Pediatric Ophthalmology and Strabismus

On this page
👁️ Pediatric Ophthalmology and Strabismus
Children's visual systems are architectural marvels under construction, where misalignment during critical developmental windows can permanently reshape how the brain processes sight. You'll master the mechanics of binocular alignment, learn to distinguish pseudostrabismus from true deviation, and build systematic frameworks for recognizing patterns that guide surgical versus non-surgical intervention. By integrating developmental milestones with examination techniques and treatment algorithms, you'll gain the diagnostic precision needed to preserve stereopsis and prevent amblyopia in your youngest patients.
🎯 The Pediatric Eye Command Center: Developmental Vision Architecture
📌 Remember: CHILD - Critical periods, High plasticity, Immature structures, Limited cooperation, Developmental milestones
The pediatric eye differs fundamentally from adult eyes in structural immaturity, ongoing development, and neural plasticity. Key developmental parameters include:
- Axial length: Grows from 16-17mm at birth to 23-24mm by age 3 years
- Corneal diameter: Increases from 9.5mm to 12mm during first year
- Visual acuity: Develops from 20/400 at birth to 20/20 by age 3-5 years
- Binocular vision: Establishes between 6 weeks to 4 months
- Stereopsis: Matures by 6 months with fine stereoacuity by 2 years
| Parameter | Birth | 6 Months | 2 Years | 5 Years | Adult |
|---|---|---|---|---|---|
| Axial Length (mm) | 16-17 | 20-21 | 22-23 | 23-24 | 23-24 |
| Visual Acuity | 20/400 | 20/200 | 20/60 | 20/20 | 20/20 |
| Corneal Power (D) | 48-50 | 45-46 | 43-44 | 43 | 43 |
| Lens Power (D) | 35 | 25 | 20 | 19 | 19 |
| Stereoacuity (arcsec) | None | 3000 | 60 | 40 | 40 |
The critical period concept governs all pediatric ophthalmology interventions. During these windows, the visual cortex remains maximally plastic, allowing for:
- Amblyopia reversal: Most effective before age 7 years
- Strabismus correction: Optimal binocular outcomes when treated before age 2 years
- Cataract surgery: Must occur within 6 weeks for dense congenital cataracts
- Ptosis repair: Required before age 5 years if vision-threatening
💡 Master This: Every pediatric eye condition must be evaluated against developmental timelines - the same condition requiring urgent intervention in a 2-year-old might be observational in a 10-year-old
Understanding pediatric ophthalmology transforms routine eye examinations into developmental assessments where timing determines visual destiny.
🎯 The Pediatric Eye Command Center: Developmental Vision Architecture
🔍 Strabismus Mechanics: The Binocular Alignment Engine
📌 Remember: MOTOR - Misalignment causes, Ocular deviation, Torsion components, Orbital restrictions, Refractive influences
Motor Components of Strabismus:
- Primary deviation: Misalignment when normal eye fixates
- Secondary deviation: Misalignment when strabismic eye fixates
- Comitance: Equal deviation in all gaze directions (comitant)
- Incomitance: Variable deviation with gaze direction (incomitant)
- Torsional component: Cyclodeviations around visual axis
Sensory Adaptations to Strabismus:
- Suppression: Active cortical inhibition of deviated eye image
- Amblyopia: Reduced visual acuity from disuse or active suppression
- Anomalous retinal correspondence: Abnormal binocular mapping
- Loss of stereopsis: Absent or reduced depth perception
| Strabismus Type | Prevalence | Age of Onset | Amblyopia Risk | Surgical Success |
|---|---|---|---|---|
| Infantile Esotropia | 0.5% | 0-6 months | 40-50% | 80-90% |
| Accommodative Esotropia | 1-2% | 2-3 years | 25-35% | 90-95% |
| Intermittent Exotropia | 1% | 2-4 years | 10-20% | 70-80% |
| Constant Exotropia | 0.5% | Variable | 60-70% | 60-75% |
| Vertical Deviations | 0.1% | Variable | 30-40% | 70-85% |
Measurement Techniques:
- Hirschberg test: 1mm corneal light reflex displacement = 15 prism diopters
- Krimsky test: Prism neutralization of corneal reflexes
- Cover-uncover test: Detects manifest deviation (tropia)
- Alternate cover test: Measures total deviation (tropia + phoria)
- Prism and cover test: Quantifies deviation magnitude
💡 Master This: Comitant strabismus suggests supranuclear or muscle problems, while incomitant strabismus indicates nerve palsy or mechanical restriction - this distinction guides diagnostic workup
The sensory-motor relationship in strabismus creates a feedback loop where motor misalignment produces sensory adaptations that can reinforce the motor deviation, making early intervention crucial for breaking this cycle.
