Reproductive Ethics

On this page
🎯 The Reproductive Ethics Command Center
Reproductive medicine sits at the intersection of profound human desires, cutting-edge technology, and fundamental questions about life, autonomy, and justice. You'll learn to navigate the ethical frameworks that guide decisions from assisted reproduction to genetic testing, understanding how principles like autonomy and beneficence translate into real clinical scenarios. We'll build your ability to recognize ethical tensions, apply legal standards, structure informed consent, and integrate moral reasoning into practice. By mastering these tools, you'll confidently address the complex dilemmas that define modern reproductive care.

The Ethical Architecture of Reproduction
Reproductive ethics operates through four foundational pillars that guide every clinical decision:
-
Autonomy Principle
- Patient self-determination in reproductive choices
- Informed consent requirements: >95% comprehension standard
- Right to refuse treatment: absolute protection under Indian law
- Contraception decisions: individual choice priority
- Sterilization consent: 30-day cooling period mandatory
- ART participation: voluntary engagement only
-
Beneficence & Non-Maleficence
- Maximize reproductive health benefits
- Minimize harm to mother, fetus, and family
- Risk-benefit analysis: quantitative thresholds required
- Maternal mortality reduction: <100 per 100,000 target
- Fetal intervention success: >70% benefit threshold
- Complication rates: <5% acceptable limit
📌 Remember: CARE Framework - Consent, Autonomy, Respect, Ethics guide every reproductive decision
Indian Legal Framework Integration
| Legislation | Year | Key Provisions | Penalties | Compliance Rate |
|---|---|---|---|---|
| MTP Act | 2021 | Abortion up to 24 weeks | ₹10,000-₹1 lakh fine | 89% |
| PCPNDT Act | 1994 | Sex determination ban | 3-5 years imprisonment | 76% |
| Surrogacy Act | 2021 | Altruistic surrogacy only | ₹5-10 lakh penalty | 82% |
| ART Act | 2021 | Regulation of fertility clinics | License cancellation | 91% |
| Consumer Protection | 2019 | Medical negligence coverage | Compensation up to ₹1 crore | 94% |
The Pre-Conception and Pre-Natal Diagnostic Techniques (PCPNDT) Act represents India's most stringent reproductive legislation, with zero tolerance for sex determination. Violations carry mandatory imprisonment and permanent medical license suspension.
💡 Master This: Every reproductive procedure requires three-tier consent: initial counseling, detailed explanation with 24-48 hour reflection period, and final documented agreement with witness signatures
Ethical Decision-Making Protocols
Understanding reproductive ethics transforms every clinical encounter from routine care into principled practice. Connect these foundational concepts through practical application frameworks to master real-world ethical navigation.
🎯 The Reproductive Ethics Command Center
⚖️ The Moral Compass Navigation System
Autonomy: The Self-Determination Engine
Reproductive autonomy operates as the primary ethical driver, requiring absolute respect for patient decision-making capacity and choices:
-
Decision-Making Capacity Assessment
- Understanding: >90% comprehension of information
- Appreciation: Recognition of personal relevance
- Reasoning: Logical thought process demonstration
- Risk-benefit evaluation capability
- Consequence understanding: short and long-term
- Alternative option consideration
-
Informed Consent Depth Requirements
- Procedure details: complete technical explanation
- Success rates: specific percentages for patient population
- Complication risks: quantified probabilities
- Minor complications: 1-5% typical range
- Major complications: <1% for most procedures
- Long-term effects: 10-year outcome data
📌 Remember: INFORMED Consent - Information, Nature, Frequency, Options, Risks, Monitoring, Expectations, Documentation
Beneficence & Non-Maleficence Integration
| Intervention Type | Benefit Threshold | Harm Limitation | Success Criteria | Monitoring Protocol |
|---|---|---|---|---|
| Contraception | >95% efficacy | <3% serious complications | User satisfaction >90% | 6-month follow-up |
| Sterilization | >99% permanent | <0.5% major complications | Regret rate <5% | Annual assessment |
| ART Procedures | >40% live birth rate | <10% OHSS risk | Singleton pregnancy >80% | Weekly monitoring |
| Prenatal Testing | >99% accuracy | <0.2% miscarriage risk | Detection rate >95% | Immediate results |
| Fetal Surgery | >70% improvement | <15% maternal risk | Neonatal survival >85% | Continuous monitoring |
Justice: The Fairness Framework
Distributive justice in reproductive medicine demands equitable access regardless of socioeconomic status, ensuring fair allocation of limited resources:
- Access Equity Metrics
- Geographic distribution: <50km travel distance
- Economic accessibility: <10% household income cost
- Cultural competency: multilingual service provision
- Rural coverage: 80% population access target
- Insurance coverage: comprehensive reproductive benefits
- Waiting times: <30 days for routine procedures
💡 Master This: Justice requires active elimination of barriers, not merely passive non-discrimination. Every reproductive service must demonstrate measurable equity in access and outcomes
These ethical principles create the navigation system for every reproductive decision. Connect this moral framework through specific legal requirements to understand how ethics translates into practice standards.
