Rectocele & Enterocele: Definitions & Anatomy - Posterior Prolapse Primer
- Posterior Compartment Prolapse:
- Rectocele: Herniation of the rectum against the posterior vaginal wall. Caused by defects in the rectovaginal septum.
- Enterocele: Herniation of the small bowel (Pouch of Douglas) into the upper posterior vaginal fornix. Due to weakness in uterosacral/cardinal ligaments.
- Key Anatomical Supports:
- Rectovaginal septum (fibromuscular layer)
- Perineal body (central anchor)
- Uterosacral & Cardinal ligaments (apical suspension)
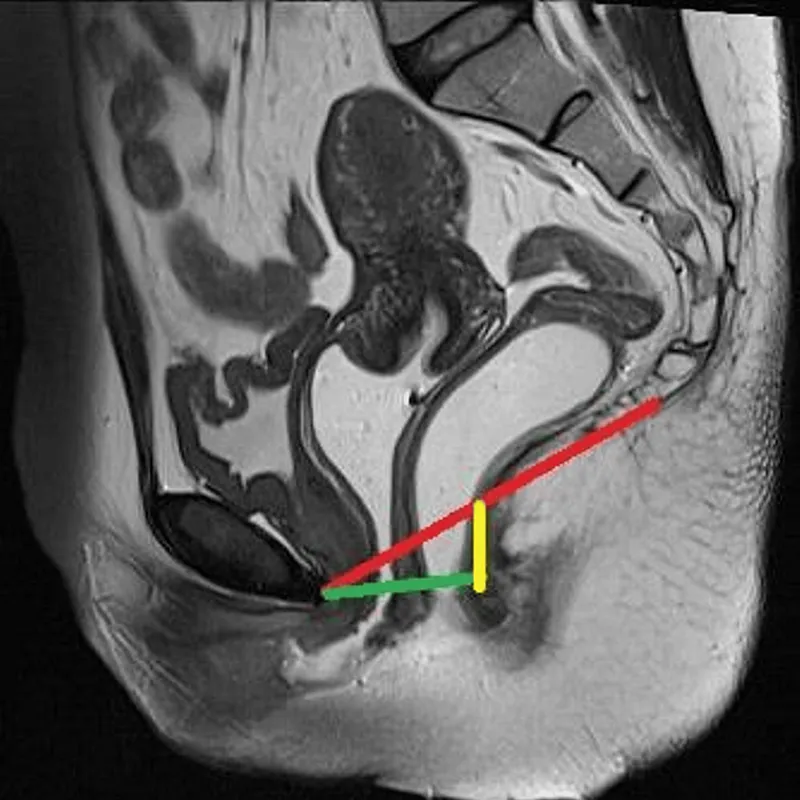
⭐ Enteroceles represent a true herniation of the cul-de-sac (Pouch of Douglas), typically containing loops of small bowel.
Rectocele & Enterocele: Etiology & Risk Factors - Why Walls Weaken
- Fundamental Cause: Weakening/damage to endopelvic fascia, levator ani muscles, and perineal body.
- Key Predisposing Factors:
- Obstetric: Vaginal birth (esp. instrumental, prolonged 2nd stage, macrosomia), multiparity.
- Pressure: Chronic ↑ intra-abdominal pressure (constipation, cough, obesity, heavy lifting).
- Hormonal/Age: Menopause (↓estrogen), advancing age (tissue degeneration).
- Iatrogenic: Prior pelvic surgeries (hysterectomy particularly for enterocele).
- Constitutional: Genetic predisposition, connective tissue disorders.
⭐ Hysterectomy is a major risk factor for enterocele development by disrupting apical vaginal support.
Rectocele & Enterocele: Clinical Features - Symptoms Unveiled
- Rectocele (Posterior Compartment):
- Vaginal bulge/mass sensation, often posterior.
- Defecatory dysfunction:
- Constipation, straining.
- Incomplete bowel emptying.
- Splinting (digital pressure on posterior vagina/perineum to evacuate).
- Pelvic pressure/heaviness, low back pain.
- Dyspareunia (occasional).
- Enterocele (Small Bowel Herniation):
- Vaginal bulge (upper posterior/apical).
- Pelvic pressure, aching, fullness.
- Symptoms worsen with prolonged standing/straining.
- Low back pain.
- Often coexists with other Pelvic Organ Prolapse (POP); may be asymptomatic.
⭐ Splinting - manually pressing perineum/posterior vaginal wall to aid defecation - is highly specific for rectocele.
Rectocele & Enterocele: Diagnosis & Staging - Seeing & Scoring Sag
- Diagnosis:
- Clinical Exam: Valsalva maneuver, Sims speculum reveals posterior vaginal bulge.