🔍 Strabismus Mechanics: The Binocular Alignment Engine
🎪 Pattern Recognition Mastery: The Strabismus Detective Framework
📌 Remember: DETECT - Direction of deviation, Eye preference, Timing of onset, Eye movements, Comitance, Torsion
Age-Based Pattern Recognition:
Birth to 6 Months:
- Intermittent deviations: Normal up to 3-4 months
- Constant large esotropia: Suggests infantile esotropia
- Any exotropia: Always abnormal, requires evaluation
- Vertical deviations: Always pathological
6 Months to 2 Years:
- New onset esotropia: Red flag - rule out accommodative or pathological causes
- Intermittent exotropia: Common, monitor for progression
- Sudden onset: Consider neurological causes
- Unilateral preference: High amblyopia risk
2-5 Years:
- Accommodative esotropia: Peak age, often hyperopia-related
- Intermittent exotropia: May progress to constant
- Vertical deviations: Often superior oblique palsy
- Variable deviations: Consider refractive causes
| Clinical Pattern | Key Features | Urgent Action | Success Rate |
|---|---|---|---|
| Infantile Esotropia | Large angle, alternating, <6 months | Surgery <24 months | 80-90% |
| Accommodative ET | +2.00D hyperopia, age 2-3 years | Glasses trial | 90-95% |
| Acute Esotropia | Sudden onset, diplopia, any age | Neuroimaging | Variable |
| Intermittent XT | Distance > near, fatigue | Monitor progression | 70-80% |
| Paralytic Squint | Incomitant, head turn | Identify cause | 60-85% |
"Red Flag" Patterns Requiring Urgent Evaluation:
- Sudden onset strabismus after 6 months of age
- Incomitant deviations with restricted eye movements
- Vertical deviations with head tilt or torticollis
- Nystagmus associated with strabismus
- Ptosis with strabismus (suggests cranial nerve palsy)
- Proptosis or orbital asymmetry
Systematic Examination Sequence:
- Visual acuity: Age-appropriate methods (preferential looking, HOTV, Snellen)
- Fixation pattern: Central, steady, maintained in each eye
- Ocular motility: Ductions (monocular) and versions (binocular)
- Alignment testing: Cover tests in primary and secondary gazes
- Sensory testing: Stereopsis, suppression, retinal correspondence
💡 Master This: The 4-step approach - History (onset, family history), Vision (acuity, fixation), Motility (ductions, versions), Alignment (cover tests, measurements) - systematically identifies 95% of strabismus patterns
Treatment Decision Framework:
Pattern recognition in pediatric strabismus transforms complex presentations into systematic diagnostic pathways, ensuring optimal timing and appropriate interventions for each unique case.
