Epidermis - Outer Bodyguard
- Outermost, avascular, stratified squamous epithelium; primary barrier (pathogens, UV, water).
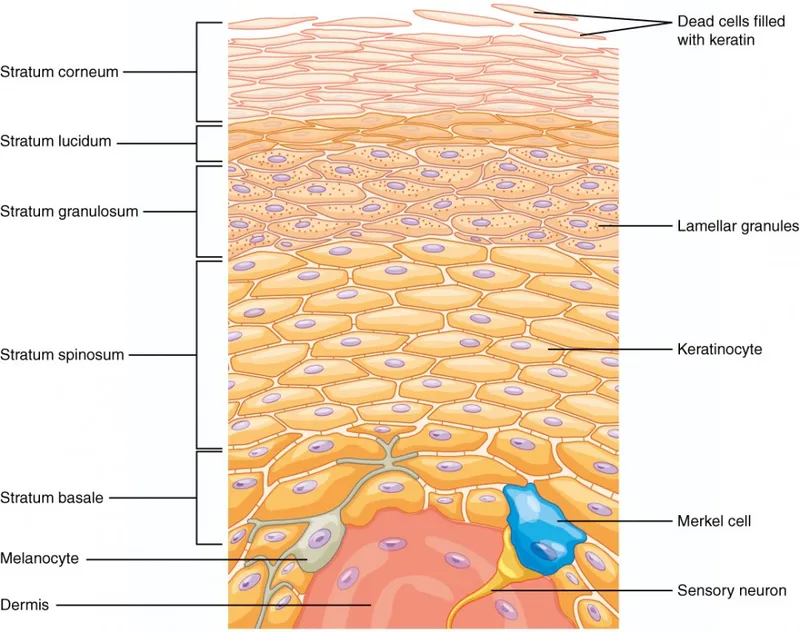
- Layers (Deep to Superficial): 📌 Mnemonic: "Britney Spears Glows Like Candy"
- S. Basale (Germinativum): Single cuboidal layer, stem cells (mitotic); melanocytes, Merkel cells.
- S. Spinosum: Polyhedral "prickle" cells (desmosomes); Langerhans cells.
- S. Granulosum: Flattened cells; keratohyalin granules; lamellar bodies (lipid barrier).
- S. Lucidum: Clear, thin; only thick skin (palms, soles); eleidin.
- S. Corneum: Anucleated corneocytes (keratin-filled); desquamation.
- Key Cells:
- Keratinocytes (~85%): Main cells; produce keratin (strength, barrier).
- Melanocytes (Neural crest): Basal; melanin (UV block); 1 per 10 basal keratinocytes.
- Langerhans Cells (Bone marrow): Spinosum; APCs (immune defense).
- Merkel Cells (Neural crest): Basal; mechanoreceptors (light touch).
- Epidermal turnover: Approx. 4 weeks (basale to corneum).
⭐ Birbeck granules (tennis-racket shaped) are characteristic of Langerhans cells.
Dermis & Dermo-Epidermal Junction - Supportive Matrix
- Dermis: Connective tissue; support, elasticity, strength.
- Papillary Dermis: Superficial. Loose CT. Type III & I collagen. Fine elastic fibers. Dermal papillae. Capillaries, Meissner's (touch).
- Reticular Dermis: Deeper. Dense irregular CT. Predominantly Type I collagen. Coarse elastic fibers. Vessels, appendages, Pacinian (pressure), Ruffini (stretch).
- Cells: Fibroblasts (synthesize matrix), mast cells, macrophages.
- Ground Substance: GAGs (e.g., hyaluronic acid), proteoglycans.
- Dermo-Epidermal Junction (DEJ): Basement Membrane Zone (BMZ).
- Layers (Epidermis to Dermis):
- Hemidesmosomes (basal cells).
- Lamina Lucida (laminin, BP antigens).
- Lamina Densa (Type IV collagen).
- Sublamina Densa (Anchoring Fibrils - Type VII collagen).
- 📌 DEJ Layers: Heavy Lions Drink Soda (Hemidesmosomes, Lucida, Densa, Sublamina densa).
