UI Basics - Leaky Pipes 101
- Definition: Any involuntary leakage of urine.
- A common & distressing symptom; significantly impacts quality of life (QoL).
- Risk factors: ↑ Age, parity, obesity, menopause, previous pelvic surgery.
- Main classifications:
- Stress UI (SUI)
- Urgency UI (UUI) / Overactive Bladder (OAB)
- Mixed UI (MUI)
- Overflow UI
- Functional UI
⭐ Urinary incontinence (UI) is the complaint of any involuntary leakage of urine. It is NOT a normal part of aging, though its prevalence increases with age.
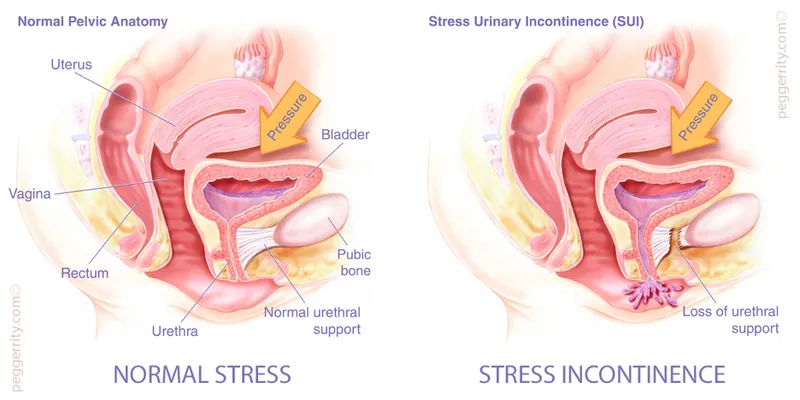
Stress UI - Cough & Sneeze Leaks
- Involuntary urine loss on effort or exertion (e.g., coughing, sneezing, laughing, lifting).
- Primary Mechanisms:
- Urethral Hypermobility: Weak pelvic floor support leads to downward/rotational descent of urethra & bladder neck.
- Intrinsic Sphincter Deficiency (ISD): Weakness of the urethral sphincter's closing mechanism.
- Common Risk Factors:
- Pregnancy, childbirth (especially vaginal).
- Obesity, chronic cough, constipation.
- Menopause (↓ estrogen).
- Previous pelvic surgery.
- Diagnostic Clues:
- History of leakage with physical stress.
- Positive cough stress test (observed leakage).
⭐ In Stress Urinary Incontinence (SUI), a positive Q-tip test (angle > 30 degrees from horizontal with Valsalva) suggests urethral hypermobility.
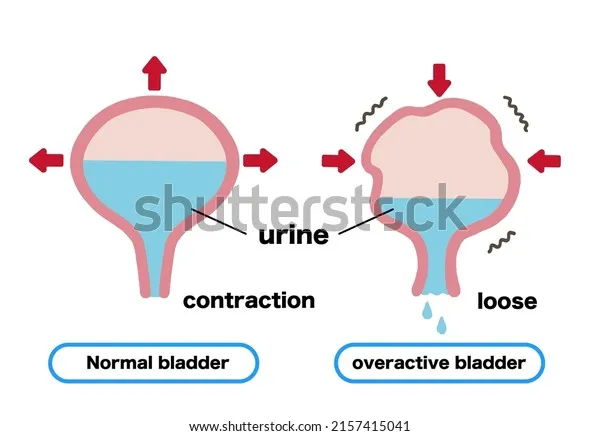
Urgency UI/OAB - Gotta Go NOW!
- UUI: Involuntary urine leakage with/preceded by urgency.
- OAB Syndrome: Urgency (key), often with frequency (>8/24h) & nocturia (>1/night), +/- UUI.
- Pathophysiology: Detrusor Overactivity (DO) - involuntary bladder contractions during filling.
- Idiopathic (most common) or Neurogenic.
- Triggers: 📌 Key-in-lock phenomenon, running water, cold.
⭐ Detrusor overactivity is the most common urodynamic finding in patients with Urgency Urinary Incontinence (UUI); Overactive Bladder (OAB) is a syndrome of urgency, usually with frequency and nocturia, +/- UUI.
- Management:
- Behavioral (bladder training)
- Meds (antimuscarinics, β3-agonists)
- Advanced (Botox, neuromodulation)
Mixed & Overflow UI - Combo & The Dam
- Mixed UI:
- Combination of Stress UI (SUI) and Urgency UI (UUI).
- Patient experiences symptoms of both involuntary leakage on effort/exertion AND urgency with leakage.
- Common, especially in older women.
- Overflow UI: 📌 (Mnemonic: "The Dam is Full")
- Involuntary urine loss when bladder pressure exceeds urethral pressure due to bladder overdistension, without detrusor contraction.
- Causes:
- Bladder Outlet Obstruction (BOO): e.g., BPH, urethral stricture, severe pelvic organ prolapse.
- Detrusor Underactivity: e.g., neurogenic (diabetes, MS), myogenic, medications (anticholinergics).
- Symptoms: Dribbling, weak stream, hesitancy, nocturia, feeling of incomplete emptying.
⭐ A post-void residual (PVR) urine volume > 200 mL is often indicative of overflow incontinence or significant bladder emptying dysfunction.
Functional & Transient UI - Odd Jobs & Quick Fixes
- Functional UI: Due to cognitive/physical impairments (e.g., dementia, immobility) preventing toilet use.
- Transient UI: Temporary, often reversible causes.
- 📌 Key: DIAPPERS mnemonic.
⭐ The 'DIAPPERS' mnemonic (Delirium, Infection, Atrophic urethritis/vaginitis, Pharmaceuticals, Psychological, Excess urine output, Restricted mobility, Stool impaction) is crucial for identifying reversible causes of transient incontinence.
High‑Yield Points - ⚡ Biggest Takeaways
- SUI: Leakage on effort (cough, sneeze); due to urethral hypermobility or Intrinsic Sphincter Deficiency (ISD).
- UUI: Leakage with urgency; due to detrusor overactivity.
- MUI: Combination of SUI and UUI symptoms.
- Overflow Incontinence: Dribbling from overfull bladder; due to detrusor underactivity or bladder outlet obstruction; ↑ PVR.
- Continuous Incontinence: Constant leakage; suspect urinary fistula (e.g., Vesicovaginal Fistula - VVF).
- Urodynamics (UDS): Key for complex cases or before incontinence surgery.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more