🎪 Pattern Recognition Mastery: The Strabismus Detective Framework
⚖️ Differential Mastery: The Strabismus Discrimination Matrix
📌 Remember: DIFFER - Direction consistency, Incomitance degree, Fixation preference, Family history, Eye movement restriction, Refractive error magnitude
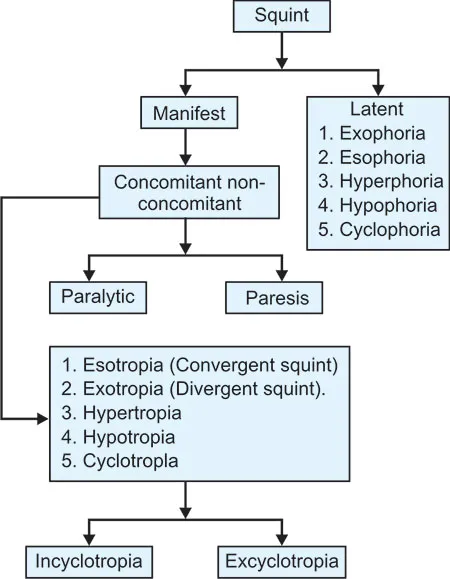
Esotropia Differential Matrix:
| Type | Age Onset | Deviation Size | Refractive Error | AC/A Ratio | Amblyopia Risk |
|---|---|---|---|---|---|
| Infantile | 0-6 months | 40-60 PD | Variable | Normal (3-5:1) | 40-50% |
| Accommodative | 2-3 years | 20-40 PD | +2.00 to +6.00D | High (>6:1) | 25-35% |
| Partially Accommodative | 2-4 years | Variable | +1.00 to +4.00D | Variable | 30-40% |
| Acute Acquired | Any age | Variable | Variable | Variable | 20-30% |
| Sensory | Variable | Large (>40 PD) | Variable | Variable | 90-100% |
| Restrictive | Variable | Incomitant | Variable | Variable | Variable |
- Intermittent Exotropia: Distance > near deviation, good fusional control
- Constant Exotropia: Equal distance/near, poor fusional control
- Sensory Exotropia: Dense amblyopia or structural abnormality
- Consecutive Exotropia: Post-surgical overcorrection
- Restrictive Exotropia: Mechanical limitation, incomitant
Critical Quantitative Discriminators:
AC/A Ratio (Accommodative Convergence/Accommodation):
- Normal: 3-5:1 (3-5 PD convergence per 1 diopter accommodation)
- High AC/A: >6:1 (suggests accommodative esotropia)
- Low AC/A: <3:1 (may indicate divergence excess)
Deviation Measurements:
- Small angle: <15 PD (often microtropia or phoria)
- Moderate angle: 15-40 PD (typical accommodative or intermittent)
- Large angle: >40 PD (suggests infantile, sensory, or paralytic)
⭐ Clinical Pearl: Accommodative esotropia shows >10 PD reduction with +3.00D lenses, while non-accommodative shows <5 PD change - this lens test differentiates management approaches
Incomitance Assessment:
| Condition | Primary Gaze | Secondary Gaze | Restriction Pattern | Head Position |
|---|---|---|---|---|
| VI Nerve Palsy | Variable ET | Increased ET in abduction | Lateral rectus weakness | Face turn away |
| III Nerve Palsy | Large XT | Variable | Multiple muscles | Variable |
| IV Nerve Palsy | Minimal | Hypertropia in adduction | Superior oblique weakness | Head tilt |
