantoux test for tuberculosis is a classic example of a delayed-type hypersensitivity (DTH) reaction.
High‑Yield Points - ⚡ Biggest Takeaways
- Type I (Anaphylactic): IgE-mediated; mast cell degranulation. Examples: anaphylaxis, allergic asthma.
- Type II (Cytotoxic): Antibody (IgG/IgM)-mediated destruction of cells/tissues. Examples: Goodpasture's syndrome, AIHA.
- Type III (Immune Complex): Deposition of circulating antigen-antibody complexes. Examples: SLE, PSGN, serum sickness.
- Type IV (Delayed-Type): Cell-mediated immunity (sensitized T-lymphocytes). Examples: contact dermatitis, tuberculin PPD test.
- Arthus reaction is a localized Type III; Serum sickness is systemic Type III.
- Remember Gell and Coombs classification (Types I-IV).
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

