Adrenal Cortex: Basics - Gland Essentials
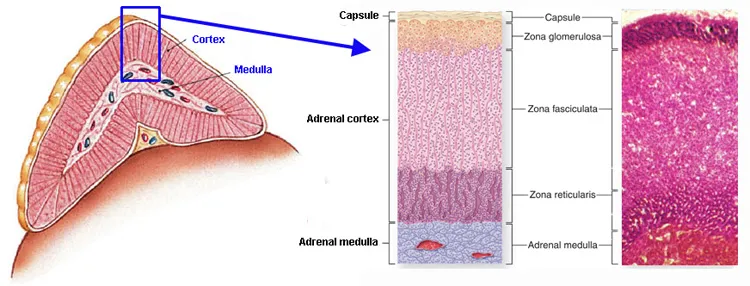
- Adrenal Cortex Layers (Outer to Inner) & Primary Products:
- Zona Glomerulosa (ZG): Mineralocorticoids (e.g., Aldosterone - salt balance).
- Zona Fasciculata (ZF): Glucocorticoids (e.g., Cortisol - sugar metabolism).
- Zona Reticularis (ZR): Androgens (e.g., DHEA - sex characteristics).
- 📌 Mnemonic (GFR → Hormones): Glomerulosa, Fasciculata, Reticularis → Salt, Sugar, Sex.
⭐ Embryological Origin: Adrenal cortex develops from mesoderm; adrenal medulla from neural crest cells.
Cushing's Syndrome - Moon Face Mayhem
⭐ Most common cause of Cushing's syndrome is exogenous glucocorticoid administration; most common endogenous cause is Cushing's disease (pituitary adenoma).
- Chronic cortisol excess. 📌 CUSHINGOID features: Central obesity, Moon facies, Buffalo hump, Purple striae, Hypertension, Hyperglycemia, Osteoporosis, Amenorrhea, Immunosuppression.
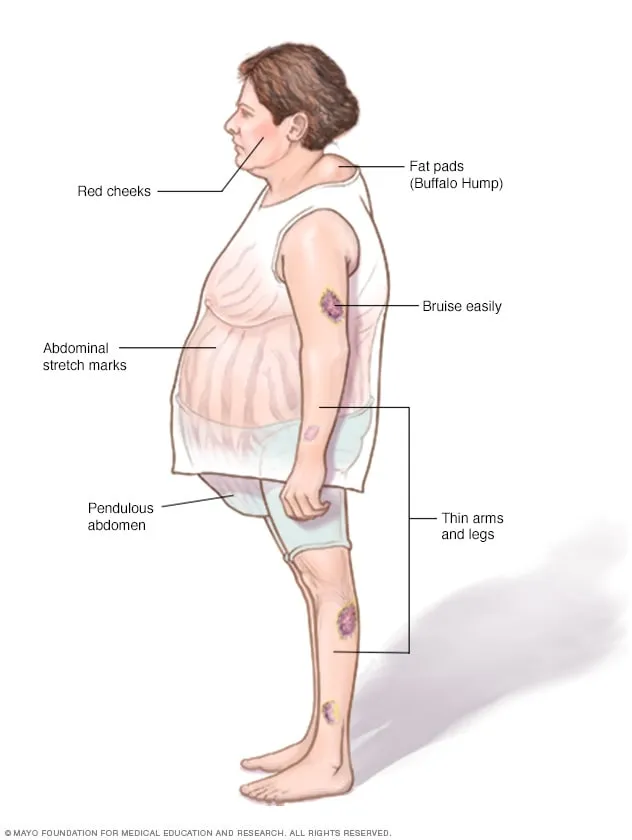
- Diagnosis:
- Screening: 24-hr Urine Free Cortisol (UFC), Late-night salivary cortisol, Low-dose Dexamethasone Suppression Test (LDDST - 1mg).
- Localization:
- Plasma ACTH: If low (e.g., <5 pg/mL) → Adrenal cause (ACTH-independent). Proceed to adrenal imaging.
- If normal/high (e.g., ≥5 pg/mL) → ACTH-dependent. Differentiate pituitary (Cushing's disease) vs. ectopic ACTH with High-dose DST (HDDST - 8mg; pituitary source typically suppresses) and/or CRH stimulation test.
Hyperaldosteronism & CAH - Salty Surges & Enzyme Snags
-
Hyperaldosteronism (Conn's Syndrome):
- Primary: ↑Aldosterone, ↓Renin.
- Causes: Adrenal adenoma (most common), bilateral adrenal hyperplasia.
- Sx: Resistant HTN, unexplained ↓K+, metabolic alkalosis. 📌 Conn's: Salty (HTN), Low K+, High Aldo.
- Dx: Aldosterone:Renin Ratio (ARR) > 20-30 (ng/dL per ng/mL/hr); confirmatory tests (e.g., saline infusion).
- Rx: Spironolactone/Eplerenone; surgery for adenoma.
-
Congenital Adrenal Hyperplasia (CAH):
- Autosomal recessive enzyme defects in cortisol synthesis → ↓Cortisol → ↑ACTH → adrenal hyperplasia & precursor shunting.