| Brown Syndrome | Minimal | Hypotropia in adduction | Mechanical restriction | Chin up |
| Duane Syndrome | Variable | Retraction on adduction | Lateral rectus fibrosis | Face turn |
- Worth 4-Dot Test: Assesses suppression and diplopia
- Stereoacuity Testing: Titmus (40-3000 arcsec), Randot (20-800 arcsec)
- Bagolini Striated Glasses: Evaluates retinal correspondence
- 4-Prism Diopter Test: Detects microtropia (<5 PD deviations)
💡 Master This: Comitant large angle esotropia in infants <6 months = Infantile esotropia (surgery), while same deviation at age 2-3 years = Rule out accommodative component (glasses first)
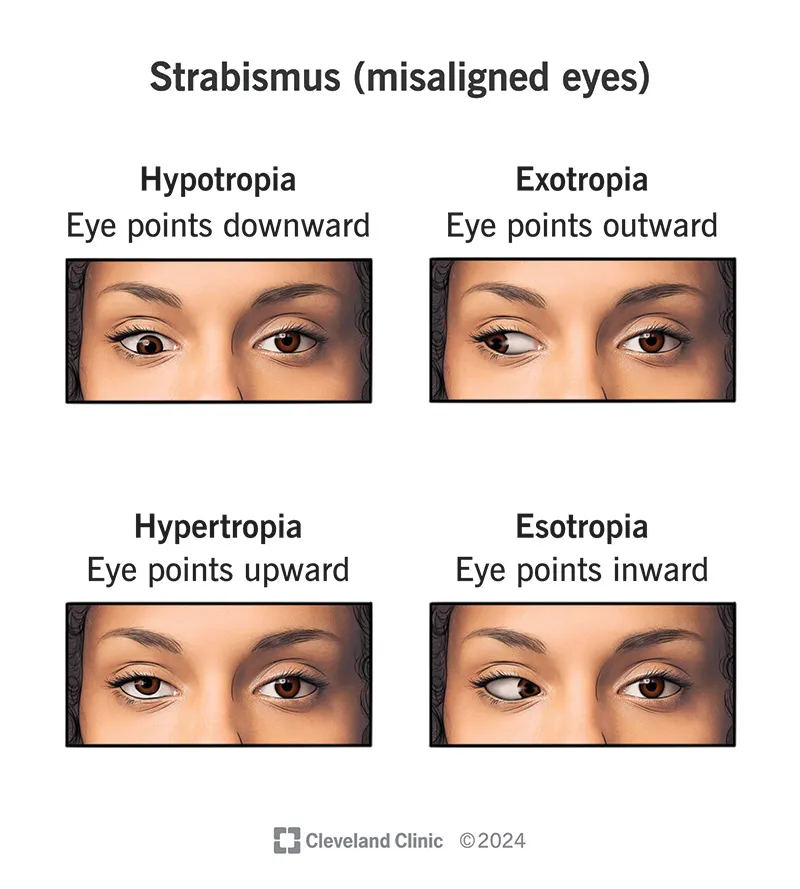
Treatment Algorithm Based on Differential:
- Infantile Esotropia: Surgery before 24 months for optimal binocular development
- Accommodative Esotropia: Full hyperopic correction, surgery only for residual deviation >15 PD
- Intermittent Exotropia: Surgery when control deteriorates or constant >50% time
- Paralytic Strabismus: Treat underlying cause, consider prisms or botulinum toxin
The differential matrix transforms pattern recognition into precise treatment algorithms, ensuring each strabismus type receives optimal management based on quantitative criteria rather than subjective assessment.
⚖️ Differential Mastery: The Strabismus Discrimination Matrix
🔧 Treatment Algorithms: The Precision Intervention Engine
📌 Remember: TIMING - Treat amblyopia first, Intervene during critical periods, Monitor progression, Individualize approach, Neuroplasticity windows, Gradual progression
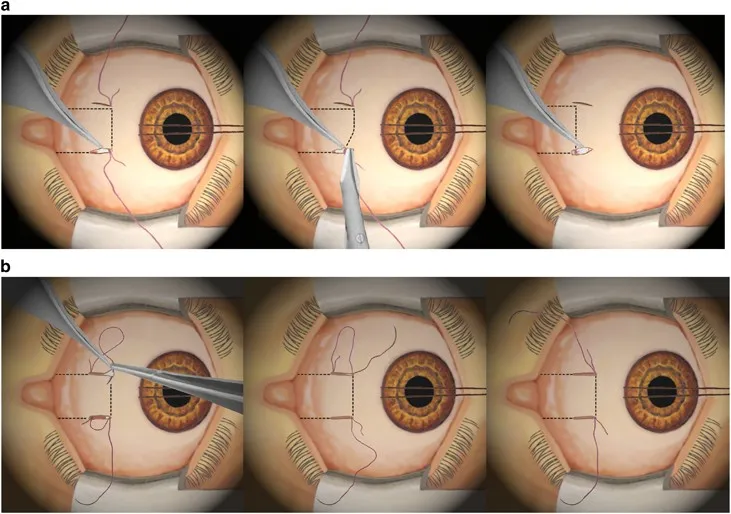
Primary Treatment Algorithm:
Amblyopia Treatment Protocols:
| Severity | Visual Acuity Difference | Treatment Protocol | Success Rate | Duration |
|---|---|---|---|---|
| Mild | 1-2 lines | 2 hours patching daily | 85-90% | 6-12 weeks |
| Moderate | 3-4 lines | 6 hours patching daily | 75-85% | 12-24 weeks |
| Severe | >4 lines | Full-time patching | 60-75% | 24-52 weeks |
| Dense | No fixation | Full-time + atropine | 40-60% | >52 weeks |
- Atropine penalization: 1% atropine daily in better eye, 80-85% effective as patching
- Optical penalization: +3.00D lens over better eye
- Bangerter filters: Graded occlusion (0.1-0.8 density)
- Binocular therapy: Dichoptic training showing promising results
