Autoimmune Manifestations - Immune System Alerts
- Systemic Lupus Erythematosus (SLE)
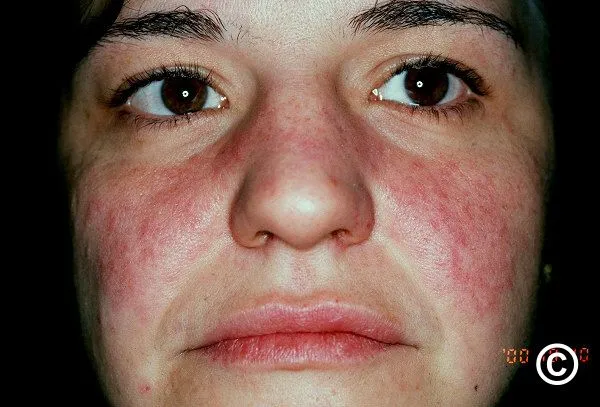
- Malar (butterfly) rash, discoid lesions, photosensitivity.
- Oral ulcers, non-scarring alopecia, Raynaud's. ANA often positive.
- Dermatomyositis
- Heliotrope rash (eyelids), Gottron's papules (knuckles).
- Shawl sign, V-sign, mechanic's hands. Periungual telangiectasias.
- Associated with internal malignancy (adults > 40 yrs). Anti-Jo-1, Anti-Mi-2.
- Scleroderma (Systemic Sclerosis)
- Skin thickening/fibrosis (sclerodactyly), Raynaud's (often first).
- Telangiectasias, calcinosis cutis, "salt-and-pepper" dyspigmentation.
- 📌 CREST: Calcinosis, Raynaud's, Esophageal dysmotility, Sclerodactyly, Telangiectasia. Anti-centromere Ab.
- Pemphigus Vulgaris
- Flaccid bullae, erosions (oral mucosa often first).
- Nikolsky sign positive. Intraepidermal acantholysis.
⭐ Antibodies against desmoglein 1 & 3 (anti-Dsg1, anti-Dsg3).
- Bullous Pemphigoid
- Tense bullae on erythematous/urticarial base (elderly).
- Nikolsky sign negative. Subepidermal split with eosinophils. Anti-BPAG1/2.
Metabolic & Endocrine - Inside‑Out Clues
- Diabetes Mellitus:
- Necrobiosis lipoidica (atrophic plaques, shins)
- Diabetic dermopathy (shin spots)
- Acanthosis nigricans (velvety, flexures)

- Eruptive xanthomas (↑ triglycerides)
- Bullosis diabeticorum
- Thyroid Disorders:
- Hypo: Myxedema, dry skin, madarosis (outer eyebrow loss)
- Hyper (Graves'): Pretibial myxedema, acropachy, Plummer's nails
- Adrenal Disorders:
- Cushing's: Violaceous striae (>1 cm), moon facies, buffalo hump, atrophy
- Addison's: Hyperpigmentation (oral, palmar, scars)
- Xanthomas:
- Xanthelasma palpebrarum (eyelids; normolipidemic common)
- Tuberous, tendinous, eruptive (hyperlipidemia)
- Porphyria Cutanea Tarda (PCT): Photosensitivity, bullae (sun-exposed), fragile skin, hypertrichosis, port-wine urine.
⭐ Acanthosis nigricans can be a sign of insulin resistance (e.g., diabetes) or internal malignancy (especially gastric adenocarcinoma).
GI & Nutritional - Gut‑Skin Signals
- IBD (Crohn's/UC):
- Erythema nodosum (EN), Pyoderma gangrenosum (PG).
- Oral aphthae, cutaneous Crohn's.