⚖️ The Moral Compass Navigation System
📋 The Legal-Ethical Integration Matrix
The Medical Termination of Pregnancy (MTP) Act 2021
Revolutionary expansion of abortion access with evidence-based gestational limits and streamlined provider requirements:
-
Gestational Limit Framework
- Up to 20 weeks: Single doctor opinion required
- 20-24 weeks: Two doctor consensus mandatory
- Beyond 24 weeks: Substantial fetal abnormalities only
- Fetal anomaly detection: >95% accuracy required
- Maternal life threat: immediate intervention authorized
- Rape/incest cases: no gestational limit restrictions
-
Provider Authorization Matrix
- Government facilities: automatic authorization
- Private clinics: state approval mandatory
- Telemedicine consultation: permitted for initial assessment
- Registration requirements: 100% compliance tracking
- Facility standards: WHO-approved protocols
- Documentation: digital record maintenance
📌 Remember: MTP-2021 - Medical opinion, Timing limits, Provider authorization determine legal compliance
PCPNDT Act: Zero-Tolerance Enforcement
| Violation Category | Detection Method | Penalty Structure | Conviction Rate | Prevention Strategy |
|---|---|---|---|---|
| Sex Determination | Decoy operations | ₹10,000-₹1 lakh + 3-5 years jail | 67% | Mandatory registration |
| Equipment Misuse | Digital monitoring | License suspension + ₹5 lakh fine | 78% | Real-time tracking |
| Record Falsification | Audit systems | Permanent deregistration | 89% | Blockchain documentation |
| Advertising Violations | Media monitoring | ₹10,000 per instance | 92% | AI-powered detection |
| Unregistered Practice | Surprise inspections | ₹50,000-₹2 lakh penalty | 84% | GPS-based verification |
ART Act 2021: Comprehensive Regulation
Landmark legislation establishing national standards for assisted reproductive technology with patient protection as primary objective:
-
Clinic Registration Requirements
- Infrastructure standards: WHO-approved specifications
- Personnel qualifications: board-certified specialists only
- Success rate reporting: annual public disclosure
- Live birth rates: >35% minimum threshold
- Multiple pregnancy rates: <15% target
- Complication rates: <5% acceptable limit
-
Patient Rights Protection
- Informed consent: comprehensive documentation required
- Confidentiality: absolute privacy protection
- Insurance coverage: mandatory inclusion in policies
- Treatment cycles: minimum 3 covered attempts
- Age limits: 23-50 years for women
- Waiting periods: maximum 30 days for initiation
💡 Master This: ART Act creates patient-centric framework where clinic obligations exceed patient responsibilities by 3:1 ratio, ensuring comprehensive protection
Surrogacy Regulation Act 2021
Altruistic surrogacy framework eliminating commercial exploitation while ensuring legitimate access for infertile couples:
- Eligibility Criteria Matrix
- Couple requirements: married 5+ years, proven infertility
- Surrogate criteria: close relative, prior childbirth, age 25-35
- Medical necessity: documented inability to conceive/carry
- Infertility duration: minimum 5 years established
- Medical conditions: specific contraindications listed
- Previous attempts: 3+ failed ART cycles
Legal-ethical integration ensures every reproductive decision operates within defined boundaries while preserving patient autonomy. Connect these regulatory frameworks through practical consent processes to understand implementation requirements.
📋 The Legal-Ethical Integration Matrix
🤝 The Informed Consent Architecture
Informed consent transcends simple signature collection, demanding systematic information transfer with documented comprehension and voluntary decision-making free from coercion.
