Retina & Optic Nerve - Eye's First Signals
- Retina: Converts light to neural signals; innermost eye layer.
- Photoreceptors:
- Rods: Scotopic (night, dim light) vision, peripheral retina, rhodopsin. ~120 million.
- Cones: Photopic (daylight, color) vision, central retina (fovea), iodopsin. ~6 million. 📌 Cones = Color, Central.
- Fovea Centralis: Highest cone density, site of sharpest visual acuity. Located in macula lutea.
- Ganglion Cell Layer (GCL): Axons converge to form the optic nerve.
- Photoreceptors:
- Optic Nerve (CN II): Transmits visual information from retina to brain.
- Composed of ~1.2 million GCL axons.
- Optic Disc (Papilla): Physiological blind spot (no photoreceptors); where optic nerve exits and central retinal artery/vein enter/exit.
- Myelination: Begins posterior to lamina cribrosa (by oligodendrocytes).
⭐ The central retinal artery and vein pierce the optic nerve approximately 1.25 cm behind the globe.
Optic Chiasm & Tract - The Great Crossover
- Optic Chiasm: X-shaped, anterior to pituitary.
- Nasal retinal fibers (medial) decussate (cross).
- Temporal retinal fibers (lateral) remain ipsilateral (do not cross).
- Optic Tract: Posterior to chiasm.
- Contains ipsilateral temporal & contralateral nasal fibers.
- Left Tract: Carries Right visual field information.
- Right Tract: Carries Left visual field information.
- Projects to Lateral Geniculate Body (LGB).
⭐ Pituitary adenomas are a common cause of bitemporal hemianopia due to compression of the decussating nasal fibers at the optic chiasm.
LGN & Optic Radiations - Relay & Fan Out
- Lateral Geniculate Nucleus (LGN): Thalamic visual relay.
- Has 6 layers:
- Layers 1, 4, 6: Input from contralateral nasal retina.
- Layers 2, 3, 5: Input from ipsilateral temporal retina.
- Magnocellular (M) layers (1,2): Motion, depth (Where pathway).
- Parvocellular (P) layers (3-6): Color, fine detail (What pathway).
- Has 6 layers:
- Optic Radiations: LGN axons to primary visual cortex (Brodmann area 17).
- Superior fibers (via parietal lobe): Carry inferior visual field information.
- Inferior fibers (Meyer's Loop, via temporal lobe): Carry superior visual field information.
- 📌 Mnemonic: PITS (Parietal-Inferior field defect, Temporal-Superior field defect).
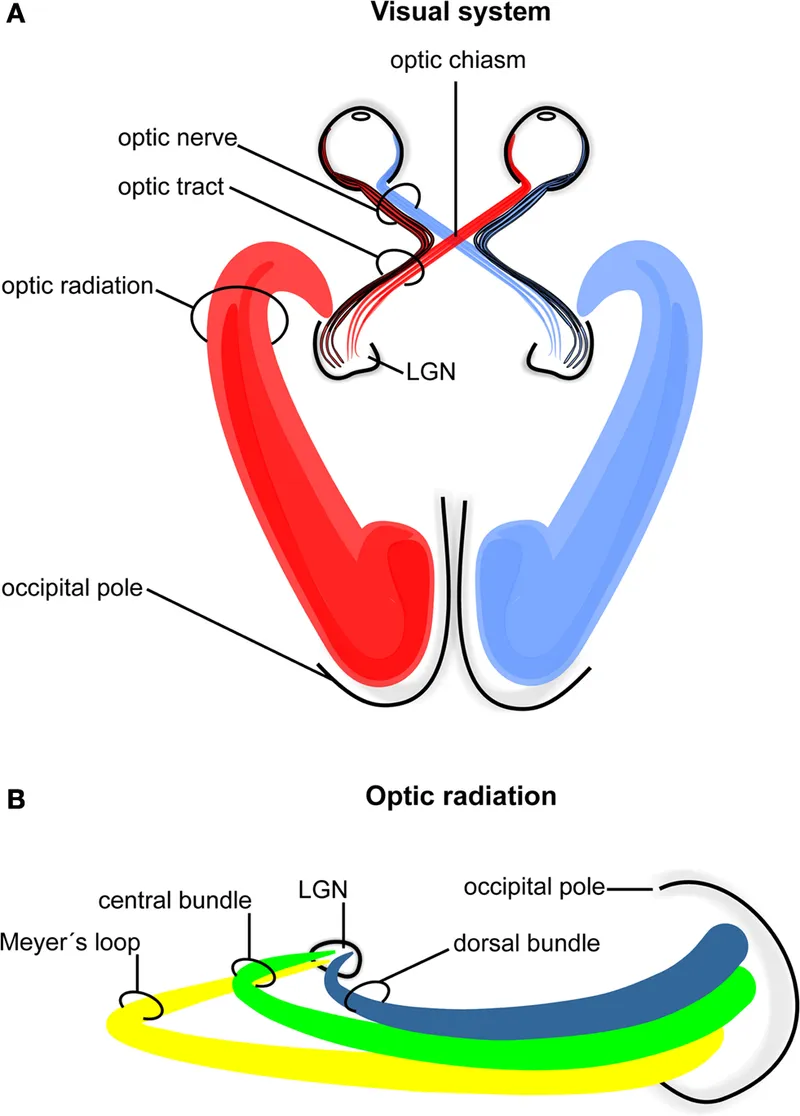
⭐ Lesions of Meyer's loop (temporal lobe) cause a contralateral superior quadrantanopia ('pie in the sky').
Visual Cortex & Blood Supply - Brain's Vision HQ
- Primary Visual Cortex (V1): Brodmann area 17; located in occipital lobe, primarily on banks of calcarine sulcus.
- Function: Initial, detailed processing of visual stimuli (form, motion, color).
- Retinotopic Organization: Precise point-to-point projection from retina.
- Cuneus gyrus (superior bank of calcarine sulcus): Represents contralateral lower visual field.
- Lingual gyrus (inferior bank of calcarine sulcus): Represents contralateral upper visual field.
- Macula: Largest cortical representation, located at posterior occipital pole.
- Blood Supply:
- Mainly Posterior Cerebral Artery (PCA).
- Occipital pole (macular cortex): Often receives dual supply from PCA & Middle Cerebral Artery (MCA).
⭐ Macular sparing in posterior cerebral artery (PCA) occlusion is often attributed to dual blood supply to the occipital pole (macular cortex) from both PCA and middle cerebral artery (MCA).
- Clinical Significance: PCA occlusion typically causes contralateral homonymous hemianopia; macular sparing is common due to dual supply.
High‑Yield Points - ⚡ Biggest Takeaways
- Nasal retinal fibers cross at optic chiasm; temporal fibers do not.
- Optic tracts synapse in the Lateral Geniculate Nucleus (LGN).
- Optic radiations link LGN to primary visual cortex (occipital lobe).
- Meyer's loop (temporal lobe) carries superior visual field info; lesions cause "pie in the sky".
- Baum's loop (parietal lobe) carries inferior visual field info; lesions cause "pie on the floor".
- Macula has large, posterior representation in visual cortex.
- Chiasmal lesions typically cause bitemporal hemianopia.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more


