Pregnancy-Related Eye Changes - Baby's Eye Perks
- Cornea:
- ↑ Thickness & curvature (due to edema) → transient myopic shift (avg. -0.5 to -1.0 D), astigmatic changes.
- Contact lens intolerance common.
- Intraocular Pressure (IOP):
- ↓ IOP (typically 2-3 mmHg), more pronounced in 2nd/3rd trimesters.
- Mechanism: ↑ uveoscleral outflow, hormonal effects (progesterone).
- Tear Film & Conjunctiva:
- Altered tear film (↓ lysozyme, ↑ mucin) → dry eye symptoms (keratoconjunctivitis sicca).
- Conjunctival vasodilation.
- Other Physiological Changes:
- Mild ptosis (fluid retention).
- Chloasma (pigmentary changes on eyelids/periorbital skin).
- Krukenberg spindles may become more prominent (benign).
- Transient ↓ accommodative amplitude (rare).
⭐ A transient myopic shift and contact lens intolerance are common due to corneal edema and changes in corneal curvature.
📌 Mnemonic: PERKS of Pregnancy Eyes
- Ptosis (mild)
- Edema (corneal) → Refractive changes
- Refractive shift (myopia)
- Krukenberg spindles
- Sicca (dry eyes) / Sensitivity to contact lenses
Pregnancy-Related Eye Changes - Vision Alarms
-
Preeclampsia/Eclampsia:
- Symptoms: Blurred vision, photopsia, scotomas, diplopia.
- Signs: Hypertensive retinopathy (retinal arteriolar narrowing, hemorrhages, cotton wool spots, exudates), papilledema, serous retinal detachment.
- ⚠️ Severe: Cortical blindness (occipital ischemia/edema).
-
Central Serous Chorioretinopathy (CSCR):
- Acute ↓ vision, metamorphopsia, micropsia, central scotoma.
- Typically 3rd trimester/postpartum.
⭐ Central Serous Chorioretinopathy (CSCR) is a key cause of acute vision loss in late pregnancy/postpartum, often resolving spontaneously.
-
Pituitary Adenoma Enlargement:
- Pre-existing pituitary adenomas may enlarge.
- Symptom: Bitemporal hemianopia.
- Urgent neuro-ophthalmic referral.
-
Other Grave Conditions:
- DIC (Disseminated Intravascular Coagulation): With HELLP/abruption. Ocular: Choroidal infarcts, serous retinal detachment, retinal/vitreous hemorrhages.
- Uveitis: Variable course. Toxoplasmosis reactivation. Vogt-Koyanagi-Harada (VKH) syndrome may trigger/worsen.
- Purtscher-like Retinopathy: Rare; associated with pancreatitis, amniotic fluid embolism.
Pregnancy-Related Eye Changes - Old Foes, New Rules
Pregnancy modifies existing eye conditions and their management, presenting unique challenges.
-
Diabetic Retinopathy (DR)
- Can significantly worsen. Risk factors: DM duration, baseline DR severity, poor glycemic control (HbA1c), hypertension, nephropathy.
- Management:
- Pre-conception counseling & optimization.
- Meticulous glycemic control (Target HbA1c < 6.5%).
- Regular ophthalmic exams:
- No DR / Mild NPDR: 1st trimester, then as indicated.
- Moderate NPDR: Each trimester.
- Severe NPDR / PDR: Monthly or more frequently.
- Laser photocoagulation: Safe and effective.
- Anti-VEGF (e.g., Bevacizumab, Ranibizumab): Generally avoided (Category C); consider only for vision-threatening PDR if laser fails/not possible.
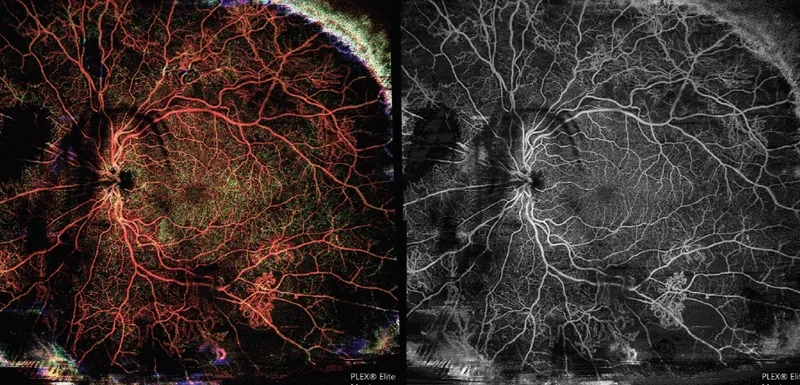
⭐ Diabetic retinopathy can significantly worsen during pregnancy; meticulous glycemic control and regular ophthalmic exams (at least once per trimester) are paramount.
-
Glaucoma
- IOP often ↓ (↑ progesterone, ↑ uveoscleral outflow, ↑ aqueous outflow facility).
- Medication safety is key (see flowchart below).
- Selective Laser Trabeculoplasty (SLT) preferred over incisional surgery if intervention needed.
-
Other Conditions
- Central Serous Chorioretinopathy (CSCR): May occur/worsen, often bilateral; usually self-limiting postpartum.
- Uveitis: Course is variable. Immunosuppression requires careful selection (e.g., avoid methotrexate).
- Idiopathic Intracranial Hypertension (IIH): Weight gain can exacerbate. Acetazolamide (Cat C) used cautiously if benefits outweigh risks.
- Refractive Changes: Transient myopic shift due to corneal edema & ↑ thickness. Delay new spectacle Rx until stable postpartum.
- Pituitary Adenoma: Pre-existing adenomas may enlarge, causing visual field defects (bitemporal hemianopia).
- Pre-eclampsia/Eclampsia: Ocular signs include retinal vasospasm, serous retinal detachments, cortical blindness.
High‑Yield Points - ⚡ Biggest Takeaways
- Physiological corneal edema and ↑ thickness cause transient refractive shifts & contact lens intolerance.
- Intraocular pressure (IOP) typically ↓ decreases, often by 10-20%.
- Preeclampsia/Eclampsia can induce severe hypertensive retinopathy, serous retinal detachment, and even cortical blindness.
- Central Serous Chorioretinopathy (CSCR) may develop or worsen, especially in the third trimester.
- Diabetic retinopathy can progress rapidly; regular fundus screening is vital.
- Pituitary adenomas may enlarge, causing bitemporal hemianopia or other visual field defects.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