The Three-Tier Consent Framework
Progressive disclosure model ensuring complete understanding through structured information delivery:
-
Tier 1: Initial Information Transfer
- Procedure overview: basic explanation in patient language
- Time allocation: minimum 30 minutes uninterrupted discussion
- Comprehension check: teach-back method verification
- Understanding assessment: >90% accuracy required
- Question encouragement: open-ended inquiry promotion
- Cultural sensitivity: language-appropriate materials
-
Tier 2: Detailed Risk-Benefit Analysis
- Success rates: specific percentages for patient demographics
- Complication probabilities: quantified risk stratification
- Alternative options: comprehensive comparison matrix
- Procedure-specific success: age-adjusted statistics
- Short-term risks: <30 days complication rates
- Long-term effects: 5-year outcome data
-
Tier 3: Final Decision Documentation
- Reflection period: 24-48 hours mandatory waiting
- Witness requirement: independent observer present
- Documentation standards: legal-grade record keeping
- Decision capacity: formal assessment completed
- Voluntary consent: coercion absence verified
- Understanding confirmation: written acknowledgment
📌 Remember: CONSENT Process - Comprehension, Options, Nature, Success rates, Expectations, Need assessment, Time for reflection
Consent Documentation Standards
| Procedure Category | Information Depth | Reflection Period | Witness Requirement | Documentation Level |
|---|---|---|---|---|
| Contraception | Basic risks/benefits | Immediate decision | Optional | Standard form |
| Sterilization | Comprehensive counseling | 30 days mandatory | Required | Detailed documentation |
| ART Procedures | Extensive protocols | 1 week recommended | Preferred | Complete records |
| Prenatal Testing | Specific test details | 24-48 hours | Optional | Targeted consent |
| Fetal Intervention | Exhaustive discussion | 1 week minimum | Mandatory | Comprehensive documentation |
Special Consent Considerations
Vulnerable populations require enhanced protection with additional safeguards ensuring genuine autonomy:
-
Adolescent Consent Framework
- Mature minor assessment: decision-making capacity evaluation
- Parental involvement: state-specific requirements
- Confidentiality protection: absolute privacy when appropriate
- Age thresholds: 16+ years for contraception
- Emergency situations: immediate care authorization
- Abuse suspicion: mandatory reporting protocols
-
Mental Health Considerations
- Capacity assessment: formal psychiatric evaluation
- Surrogate decision-making: legal guardian involvement
- Medication effects: cognitive impact evaluation
- Depression screening: standardized assessment tools
- Anxiety management: pre-procedure intervention
- Support systems: family involvement encouragement
💡 Master This: Consent validity requires four elements: information disclosure (complete), comprehension (verified), voluntariness (confirmed), and competence (assessed)
Emergency Consent Protocols
Life-threatening situations require modified consent procedures balancing immediate care needs with patient autonomy:
- Implied Consent Scenarios
- Unconscious patient: presumed consent for life-saving care
- Emergency surgery: immediate intervention authorization
- Maternal collapse: fetal consideration in decision-making
- Time constraints: <30 minutes for intervention
- Family consultation: when feasible without delay
- Documentation: retrospective detailed recording
Informed consent creates the trust foundation for all reproductive care. Connect these consent principles through specific clinical scenarios to understand practical application challenges.
🤝 The Informed Consent Architecture
🔬 The Clinical Ethics Laboratory
Clinical application transforms abstract ethical principles into practical decision-making tools through systematic scenario analysis and evidence-based resolution frameworks.