⭐ Clinical Pearl: Amblyopia treatment must precede strabismus surgery - untreated amblyopia leads to surgical failure in 40-50% of cases due to poor fixation and sensory instability
Surgical Decision Matrix:
Infantile Esotropia Protocol:
- Age: Surgery before 24 months (optimal 6-18 months)
- Procedure: Bilateral medial rectus recession (4-6mm based on angle)
- Success: 80-90% achieve <10 PD residual deviation
- Binocular outcome: 65% develop some stereopsis when corrected early
Accommodative Esotropia Management:
- First-line: Full hyperopic correction (+0.25D over cycloplegic refraction)
- Success criteria: <10 PD residual deviation after 6-8 weeks
- Surgical indication: >15 PD residual after optimal glasses
- Procedure: Bilateral medial rectus recession (3-5mm)
Intermittent Exotropia Surgical Criteria:
- Frequency: Constant >50% of waking hours
- Control deterioration: Poor fusional control at distance
- Angle progression: >5 PD increase over 6 months
- Stereopsis loss: Deteriorating depth perception
| Exotropia Angle | Surgical Procedure | Success Rate | Overcorrection Risk |
|---|---|---|---|
| 15-20 PD | Unilateral LR recession | 70-80% | 5-10% |
| 25-35 PD | Bilateral LR recession | 75-85% | 10-15% |
| 40-50 PD | LR recession + MR resection | 80-90% | 15-20% |
| >50 PD | Bilateral LR recession + MR resection | 70-80% | 20-25% |
Muscle Recession Amounts:
- Medial rectus: 4-6mm for 30-50 PD esotropia
- Lateral rectus: 6-8mm for 25-40 PD exotropia
- Superior rectus: 3-5mm for 15-25 PD hypertropia
- Inferior rectus: 3-4mm for 10-20 PD hypotropia
Resection Guidelines:
- Maximum safe resection: 8mm for horizontal muscles, 5mm for vertical
- Typical amounts: 4-6mm for moderate strengthening procedures
- Combined procedures: Recession-resection for large angles (>40 PD)
💡 Master This: Surgical timing follows the "Rule of 2s" - Infantile esotropia before 2 years, accommodative after 2 months of glasses, intermittent exotropia when constant >2 hours daily
Post-operative Management Protocol:
Immediate (0-2 weeks):
- Antibiotic drops: 4 times daily for 1 week
- Activity restriction: No swimming for 2 weeks
- Follow-up: 1 week and 6 weeks post-operatively
Short-term (2-12 weeks):
- Alignment assessment: Target <10 PD residual deviation
- Diplopia management: Prisms if symptomatic
- Amblyopia monitoring: Resume treatment if regression
Long-term (3 months-2 years):