- Differentiation:
- Rectocele: Bulge of rectum into posterior vagina.
- Enterocele: Herniation of small bowel (peritoneal sac) into upper posterior vagina, often superior to rectocele.
- Rectovaginal exam: Assesses rectovaginal septum integrity (thinned in rectocele).
- Staging Systems:
- POP-Q (Pelvic Organ Prolapse Quantification): Standard, objective. Point Bp (most distal point on posterior vaginal wall) is key for rectocele.
- Stage 0: No prolapse.
- Stage I: Leading edge >1 cm above hymen (value < -1 cm).
- Stage II: Leading edge between -1 cm and +1 cm relative to hymen.
- Stage III: Leading edge >1 cm below hymen, but < (TVL-2) cm. (TVL = Total Vaginal Length)
- Stage IV: Complete eversion; leading edge ≥ (TVL-2) cm.
- Baden-Walker System: Simpler, less precise (Grades 0-4).
- POP-Q (Pelvic Organ Prolapse Quantification): Standard, objective. Point Bp (most distal point on posterior vaginal wall) is key for rectocele.
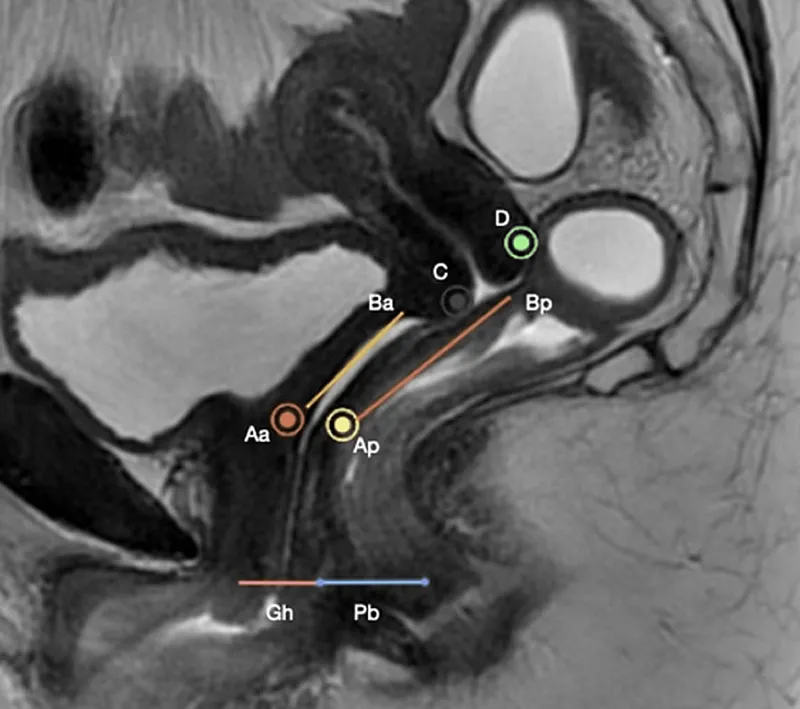
⭐ Enterocele typically involves the herniation of the small bowel and is often found superior and posterior to a rectocele; it may become more apparent when the patient is standing or straining.
Rectocele & Enterocele: Management - Fixing the Flaw
- Conservative (Mild/Asymptomatic): 📌 Mnemonic: PELT
- Pessary.
- Estrogen (topical, if atrophy).
- Lifestyle: ↑Fiber, fluids, weight control, avoid strain.
- Training (Pelvic Floor Muscle Training - PFMT).
- Surgical (Symptomatic/Failed Conservative):
- Goal: Restore anatomy, relieve symptoms.
- **Rectocele Repair:** Posterior Colporrhaphy (transvaginal fascial plication). Mesh for complex/recurrent.
- **Enterocele Repair:** Vaginal (McCall culdoplasty, USLS) or Abdominal (Sacrocolpopexy - apical).
> ⭐ McCall culdoplasty, often with vaginal hysterectomy, supports vaginal apex, preventing future enterocele.
High‑Yield Points - ⚡ Biggest Takeaways
- Rectocele: Posterior vaginal wall prolapse from rectovaginal septum defects; presents with constipation, splinting, incomplete evacuation.
- Enterocele: Small bowel herniation into upper posterior vagina, often iatrogenic (post-hysterectomy) or from a deep Pouch of Douglas.
- Enterocele symptoms: vaginal bulge, pelvic pressure, worsening on standing.
- POP-Q system is crucial for objective assessment and staging.
- Management: Conservative (Kegels, pessaries) or surgical repair (posterior colporrhaphy, McCall culdoplasty).
- Multiparity and connective tissue disorders are significant risk factors for both.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