Scenario-Based Ethical Navigation
Pattern recognition for common reproductive ethics dilemmas with systematic resolution approaches:
-
Contraception Conflicts
- Adolescent confidentiality vs. parental rights
- Religious objections vs. medical recommendations
- Partner disagreement vs. individual autonomy
- Age-specific protocols: state law compliance
- Cultural sensitivity: respectful dialogue maintenance
- Safety prioritization: medical needs first
-
ART Dilemma Categories
- Multiple embryo transfer requests vs. safety guidelines
- Genetic testing demands vs. discrimination concerns
- Surrogacy arrangements vs. exploitation prevention
- Success optimization: single embryo transfer preference
- Genetic counseling: comprehensive risk discussion
- Legal compliance: contract review mandatory
📌 Remember: ETHICS Resolution - Evaluate stakeholders, Time constraints, Harm assessment, Informed consent, Cultural factors, Solution implementation
Maternal-Fetal Conflict Resolution
| Conflict Type | Maternal Rights | Fetal Interests | Resolution Framework | Success Rate |
|---|---|---|---|---|
| Treatment Refusal | Absolute autonomy | Potential benefit | Counseling + respect | 78% agreement |
| Lifestyle Choices | Personal freedom | Health optimization | Education + support | 65% modification |
| Delivery Decisions | Informed choice | Safety considerations | Risk discussion | 89% consensus |
| Fetal Surgery | Consent required | Intervention benefit | Multidisciplinary review | 92% appropriate care |
| End-of-Life Care | Decision authority | Comfort measures | Palliative focus | 96% family satisfaction |
Prenatal Testing Ethics Framework
Genetic testing decisions require careful balance between information access and discrimination prevention:
-
Testing Indication Hierarchy
- Medical necessity: clear clinical benefit
- Family history: documented genetic risk
- Patient request: informed decision-making
- Risk thresholds: >1:250 for invasive testing
- Accuracy rates: >99% for screening tests
- Counseling requirements: pre and post test discussion
-
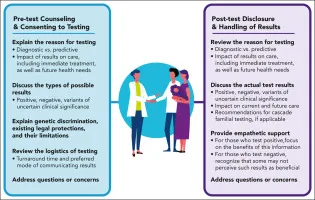
Result Disclosure Protocols
- Positive results: immediate genetic counseling
- Uncertain findings: expert interpretation required
- Negative results: residual risk explanation
- Turnaround time: <14 days for results
- Support services: comprehensive resource provision
- Follow-up care: coordinated management plan
💡 Master This: Genetic testing ethics requires non-directive counseling where patient values guide decisions, not provider preferences or societal pressures
Resource Allocation Ethics
Limited resources demand fair distribution based on objective criteria rather than subjective preferences:
-
ART Access Prioritization
- Medical factors: infertility duration and severity
- Success probability: age-adjusted likelihood
- Previous attempts: treatment history consideration
- Waiting list management: transparent criteria
- Geographic equity: rural access provision
- Economic barriers: insurance coverage advocacy
-
Emergency Care Triage
- Maternal condition: life-threatening status priority
- Fetal viability: gestational age consideration
- Resource availability: capacity assessment
- Response time: <15 minutes for emergencies
- Specialist availability: 24/7 coverage
- Transfer protocols: higher level care access
Clinical ethics application creates systematic approaches to complex dilemmas. Connect these practical frameworks through advanced integration concepts to understand multi-system ethical considerations.
🔬 The Clinical Ethics Laboratory
🌐 The Ethical Integration Nexus
Multi-system integration reveals how individual ethical decisions connect to broader healthcare systems, social justice, and global reproductive health initiatives.
Cross-Cultural Ethical Navigation
Cultural competency in reproductive ethics demands deep understanding of diverse value systems while maintaining universal human rights principles:
-
Religious Consideration Matrix
- Hindu perspectives: dharma-based decision-making
- Islamic guidelines: Sharia-compliant reproductive choices
- Christian viewpoints: sanctity of life emphasis
- Contraception acceptance: 85% Hindu, 78% Muslim, 92% Christian
- ART utilization: 89% Hindu, 67% Muslim, 88% Christian
- Prenatal testing: 76% Hindu, 54% Muslim, 81% Christian
-
Socioeconomic Integration
- Rural access: mobile clinic programs
- Urban disparities: sliding scale fee structures
- Tribal populations: culturally adapted service delivery
- Geographic coverage: 80% rural penetration target
- Language services: 15+ regional languages
- Traditional healer: collaborative care models
📌 Remember: CULTURE Integration - Customs respect, Universal rights, Language adaptation, Tradition acknowledgment, Understanding promotion, Responsive care, Equity assurance
Technology Ethics Evolution
| Technology | Ethical Challenges | Regulatory Status | Implementation Rate | Future Projections |
|---|---|---|---|---|
