Antenatal Screening - Bump's First Roadmap
Systematic tests during pregnancy to detect risks for mother and fetus, enabling timely interventions.
- Initial & Universal:
- Blood group, Rh type, CBC, Hb electrophoresis
- Infections: HIV, HBsAg, VDRL, Urine R/M & C/S
- Rubella IgG, TSH
- Aneuploidy Screening:
- Combined Test (First Trimester Screen): NT scan + PAPP-A + β-hCG
- Quadruple Test (Second Trimester)
- NIPT (cfDNA)
- Key Ultrasounds:
- Early scan (dating)
- NT scan (11-13+6 wks)
- Anomaly scan (TIFFA: 18-22 wks)
⭐ In India, a single-step 75g OGTT is recommended for GDM screening at 24-28 weeks, or at first visit for high-risk women (as per DIPSI guidelines).
First Trimester Screening - Early Bird Detectives
- Timing: 11 - 13+6 weeks gestation.
- Combined Test Components:
- Maternal Serum (Dual Test):
- Free β-hCG: ↑ Trisomy 21; ↓ Trisomy 18/13.
- PAPP-A (Pregnancy-Associated Plasma Protein-A): ↓ Trisomy 21, 18, 13.
- Ultrasound (USG) Markers:
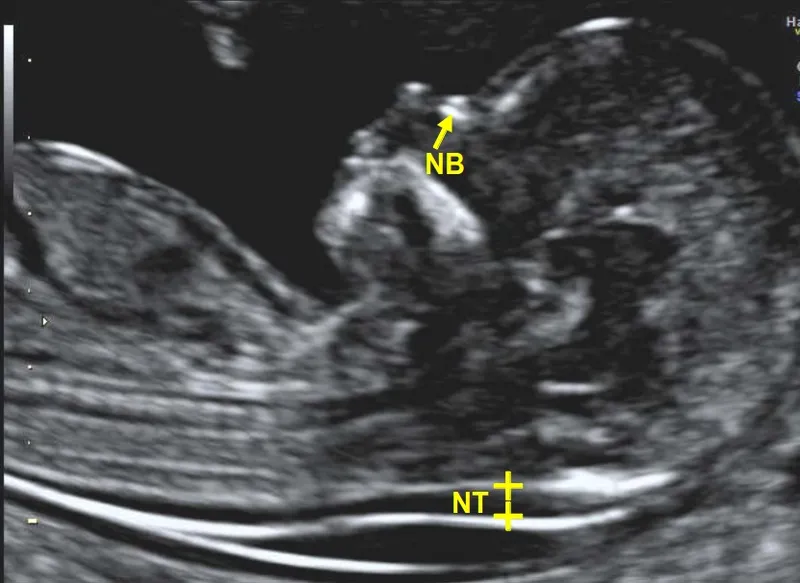
- Nuchal Translucency (NT): ↑ suggests aneuploidy/cardiac defects. (Normal < 3.5 mm)
- Nasal Bone (NB): Absent ↑ Trisomy 21 risk.
- Maternal Serum (Dual Test):
- Aims:
- Screen for Trisomies 21, 18, 13.
- Accurate dating (Crown-Rump Length - CRL).
- Detect multiple pregnancies, major anomalies.
- Combined First Trimester Screening (CFTS):
- Combines maternal age, NT, Free β-hCG, PAPP-A.
- Trisomy 21 Detection Rate: ~90%; False Positive Rate: 5%.
⭐ PAPP-A levels are significantly decreased in Trisomies 21, 18, and 13, making it a crucial early marker.
Second Trimester Screening - Mid-Journey Checkpoint
- Optimal Timing:
- Anomaly Scan (TIFFA/Level II): 18-20 weeks (acceptable up to 22 weeks).
- Quadruple Test: 15-20 weeks (acceptable up to 22 weeks).
- Targeted Imaging for Fetal Anomalies (TIFFA) / Level II Scan:
- Comprehensive fetal structural survey (e.g., brain, face, spine, heart, abdomen, limbs).
- Assesses fetal biometry, placental localization, amniotic fluid volume (AFV).
- Cervical length assessment.

- Quadruple Test (Serum Markers):
- Components: Maternal serum AFP (Alpha-fetoprotein), hCG (Human Chorionic Gonadotropin), uE3 (Unconjugated Estriol), Inhibin A.
- Screens for: Trisomy 21 (Down syndrome), Trisomy 18 (Edwards syndrome), Open Neural Tube Defects (ONTDs).
- Trisomy 21: ↓AFP, ↓uE3, ↑hCG, ↑Inhibin A. (📌 Remember: HIgh hCG & Inhibin A)
- Trisomy 18: ↓AFP, ↓uE3, ↓hCG (all significantly low).
- Open NTDs: ↑↑AFP (significantly elevated, isolated finding).
⭐ Increased Nuchal Fold thickness (>6mm) on ultrasound is the most specific second-trimester soft marker for Down syndrome (Trisomy 21).
Late Pregnancy Screens - Homestretch Safeguards
- Gestational Diabetes (GDM):
- Screen: 24-28 weeks.
- India (DIPSI): 75g OGTT, 2-hr plasma glucose $\ge$ 140 mg/dL.
- IADPSG: 75g OGTT; Fasting $\ge$ 92, 1-hr $\ge$ 180, 2-hr $\ge$ 153 mg/dL (any one).
- Group B Strep (GBS):
- Screen: 36+0 to 37+6 weeks (rectovaginal swab).
- Purpose: Intrapartum antibiotic prophylaxis (IAP) if positive.
- Anemia: Repeat Hb/Hct at 28-32 weeks.
- RhD Negative Mothers: Antibody screen at 28 weeks (before Anti-D Ig).
- Fetal Surveillance: As indicated (e.g., USG for growth, NST).
⭐ Universal GBS screening (rectovaginal swab) at 36+0 to 37+6 weeks significantly reduces early-onset neonatal GBS sepsis.
High‑Yield Points - ⚡ Biggest Takeaways
- Combined test (NT, β-hCG, PAPP-A) is optimal 1st-trimester aneuploidy screening.
- Quadruple test (AFP, β-hCG, uE3, Inhibin A) is key for 2nd-trimester screening (15-20 wks).
- NIPT (cell-free DNA) shows highest detection for trisomies 21, 18, 13.
- 75g OGTT is standard for GDM screening; DIPSI criteria (single step) widely used in India.
- Urine culture at first visit is crucial for detecting asymptomatic bacteriuria (ASB).
- Hb electrophoresis is vital for hemoglobinopathy screening (thalassemia, sickle cell).
- Universal screening for HIV, HBsAg, VDRL at the booking visit is mandatory.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