- Functions: Adhesion, barrier, mechanical support.
⭐ Defects in Type VII collagen (anchoring fibrils) cause Dystrophic Epidermolysis Bullosa.
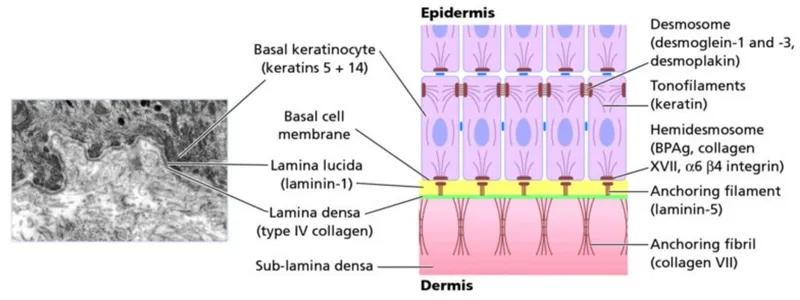
- Layers (Epidermis to Dermis):
Skin Appendages & Subcutis - Skin's Gadgets
- Eccrine Glands: Thermoregulation (sweat); entire body, esp. palms, soles, axillae; cholinergic sympathetic innervation.
- Apocrine Glands: Scent (pheromones); axillae, anogenital, areolae; adrenergic sympathetic innervation; decapitation secretion. Active from puberty.
- Sebaceous Glands: Secrete sebum (lubrication); holocrine secretion; face, scalp (most); androgen-sensitive. Part of pilosebaceous unit.
- Hair Follicles:
- Structure: Infundibulum, isthmus, inferior segment (bulb, papilla).
- Cycle: Anagen (growth, ~85-90%), Catagen (involution, ~1-2%), Telogen (rest, ~10-15%). 📌 ACT.
- Arrector pili muscle: Smooth muscle, causes piloerection ("goosebumps").
- Nails: Nail plate, bed, matrix (growth). Fingernails grow ~3 mm/month.
- Subcutis (Hypodermis): Adipose tissue lobules, connective tissue septa. Functions: Insulation, energy storage, shock absorption.

⭐ Apocrine glands utilize decapitation secretion (apical cytoplasm loss), sebaceous glands use holocrine secretion (entire cell lysis), and eccrine glands employ merocrine secretion (exocytosis).
Overall Skin Functions - Body's Versatile Shield
- Protection (Multi-layered Defense):
- Physical: Against trauma, friction (keratin).
- Chemical: Resists mild acids, alkalis.
- Microbial: Acid mantle, defensins, Langerhans cells.
- UV Radiation: Melanin absorption.
- Dehydration: Impermeable stratum corneum, lipids.
- Sensation (Sensory Input): Detects touch, pressure, pain, temperature via specialized receptors.
- Thermoregulation (Temperature Balance):
- Sweating (evaporative cooling).
- Dermal vasodilation/vasoconstriction.
- Subcutaneous fat insulation.
- Metabolic Activity:
- Vitamin D synthesis (UVB on 7-dehydrocholesterol).
- Energy storage (subcutaneous fat).
- Immune Response: Antigen presentation (Langerhans cells), cytokine production (keratinocytes).
- Excretion (Limited): Small amounts of urea, salts, water via sweat.
⭐ Langerhans cells in the epidermis are crucial antigen-presenting cells, initiating skin's immune defense.
High‑Yield Points - ⚡ Biggest Takeaways
- Epidermis: Stratum corneum (keratin barrier), spinosum (Langerhans cells, desmosomes), basale (melanocytes, stem cells).
- Dermo-Epidermal Junction: Hemidesmosomes and Type VII collagen anchor epidermis; defects cause blistering.
- Dermis: Rich in Type I collagen; supports appendages, blood vessels, and nerves.
- Skin Appendages: Eccrine (sweat/thermoregulation), apocrine (odor), sebaceous glands (sebum), hair follicles.
- Specialized Cells: Melanocytes (UV defense), Langerhans cells (immune response), Merkel cells (touch sensation).
- Core Functions: Protection (barrier), thermoregulation, Vitamin D synthesis, sensation, immune defense.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