- Binocular function: Stereopsis testing at 3-6 months
- Stability assessment: <5 PD drift considered stable
- Reoperation rate: 15-20% require additional surgery
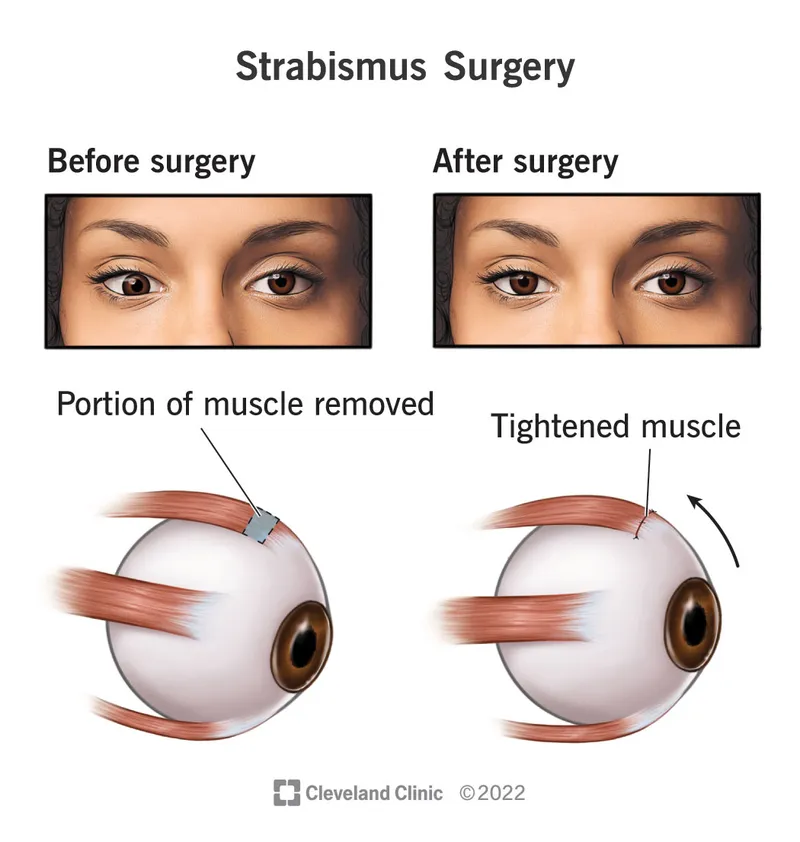
Treatment algorithms transform complex clinical decisions into systematic protocols, ensuring optimal outcomes through precise timing, appropriate technique selection, and comprehensive post-operative management.
🔧 Treatment Algorithms: The Precision Intervention Engine
🌐 Advanced Integration: The Pediatric Vision Ecosystem
📌 Remember: SYSTEM - Sensory-motor integration, Young brain plasticity, Stereopsis development, Timing coordination, Environmental factors, Multi-modal treatment
Neuroplasticity Revolution in Pediatric Ophthalmology:
Recent breakthrough research demonstrates extended plasticity windows beyond traditional critical periods:
- Amblyopia treatment: Effective up to age 17 years with intensive protocols
- Binocular therapy: Dichoptic training shows 40-60% improvement in adult amblyopia
- Perceptual learning: Contrast sensitivity improvements in teenagers with amblyopia
- Pharmacological enhancement: Fluoxetine + environmental enrichment reopens critical periods
Multi-System Integration Matrix:
| Primary Condition | Secondary Effects | Tertiary Consequences | Treatment Interactions |
|---|---|---|---|
| Strabismus | Suppression, diplopia | Amblyopia, stereopsis loss | Surgery timing affects amblyopia |
| Amblyopia | Poor fixation, nystagmus | Strabismus instability | Must treat before surgery |
| High Refractive Error | Accommodative esotropia | Amblyopia development | Glasses may cure strabismus |
| Ptosis | Deprivation amblyopia | Astigmatism, strabismus | Surgery timing critical |
| Cataract | Dense deprivation | Nystagmus, strabismus | Immediate surgery required |
Binocular Therapy Protocols:
- Dichoptic training: Separate images to each eye, forces binocular integration
- Success rates: 60-70% improvement in contrast sensitivity
- Stereopsis gains: 40-50% develop measurable stereopsis
- Treatment duration: 40-60 hours over 8-12 weeks
Pharmacological Adjuncts:
- Levodopa: 100mg daily enhances visual learning in amblyopia
- Citicoline: 500mg daily improves contrast sensitivity by 25-30%
- Fluoxetine: 20mg daily + environmental enrichment reopens plasticity
