Routine Antenatal Assessments - First Steps First
- History Taking:
- LMP, EDD calculation (Naegele's rule).
- Obstetric history (GTPAL), medical, surgical, family history.
- Clinical Examination:
- Vitals (BP, Wt, Ht), general physical (pallor, edema), systemic exam.
- Obstetric: P/A (fundal height if >12 wks), P/V (if indicated).
- Baseline Investigations:
- Hemoglobin (Hb), Blood group & Rh typing.
- Urine: Routine/Microscopy, Culture.
- Serology: HIV, HBsAg, VDRL/RPR.
- Random Blood Sugar (RBS) or Glucose Challenge Test (GCT).
- Dating Ultrasound (USS):
- Ideally 6-9 weeks: confirms viability, accurate dating (CRL), number of fetuses.
- Nuchal Translucency (NT) scan option at 11-13.6 weeks.
- Counseling:
- Nutrition, weight gain, folic acid supplementation.
- Warning signs, antenatal visit schedule, tetanus toxoid immunization.
⭐ Folic acid (400 mcg/day; 5 mg for high-risk) initiated pre-conceptionally or ASAP to prevent Neural Tube Defects (NTDs).

Routine Antenatal Assessments - Bump Watch Continues
- Goal: Healthy mother & baby.
- Initial Visit (Booking ~8-12 wks):
- Hx (LMP, EDD ($LMP + 9M + 7D$)), Exam (Wt, BP, FH).
- Labs: Hb, BG-Rh, HIV, HBsAg, VDRL, RBS, Urine.
- Dating USG (6-9 wks CRL).
- Follow-up Visit Frequency:
- Key Gestational Assessments:
- Each visit: Wt, BP, FH, FHS, FM, Urine alb/sugar.
- 11-14 wks: NT scan, Dual marker.
- 18-20 wks: Anomaly Scan (TIFFA).
⭐ TIFFA (18-20 wks) detects major fetal structural anomalies.
- 24-28 wks: GDM screen, Hb. Rh(-): ICT.
- 32-36 wks: Growth scan (opt). GBS screen (35-37 wks).

Routine Antenatal Assessments - Test Fest Time
- Booking Visit (<12 wks):
- Hx, Exam (BP, Wt), EDD (Naegele: LMP - 3mo + 7d + 1yr).
- Labs: Hb, Blood grp/Rh, HIV, HBsAg, VDRL/RPR, RBS, Urine R/M, C/S.
- Visit Freq: 📌 4-2-1 Rule: Q4W till 28 wks → Q2W 28-36 wks → Q1W from 36 wks.
- Routine Checks (Each Visit): BP, Wt, Fundal Ht, FHS, Urine Alb/Sugar.
⭐ Anomaly scan (TIFFA) is ideally performed between 18-20 weeks gestation for detecting major structural fetal abnormalities.
Routine Antenatal Assessments - Baby's Report Card
- Goal: Monitor maternal & fetal health, early detection of complications.
- Initial Visit (Booking):
- History: LMP, EDD (📌 Naegele's: $LMP + 9 \text{ months} + 7 \text{ days}$), Obstetric Hx.
- Exam: General, Systemic, Obstetric.
- Labs: Hb, Blood group/Rh, VDRL, HBsAg, HIV, Urine R/M, RBS.
- Follow-up Visits:
- Schedule: Q4W up to 28w → Q2W 28-36w → Q1W >36w.
- Checks: Wt, BP, SFH, FHS, Fetal Movements, Urine Alb/Sugar.
- Key Investigations Timeline:
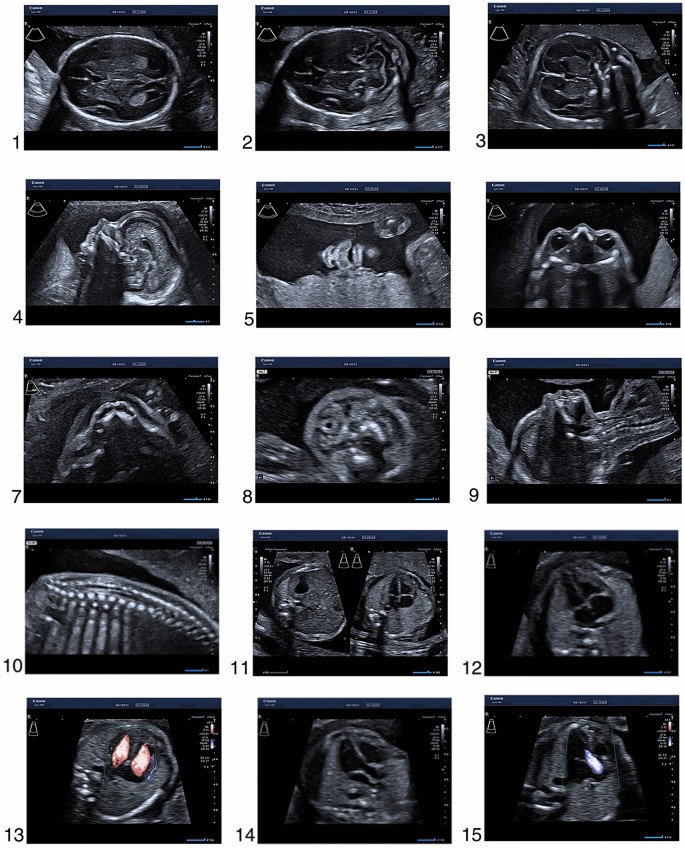
> ⭐ The anomaly scan (Level II USG) around **18-20 weeks** is crucial for detecting major structural fetal abnormalities.
High‑Yield Points - ⚡ Biggest Takeaways
- First antenatal visit: ideally first trimester for baseline investigations & risk stratification.
- Regular BP checks: vital for early detection of hypertensive disorders.
- Fundal height: correlates with gestational age, especially post 20 weeks.
- Anomaly scan (TIFFA): crucial at 18-20 weeks for fetal structural defects.
- Iron & Folic Acid (IFA): routine supplementation prevents anemia & neural tube defects.
- Tetanus Toxoid (TT): two doses prevent maternal & neonatal tetanus.
- GDM Screening: OGTT mandatory for detecting Gestational Diabetes.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