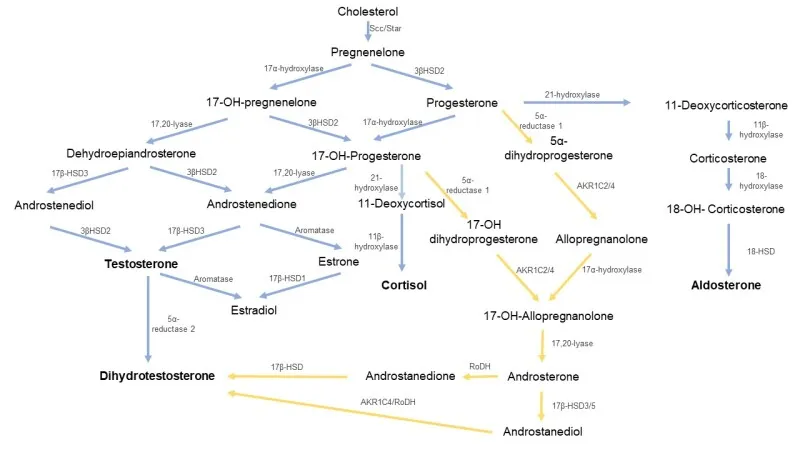
- ⭐ > 21-hydroxylase deficiency is the most common cause of Congenital Adrenal Hyperplasia.
- Key Types & Features:
Adrenal Insufficiency - Energy Crisis Central
| Feature | Primary (Addison's) | Secondary Adrenal Insufficiency |
|---|---|---|
| ACTH | ↑↑ High | ↓ Low / Normal |
| Cortisol | ↓ Low | ↓ Low |
| Aldosterone | ↓ Low | Normal |
| K+ | ↑ High (Hyperkalemia) | Normal |
| Pigmentation | ↑ Hyperpigmentation (↑MSH) | Normal |
| Causes | Autoimmune, TB, Waterhouse-Friderichsen (acute) | Pituitary/Hypothalamic failure, Chronic steroids |
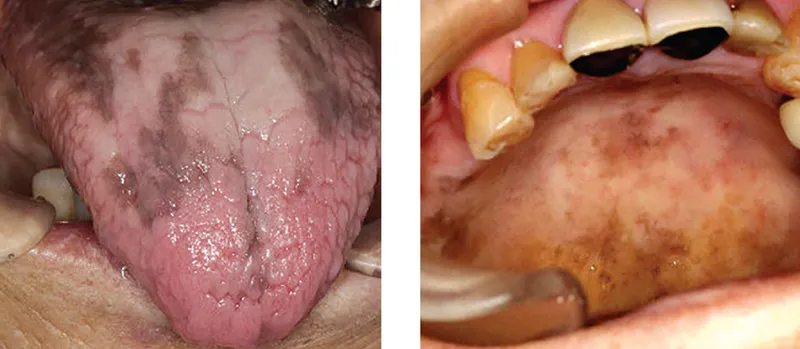
⭐ Hyperpigmentation and hyperkalemia are characteristic of primary (Addison's) but not secondary adrenal insufficiency.
- Acute Crisis: Hypotension, shock. IV hydrocortisone.
- ACTH Stim Test: Primary: Cortisol no rise > 20 µg/dL.
Adrenal Cortical Neoplasms - Cortical Growth Alarms
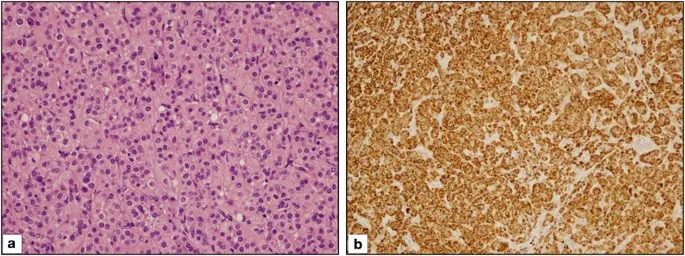
| Feature | Adrenocortical Adenoma | Adrenocortical Carcinoma |
|---|---|---|
| Size | Usually <4 cm, well-circumscribed | Often >6 cm, large, poorly-defined |
| Functionality | May be functional (Cushing's, Conn's) or non-functional | Frequently functional (virilization, Cushing's, mixed) |
| Weiss Criteria | Low score (<3), benign features | High score (≥3) indicates malignancy |
| Prognosis | Excellent | Poor, aggressive, high recurrence |
High‑Yield Points - ⚡ Biggest Takeaways
- Cushing's syndrome: Excess cortisol from pituitary adenomas (Cushing's disease), adrenal tumors, or ectopic ACTH.
- Conn's syndrome: Primary hyperaldosteronism causing hypertension, hypokalemia, low renin.
- Addison's disease: Primary adrenal insufficiency with ↓cortisol/aldosterone, ↑ACTH, hyperpigmentation, hypotension.
- Waterhouse-Friderichsen syndrome: Acute adrenal hemorrhage, classically with N. meningitidis sepsis.
- CAH: Most common is 21-hydroxylase deficiency leading to virilization, salt wasting.
- Adrenocortical carcinoma: Differentiated from adenoma by large size, necrosis, invasion.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