⭐ Clinical Pearl: Binocular therapy combined with traditional patching shows 30-40% faster amblyopia improvement compared to patching alone - the future is combination therapy
Environmental and Genetic Factors:
Risk Factor Analysis:
- Premature birth: 3-5x increased strabismus risk
- Family history: 40-50% heritability for strabismus
- Refractive error: >3.00D anisometropia carries 85% amblyopia risk
- Screen time: >2 hours daily associated with increased myopia and reduced stereopsis
Genetic Considerations:
- PHOX2A mutations: Associated with congenital fibrosis syndromes
- CHN1 mutations: Duane syndrome inheritance patterns
- TUBB3 mutations: Congenital cranial nerve dysinnervation
- PAX6 mutations: Aniridia with associated strabismus
Precision Medicine Approaches:
Individualized Treatment Protocols:
- Genetic testing: CFEOM, Duane syndrome variants guide surgical planning
- Biomarker assessment: BDNF levels predict amblyopia treatment response
- Neuroimaging: fMRI shows cortical plasticity changes during treatment
- Pharmacogenomics: CYP2D6 variants affect atropine metabolism
Technology Integration:
- Virtual reality therapy: Immersive binocular training protocols
- Eye tracking: Precise fixation monitoring during amblyopia treatment
- Smartphone apps: Home-based amblyopia therapy with compliance monitoring
- AI-assisted diagnosis: Automated strabismus measurement with 95% accuracy
💡 Master This: The "Pediatric Vision Triangle" - Structure (anatomy), Function (physiology), Development (time) - must be simultaneously optimized for maximum visual potential
Outcomes Research and Quality Metrics:
Long-term Success Indicators:
- Binocular single vision: >60 arcsec stereopsis at 5-year follow-up
- Educational performance: Normal reading speed and comprehension
- Quality of life: Pediatric Quality of Life inventory scores
- Surgical stability: <5 PD drift over 2-year period
Evidence-Based Benchmarks:
- Amblyopia treatment: >2 line improvement in 85% of patients
- Strabismus surgery: <10 PD residual deviation in 80% of cases
- Binocular outcomes: Stereopsis development in 65% of early-treated patients
- Reoperation rates: <20% for primary procedures
The pediatric vision ecosystem represents medicine's most time-sensitive specialty, where understanding system interactions and leveraging cutting-edge therapies transforms visual potential into lifelong success.
