Eczematous Dermatoses - Itch & Scratch Saga
- General: Pruritus, erythema, vesicles (acute); scaling, lichenification (chronic).
- Histopathology:
- Acute: Spongiosis (intraepidermal edema), lymphocytic infiltrate.
- Chronic: Acanthosis, hyperkeratosis, parakeratosis.
⭐ Spongiosis is the hallmark of acute eczematous dermatitis.
- Atopic Dermatitis (AD):
- Patho: Th2 immune response, filaggrin (FLG) gene mutations.
- Distribution: Infants (face, extensors); Children/Adults (flexures).
- Allergic Contact Dermatitis (ACD):
- Patho: Type IV (delayed) hypersensitivity. Haptens (e.g., nickel, poison ivy).
- Morph: Well-demarcated lesions at contact site.
- Irritant Contact Dermatitis (ICD):
- Patho: Non-immunologic, direct chemical injury to keratinocytes.
- Morph: Burning, stinging > itch. Often hands.
- Seborrheic Dermatitis (SD):
- Patho: Malassezia spp. role, inflammation.
- Distribution: Scalp (dandruff), face (nasolabial folds, eyebrows), chest. Greasy yellow scales.

Papulosquamous Disorders - Scaly Skin Stories
Psoriasis vs. Lichen Planus
| Feature | Psoriasis | Lichen Planus |
|---|---|---|
| Clinical | Well-demarcated erythematous plaques, silvery scales. Auspitz sign, Koebner phenomenon. Guttate: drop-like, post-strep. | 📌 5 P's: Purple, Pruritic, Polygonal, Papules, Plaques. Wickham's striae (lacy white lines). Flexor surfaces, oral/mucosal. |
| Histology | Parakeratosis, Munro's microabscesses (neutrophils in S. corneum), acanthosis with clubbed rete ridges, suprapapillary thinning. | Hyperkeratosis, sawtooth rete ridges, band-like lymphocytic infiltrate at DEJ, Civatte bodies (apoptotic keratinocytes). |

Vesiculobullous Diseases - Bubble Trouble Tales
- Autoimmune blistering disorders. Key distinction: level of epidermal split.
| Feature | Pemphigus Vulgaris (PV) | Bullous Pemphigoid (BP) |
|---|---|---|
| Pathogenesis | AutoAbs vs. Desmoglein 1 & 3 (intercellular) | AutoAbs vs. BPAG1 (BP230) & BPAG2 (BP180) (hemidesmosomes) |
| Level of Split | Intraepidermal (suprabasal acantholysis) | Subepidermal (dermo-epidermal junction) |
| Clinical: Bullae | Flaccid, easily ruptured, painful erosions | Tense, intact, often pruritic |
| Nikolsky Sign | Positive (+) (pressure extends blister) | Negative (-) |
| Mucosal Involvement | Common, severe (oral >50%) | Less common (~10-30%), milder |
| Age (Typical) | 40-60 years | >60 years (elderly) |
| Direct IF (DIF) | Intercellular IgG/C3 ("Fishnet" pattern) | Linear IgG/C3 at Basement Membrane Zone (BMZ) |
⭐ Pemphigus vulgaris shows intraepidermal acantholysis and a 'row of tombstones' (basal cells attached to dermis) appearance on histology.
Hypersensitivity Reactions - Rash Decisions Drama
- Spectrum of severe mucocutaneous reactions: EM Minor → EM Major → SJS → SJS/TEN Overlap → TEN.
- Triggers:
- EM: Infections (📌 HSV most common), Mycoplasma.
- SJS/TEN: Drugs (e.g., sulfonamides, allopurinol, anticonvulsants, NSAIDs), Mycoplasma, vaccines.
- Key Features:
- EM: Target/iris lesions (often acral). EM Minor: minimal/no mucosal. EM Major: mucosal involvement (≥1 site), <10% BSA.
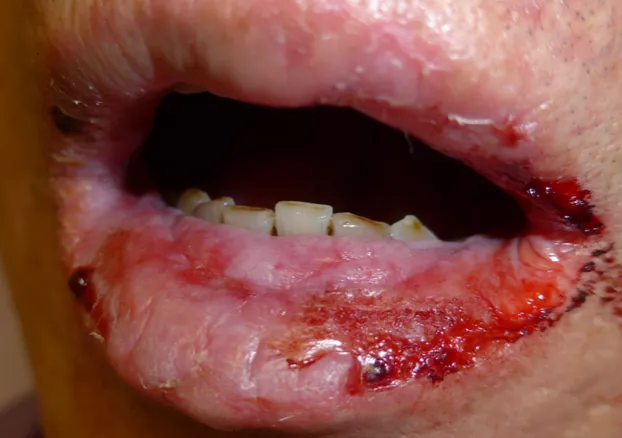
- SJS/TEN: Prodrome (fever, malaise), painful atypical targets/macules → widespread blistering, Nikolsky sign (+), severe mucosal erosions (≥2 sites).
- Histology:
- EM: Keratinocyte apoptosis, vacuolar interface change, lymphocytic infiltrate.
- SJS/TEN: Full-thickness epidermal necrosis, subepidermal split/blisters.
- BSA Detachment for SJS/TEN Classification:
- SJS: <10%
- SJS/TEN Overlap: 10-30%
- TEN: >30% (SCORTEN score for prognosis)
⭐ Herpes simplex virus is the most common trigger for Erythema Multiforme.
High‑Yield Points - ⚡ Biggest Takeaways
- Psoriasis: Characterized by acanthosis, parakeratosis, Munro's microabscesses, and elongated rete ridges.
- Lichen Planus: Features sawtooth rete ridges, Civatte bodies, and a dense band-like lymphocytic infiltrate at the dermo-epidermal junction.
- Eczema (Dermatitis): Acute shows spongiosis; chronic presents with acanthosis and hyperkeratosis.
- Pemphigus Vulgaris: Intraepidermal bullae due to acantholysis (Nikolsky sign positive); antibodies target desmogleins.
- Bullous Pemphigoid: Subepidermal bullae with numerous eosinophils (Nikolsky sign negative); targets hemidesmosomal proteins.
- Dermatitis Herpetiformis: Subepidermal bullae with neutrophilic microabscesses at dermal papillae tips; strong celiac disease association with IgA deposits.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

