PJI Basics - Setting the Stage
- Prosthetic Joint Infection (PJI): A severe complication involving the artificial joint and adjacent tissues, often leading to implant failure.
- Significance: Major cause of morbidity, multiple surgeries, prolonged antibiotics, and ↑ healthcare costs.
- Temporal Classification (from index surgery):
- Early Onset: <3 months. Often acquired intraoperatively.
- Delayed Onset: 3-12 months (some use 3-24 months). Typically low-virulence organisms.
- Late Onset: >12 months (some use >24 months). Usually due to hematogenous seeding.
⭐ PJI is a leading reason for revision arthroplasty, especially in knee replacements (TKA).
Bugs & Biofilms - The Culprit Crew
- Key Pathogens by Onset:
- Early (<3 months): Staphylococcus aureus (most common overall, MSSA/MRSA), Gram-negative bacilli (e.g., Pseudomonas, Enterobacteriaceae).
- Delayed (3-12 months): Coagulase-negative Staphylococci (CoNS) like S. epidermidis; Cutibacterium acnes (especially shoulder implants).
- Late (>12 months): Hematogenous spread; S. aureus, Streptococci, Gram-negative bacilli.
- Biofilm - The Microbial Fortress:
- Definition: Structured community of bacteria encased in a self-produced Extracellular Polymeric Substance (EPS), adherent to the prosthesis.
- Pathogenesis: Attachment → Microcolony formation & EPS production → Maturation (3D structure) → Dispersion.
- Significance: ↑ Antibiotic resistance (often 100-1000x), shields from host immunity, necessitates implant removal for cure.
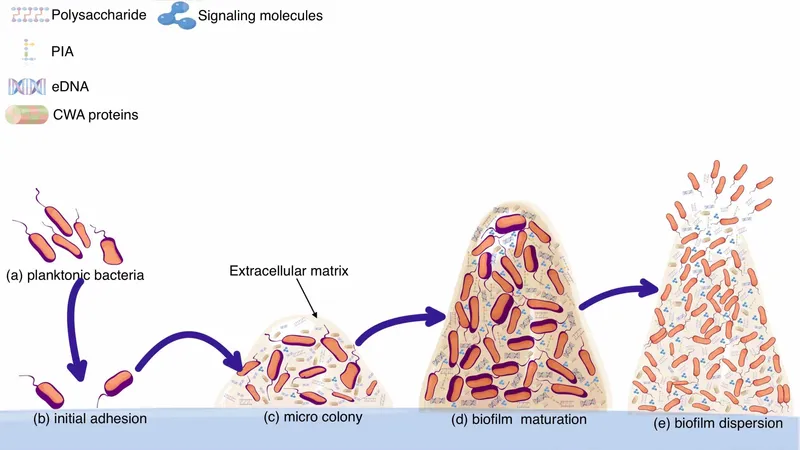
⭐ Staphylococcus epidermidis, a CoNS, is notorious for its robust biofilm formation, leading to chronic, low-grade, delayed-onset PJIs that are difficult to treat without implant removal.
Diagnosis Dilemma - Cracking the Case
- Clinical Clues:
- Persistent joint pain (new/worsening).
- Local: Swelling, erythema, warmth.
- Sinus tract (strong PJI indicator).
- Fever (acute PJI).
- Lab Markers:
- Serum: ↑ ESR (>30 mm/hr), ↑ CRP (>10 mg/L).
- Synovial Fluid:
- WBC >3000/µL, PMN% >80% (hip/knee).
- Culture (aerobic/anaerobic): Min. 2 samples.
- Leukocyte Esterase (++), Alpha-defensin.
- Diagnostic Standards:
- MSIS or ICM 2018 criteria are key.
⭐ A sinus tract communicating with the prosthesis is a major criterion for PJI diagnosis.
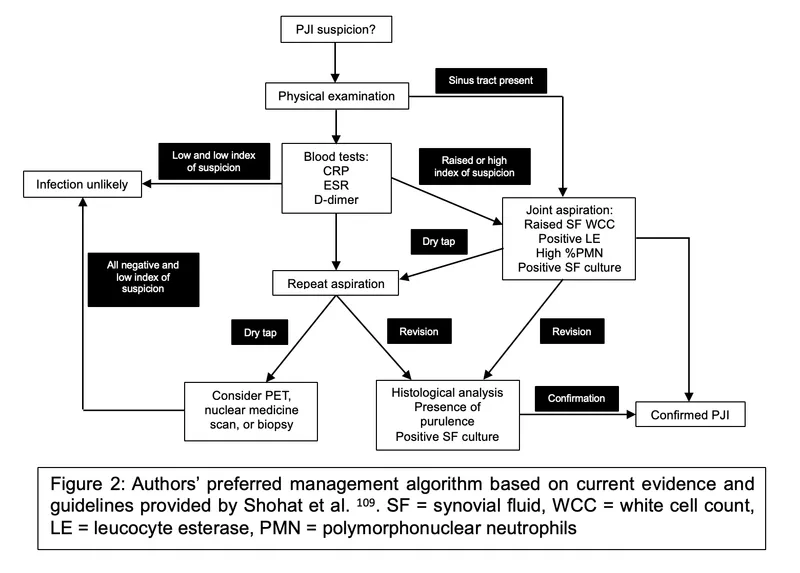
Treatment Tactics - Battling the Bugs
-
Core Goals: Eradicate infection, pain relief, restore function, prevent recurrence.
-
Multidisciplinary Team: Ortho, ID, Microbiology.
-
Surgical Strategies:
- DAIR (Debridement, Antibiotics, and Implant Retention):
- Early PJI (<4 wks post-op OR acute hematogenous <3 wks symptoms).
- Stable implant, susceptible organism, good soft tissue.
- One-Stage Exchange:
- Select cases: known susceptible organism, good host & tissues.
- Implant removal, debridement, immediate reimplantation.
- Two-Stage Exchange (Gold Standard for Chronic PJI):
- Stage 1: Implant removal, debridement, antibiotic spacer + IV Abx (4-6 wks).
- Stage 2: Reimplantation after infection clearance (typically 2-8 wks post-Abx).
- Resection Arthroplasty / Amputation: Salvage for severe/failed cases.
- DAIR (Debridement, Antibiotics, and Implant Retention):
-
Antibiotic Therapy:
- Prolonged: IV then oral (weeks to months).
- Biofilm-active agents (e.g., Rifampicin for Staph).
- Guided by culture & sensitivity.

⭐ Rifampicin is crucial for treating Staphylococcal PJI due to its excellent biofilm penetration, but it should never be used as monotherapy to prevent resistance.
High‑Yield Points - ⚡ Biggest Takeaways
- Key organisms: Staphylococcus aureus and Coagulase-Negative Staphylococci (CoNS) are most common.
- Diagnosis: Synovial fluid culture is gold standard; ↑ ESR/CRP are sensitive inflammatory markers.
- Biofilm formation on implants makes eradication challenging, often requiring implant removal.
- Treatment for acute early PJI: DAIR (Debridement, Antibiotics, Implant Retention).
- Gold standard for chronic PJI: Two-stage revision arthroplasty.
- Antibiotic-loaded cement spacers are integral to two-stage revision success.
- Prolonged antibiotics (IV then oral) are essential post-operatively for 4-6 weeks or longer based on sensitivity and clinical response.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