🌐 Advanced Integration: The Pediatric Vision Ecosystem
🎯 Clinical Mastery Arsenal: The Pediatric Vision Command Center
📌 Remember: MASTER - Measure precisely, Assess systematically, Surgery timing, Treat amblyopia first, Evaluate outcomes, Repeat as needed
Essential Numbers Arsenal:
Critical Age Thresholds:
- 6 weeks: Binocular vision onset
- 4 months: Intermittent deviations become abnormal
- 6 months: Stereopsis establishment
- 2 years: Optimal infantile esotropia surgery
- 7 years: Traditional amblyopia critical period
- 17 years: Extended plasticity window
Measurement Precision Standards:
- Hirschberg: 1mm displacement = 15 PD
- Krimsky: Prism neutralization accuracy ±2 PD
- Cover test: Gold standard for deviation measurement
- AC/A ratio: Normal 3-5:1, high >6:1, low <3:1
| Quick Reference | Normal Values | Abnormal Thresholds | Action Required |
|---|---|---|---|
| Stereoacuity | 40-60 arcsec | >200 arcsec | Evaluate binocularity |
| Visual Acuity | 20/20 by age 5 | >2 line difference | Amblyopia treatment |
| Deviation Size | <5 PD phoria | >15 PD tropia | Consider surgery |
| Fixation Pattern | Central, steady | Eccentric/unsteady | High amblyopia risk |
| Pupil Response | Equal, reactive | APD present | Rule out pathology |
30-Second Screening:
- Visual behavior: Fixation preference, following patterns
- Alignment: Hirschberg test, cover-uncover
- Motility: Smooth pursuits, saccades
- Pupils: Size, reactivity, APD
2-Minute Evaluation:
- Visual acuity: Age-appropriate methods
- Complete cover testing: Primary and secondary gazes
- Stereopsis: Titmus or Randot testing
- Cycloplegic refraction: Essential for accurate assessment
⭐ Clinical Pearl: The "Rule of 15s" - 15 PD minimum for surgical consideration, 15 degrees head turn suggests significant palsy, 15% overcorrection risk with bilateral procedures
Treatment Decision Matrix:
Surgical Planning Quick Reference:
Recession Amounts (mm):
- Small angle (15-25 PD): 3-4mm
- Moderate angle (25-40 PD): 4-6mm
- Large angle (40-60 PD): 6-8mm
Success Prediction Factors:
- Early surgery (<24 months): 80-90% success
- Good preoperative vision: 85-95% success
- Comitant deviation: 75-85% success
- Incomitant deviation: 60-75% success
Complication Prevention:
High-Risk Scenarios:
- Previous surgery: 20-30% increased complication risk
- Restrictive conditions: Higher undercorrection rates
- Poor vision: Increased reoperation likelihood
- Systemic conditions: Modified healing responses
💡 Master This: Amblyopia treatment intensity follows "Dose-Response" - Mild amblyopia needs 2 hours daily, severe requires 6+ hours, dense demands full-time patching
Outcome Monitoring Checklist:
Immediate Post-op (1-6 weeks):
- Alignment: Target <10 PD residual
- Motility: Full range expected
- Diplopia: Temporary in 20-30%
- Infection signs: <1% incidence
Long-term Success (6 months-2 years):
- Stability: <5 PD drift acceptable
- Binocularity: Stereopsis development
- Functional vision: Reading, sports performance
- Quality of life: Confidence, social interaction
Red Flag Monitoring:
Immediate Concerns:
- Sudden vision loss: Rare but urgent
- Severe pain: Unusual post-operatively
- Excessive inflammation: May indicate infection
- Lost muscle: Requires immediate re-exploration
Long-term Vigilance:
- Progressive drift: >5 PD change over 6 months
- Amblyopia recurrence: Vision deterioration
- Diplopia persistence: >3 months post-surgery
- Functional limitations: Reading, driving difficulties
Essential Clinical Pearls:
- Timing trumps technique - perfect surgery at wrong age yields poor outcomes
- Amblyopia first - untreated amblyopia sabotages surgical success
- Binocular potential decreases exponentially with delayed treatment
- Family compliance determines treatment success more than severity
- Long-term monitoring essential - stability takes 2+ years to establish
The clinical mastery arsenal transforms pediatric ophthalmology complexity into systematic excellence, ensuring every child achieves maximum visual potential through precise assessment, optimal timing, and evidence-based intervention.
🎯 Clinical Mastery Arsenal: The Pediatric Vision Command Center
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more
Have doubts about this lesson?
Ask Rezzy, your AI Study Mate, to explain anything you didn't understand
Everything you need for NEET-PG prep
Get full Oncourse access with lessons, practice questions, flashcards and AI study tools.
Scan to download app