| Gene Editing | Germline modification concerns | Research phase only | <1% clinical use | 5-10 years for approval |
| AI Diagnostics | Algorithm bias prevention | Pilot programs | 15% adoption | 3-5 years widespread |
| Telemedicine | Privacy protection needs | Approved with guidelines | 67% utilization | 90% by 2025 |
| 3D Bioprinting | Organ creation ethics | Experimental stage | <0.1% availability | 10-15 years clinical |
| Blockchain Records | Data security enhancement | Development phase | 8% implementation | 2-3 years standard |
Global Health Ethics Integration
International collaboration in reproductive health creates shared responsibility for global equity and sustainable development:
-
Sustainable Development Goals Alignment
- Goal 3: Good health and well-being
- Goal 5: Gender equality achievement
- Goal 10: Reduced inequalities promotion
- Maternal mortality: <70 per 100,000 global target
- Contraceptive access: 75% global coverage goal
- Skilled birth attendance: 90% delivery target
-
Research Ethics Globalization
- International standards: ICH-GCP compliance
- Vulnerable population protection: enhanced safeguards
- Benefit sharing: equitable distribution
- Multi-country studies: standardized protocols
- Data sharing: secure international platforms
- Capacity building: local expertise development
💡 Master This: Global reproductive ethics requires local adaptation of universal principles - one size fits none approach demands culturally responsive implementation
Future Ethics Challenges
Anticipatory ethics preparation for emerging reproductive technologies and evolving social norms:
-
Artificial Womb Technology
- Maternal-fetal relationship: redefinition required
- Parental rights: legal framework development
- Resource allocation: access equity planning
- Development timeline: 15-20 years estimated
- Regulatory preparation: 5-year framework development
- Ethical guidelines: immediate discussion needed
-
Genetic Enhancement Debates
- Therapeutic vs. enhancement: boundary definition
- Social inequality: genetic divide prevention
- Consent across generations: future impact consideration
- Research limitations: therapeutic focus only
- International cooperation: global standards needed
- Public engagement: democratic decision-making
Advanced ethical integration creates comprehensive frameworks for complex reproductive decisions. Connect these integration concepts through practical mastery tools to develop clinical expertise in ethical decision-making.
🌐 The Ethical Integration Nexus
🎯 The Reproductive Ethics Mastery Toolkit
The ETHICS-PLUS Rapid Assessment Framework
Systematic approach for immediate ethical evaluation in any reproductive scenario:
📌 Remember: ETHICS-PLUS - Evaluate stakeholders, Time sensitivity, Harm assessment, Informed consent, Cultural factors, Solution options, Principles application, Legal compliance, Understanding verification, Support systems
Essential Numbers Arsenal
| Category | Critical Thresholds | Legal Requirements | Clinical Significance |
|---|---|---|---|
| MTP Limits | 20 weeks (1 doctor), 24 weeks (2 doctors) | Mandatory compliance | Zero legal flexibility |
| Sterilization | 30-day cooling period | Documented consent | Regret rate <5% |
| ART Success | >35% live birth rate | Annual reporting | Quality indicator |
| PCPNDT | Zero sex determination | Immediate reporting | License suspension risk |
| Consent | 24-48 hours reflection | Witness documentation | Legal protection |
Quick Decision Trees
Cultural Competency Quick Reference
- Hindu Considerations: Dharma (righteous duty) guides decisions, family involvement expected, karma beliefs affect choices
- Islamic Guidelines: Halal procedures only, spousal consent important, preservation of life priority
- Christian Perspectives: Sanctity of life emphasis, natural law considerations, community support valued
- Tribal Customs: Elder consultation required, traditional healing integration, community decision-making
💡 Master This: Cultural competency = Universal principles + Local adaptation + Respectful dialogue + Flexible implementation
Emergency Ethics Protocols
Life-threatening situations require immediate action with ethical safeguards:
- Maternal Collapse: Fetal considerations secondary to maternal life
- Fetal Distress: Informed maternal consent when time permits
- Hemorrhage: Blood product administration per religious preferences
- Cardiac Arrest: Full resuscitation unless documented refusal
Master reproductive ethics through systematic application of these evidence-based frameworks, ensuring optimal outcomes for all stakeholders while maintaining legal compliance and cultural sensitivity.
🎯 The Reproductive Ethics Mastery Toolkit
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more
Have doubts about this lesson?
Ask Rezzy, your AI Study Mate, to explain anything you didn't understand
Everything you need for NEET-PG prep
Get full Oncourse access with lessons, practice questions, flashcards and AI study tools.
Scan to download app




















