Fracture Principles - Bone Break Basics
- Definition: Break in cortical continuity of bone.
- Description:
- Skin: Open (communicates with exterior) vs. Closed.
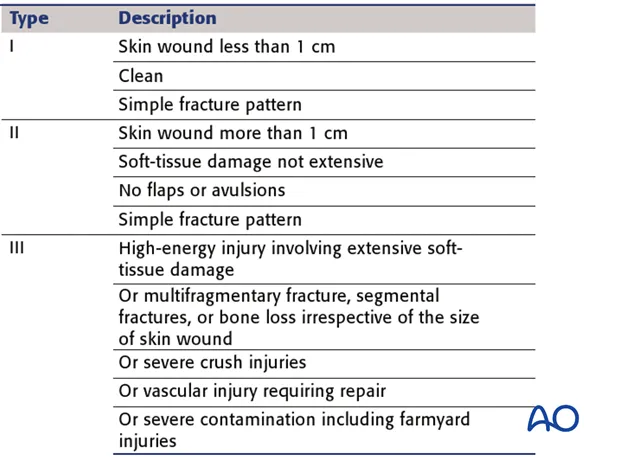
- Open #: Gustilo-Anderson classification (I, II, IIIA/B/C). Requires antibiotics, debridement.
- Displacement: Angulation, Rotation, Translation, Shortening.
- Pattern: Transverse, Oblique, Spiral, Comminuted (>2 fragments), Segmental, Greenstick (pediatric), Avulsion.
- Skin: Open (communicates with exterior) vs. Closed.
- Healing (Secondary - most common):
- Inflammation (Haematoma)
- Soft Callus (Fibrocartilaginous)
- Hard Callus (Woven Bone)
- Remodelling (Lamellar Bone) 📌 Wolff's Law: Bone remodels in response to mechanical stress.
- Initial Care: ATLS survey. RICE (Rest, Ice, Compression, Elevation). Splinting. Analgesia. Neurovascular assessment.
⭐ Compartment Syndrome: Intracompartmental pressure > 30 mmHg (or diastolic minus compartment pressure < 30 mmHg). Leads to ischemia. 6 Ps: Pain (key!), Paresthesia, Pallor, Pulselessness, Paralysis, Poikilothermia.
Hip & Femur Fractures - Thighbone Traumas
- Neck of Femur (NOF): Intracapsular. Main blood supply: Medial Circumflex Femoral Artery (MCFA). 📌 MCFA: Main Circulation For Adult NOF.
- Classifications:
- Garden: I (incomplete/impacted), II (complete, undisplaced), III (complete, partial displacement), IV (complete, full displacement).
- Pauwels Angle: I (<30° stable), II (30-50° shear), III (>50° high shear).
- Mgmt: Young (<65 yrs) or Garden I/II: Internal Fixation. Elderly (>65 yrs) & Garden III/IV: Arthroplasty (Hemi/Total).
- Complications: Avascular Necrosis (AVN), non-union.
⭐ Garden stages III & IV and Pauwels III have the highest risk of AVN.
- Classifications:
- Intertrochanteric: Extracapsular, good blood supply. Mgmt: Dynamic Hip Screw (DHS) or Proximal Femoral Nail (PFN).
- Subtrochanteric: Below lesser trochanter. Mgmt: Cephalomedullary IM Nail.
- Femoral Shaft: High-energy. Mgmt: IM Nailing. Complications: Fat embolism, ARDS.
Knee & Tibial Fractures - Shinbone Shockers

-
Tibial Plateau Fractures (Intra-articular)
- Schatzker Classification (Types I-VI):
- I: Pure cleavage, lateral.
- II: Cleavage + depression, lateral.
- III: Pure depression, lateral.
- IV: Medial plateau; worst prognosis due to varus collapse.
- V: Bicondylar.
- VI: Metaphyseal-diaphyseal dissociation.
- Management: ORIF for articular depression >2-3 mm or condylar widening >5 mm.
- Complications: Peroneal nerve injury (anterolateral approach), popliteal artery injury (posterior fractures), post-traumatic OA.
- Schatzker Classification (Types I-VI):
-
Tibial Shaft Fractures
- Most common long bone fracture.
- Management:
- Closed, stable: Cast/functional brace.
- Unstable/displaced/open: Intramedullary (IM) nailing.
- ⚠️ Complications:
- Compartment syndrome (📌 6 P's: Pain out of proportion, Paresthesia, Pallor, Paralysis, Pulselessness, Poikilothermia). Fasciotomy if intracompartmental pressure >30 mmHg or ΔP <30 mmHg (Diastolic BP - Compartment Pressure).
- Non-union, malunion, infection (especially open fractures - Gustilo-Anderson classification).
⭐ Schatzker Type II (lateral split with depression) is the most common type of tibial plateau fracture.
Ankle & Foot Fractures - Distal Damage Details
- Ankle Fractures:
- Lauge-Hansen: Foot position & force (SER commonest).
- Weber (Fibular #):
- A: Below syndesmosis (intact).
- B: At syndesmosis (variable injury).
- C: Above syndesmosis (injured).
- Pilon: Distal tibia comminuted intra-articular #; axial load.
- Foot Fractures:
- Talus: Neck # (Hawkins class.); ↑AVN risk. 📌 Hawkins sign (subchondral lucency) = viable.
- Calcaneus: ↓Böhler's angle (normal 25-40°). Assoc. lumbar spine #.
- Navicular: Often stress #; AVN risk.
- Lisfranc Injury: Tarsometatarsal disruption. Fleck sign pathognomonic.
- Jones #: 5th MT base (meta-diaphyseal); high non-union.
- March #: Metatarsal stress # (2nd/3rd).
⭐ Weber Type C fractures, being above the syndesmosis, always involve syndesmotic injury and typically require surgical fixation with syndesmotic screws for ankle stability.
High‑Yield Points - ⚡ Biggest Takeaways
- Femoral Neck Fx: Garden's classification; high AVN risk with displacement.
- Intertrochanteric Fx: Extracapsular; better prognosis than femoral neck.
- Femoral Shaft Fx: High-energy; risk of fat embolism, compartment syndrome. IM nailing standard.
- Tibial Plateau Fx: Schatzker types; associated meniscal/ligamentous injuries (ACL, MCL).
- Tibial Shaft Fx: Most common long bone fracture; risk of non-union, compartment syndrome.
- Ankle Fx: Danis-Weber (fibula & syndesmosis); Lauge-Hansen (mechanism).
- Calcaneal Fx: Fall from height; associated lumbar spine fractures; check Bohler's angle.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