- Celiac Disease:
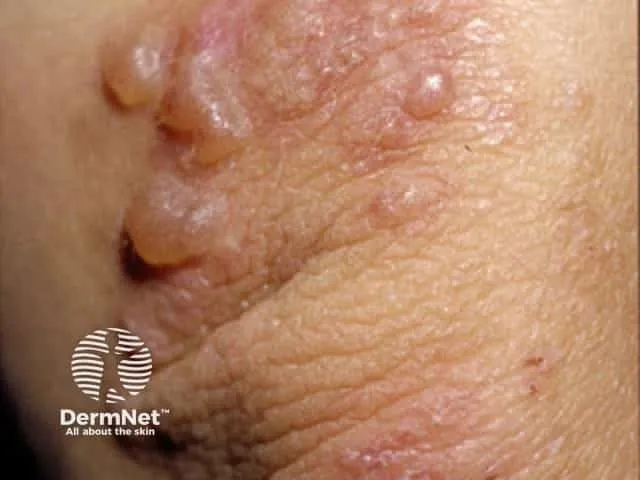
- Dermatitis herpetiformis (DH): intensely pruritic vesicles (extensors); IgA at DEJ.
- Angular cheilitis, glossitis.
- Dermatitis herpetiformis (DH): intensely pruritic vesicles (extensors); IgA at DEJ.
⭐ Dermatitis herpetiformis is a highly specific cutaneous marker for Celiac Disease, responding to a gluten-free diet.
- Nutritional Deficiencies:
- Zinc (Acrodermatitis Enteropathica): Periorificial/acral dermatitis, alopecia, diarrhea.
- Niacin/B3 (Pellagra): 📌 3 D's: Dermatitis (photosensitive, Casal's necklace), Diarrhea, Dementia.
- Vit C (Scurvy): Perifollicular hemorrhage, corkscrew hairs, gingivitis.
- Liver Disease: Pruritus, jaundice, spider nevi, palmar erythema.
- Pancreatic Disease: Enzymatic panniculitis (painful nodules), Trousseau's sign (migratory thrombophlebitis with malignancy).
Paraneoplastic & Vascular - Cancer & Vessel Alarms
- Paraneoplastic Syndromes (Skin signals of internal cancer):
- Acanthosis Nigricans: GI (stomach), lung. Velvety skin (axilla, neck).
- Leser-Trélat sign: Sudden ↑ seborrheic keratoses. GI (stomach, colon).
- Tripe Palms: Gastric/Lung cancer. Rugose palms.
- Dermatomyositis: Gottron's papules, heliotrope rash. Ovarian, lung. 📌 "Got Heli?"
- Necrolytic Migratory Erythema: Glucagonoma. Annular crusted plaques.
- Sweet's Syndrome: AML. Tender red plaques.
- Cutaneous Vasculitis (Vessel inflammation):
- Palpable purpura: Hallmark. Non-blanching. Lower limbs.
- Leukocytoclastic Vasculitis (LCV): Small vessels. Drugs, infections, malignancy.
- IgA Vasculitis (HSP): Purpura, arthritis, abdominal pain, renal.
- Polyarteritis Nodosa (PAN): Medium vessels. Livedo reticularis, nodules, ulcers. HBV.

⭐ Leser-Trélat sign: abrupt onset of multiple seborrheic keratoses, strongly linked to internal malignancy, especially GI adenocarcinoma.
High‑Yield Points - ⚡ Biggest Takeaways
- Acanthosis nigricans: Velvety plaques; linked to insulin resistance and gastric cancer.
- Dermatomyositis: Gottron's papules, heliotrope rash; signals underlying malignancy.
- Erythema nodosum: Tender shin nodules; associated with sarcoidosis, infections, IBD.
- Pyoderma gangrenosum: Painful ulcers with violaceous borders; linked to IBD.
- Porphyria cutanea tarda: Sun-exposed blisters; associated with liver disease, HCV.
- Necrobiosis lipoidica: Atrophic shin plaques; strongly indicates diabetes mellitus.
- Sweet's syndrome: Tender plaques, fever; consider Acute Myeloid Leukemia (AML).
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

