Physiological Pituitary Changes in Pregnancy - Glandular Glow-Up
- Pituitary gland enlarges significantly (up to 135% or 2x size).
- Mainly due to estrogen-driven lactotroph hyperplasia.
- ↑ Prolactin (PRL): Rises progressively for lactation.
- ↓ FSH & LH: Suppressed by placental steroids, preventing ovulation.
- ↑ ACTH & MSH: Leads to ↑ cortisol & skin pigmentation.
- TSH: Transient ↓ 1st trimester (hCG effect), then normal.
⭐ Pituitary gland nearly doubles in size due to estrogen-driven lactotroph hyperplasia, increasing vulnerability to Sheehan's syndrome post-hemorrhage.
Prolactinoma and Pregnancy - Milky Matters
Most common pituitary tumor; secretes prolactin (PRL). Pregnancy (↑estrogen) may enlarge tumor by stimulating lactotrophs.
- Microadenomas (<10 mm):
- Low risk of symptomatic enlargement.
- Stop dopamine agonists (DA) (e.g., Bromocriptine) upon pregnancy confirmation.
- Monitor symptoms (headache, visual changes); restart DA if tumor growth/symptoms.
- Macroadenomas (>10 mm):
- Higher risk of symptomatic enlargement.
- Continue DA (Bromocriptine preferred for safety) throughout pregnancy.
- Regular visual field assessment (e.g., quarterly).
- MRI (no gadolinium) for new/worsening neuro-ophth symptoms.
- Breastfeeding: Safe. Postpartum DA compatible.
⭐ Crucial: Visual field monitoring for macroadenomas in pregnancy (risk of symptomatic enlargement).

Sheehan's Syndrome - Postpartum Pituitary Peril
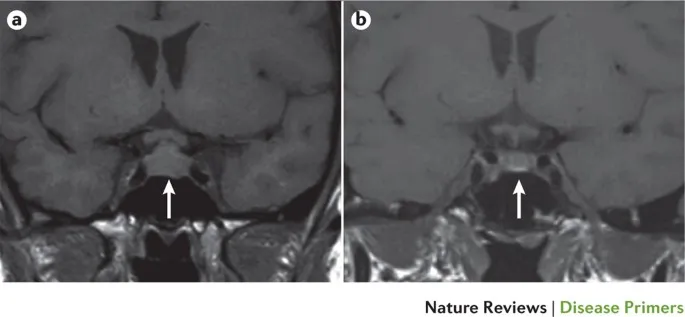
- Postpartum hypopituitarism due to ischemic necrosis of the anterior pituitary gland.
- Pathophysiology: Severe postpartum hemorrhage (PPH) → profound hypotension/shock → vasospasm of hypophyseal arteries.
- Physiologically enlarged pituitary during pregnancy is more susceptible to ischemia.
- Clinical Features:
- Early: Failure of lactation (↓prolactin), amenorrhea/oligomenorrhea (↓LH/FSH), persistent fatigue, weakness.
- Late: Symptoms of hypothyroidism (↓TSH - e.g., cold intolerance, dry skin), adrenal insufficiency (↓ACTH - e.g., postural hypotension, hypoglycemia), pallor, loss of axillary/pubic hair.
- Diagnosis: Low basal levels of pituitary & target organ hormones (e.g., TSH, free T4, ACTH, cortisol, FSH, LH, estradiol). Provocative hormonal tests. MRI may show an empty sella turcica in late stages.
- Management: Lifelong hormone replacement therapy (glucocorticoids first, then thyroxine, sex steroids).
⭐ Failure of lactation (agalactia) is often the earliest and most common presenting symptom of Sheehan's Syndrome.
Other Pituitary Disorders in Pregnancy - Rare But Real
- Cushing's Disease:
- Rare; ↑maternal/fetal risks (preeclampsia, GDM, IUGR).
- Diagnosis: 24-hr UFC, late-night salivary cortisol.
- Management: Metyrapone (preferred); surgery if severe.
- Acromegaly:
- Very rare; GH can ↓fertility.
- Tumor growth possible. Visual field monitoring crucial.
- Management: Bromocriptine if symptomatic. Discontinue somatostatin analogs.
- Diabetes Insipidus (DI):
- Central: Vasopressin deficiency.
- Gestational: Placental vasopressinase ↑ADH degradation; typically 3rd trimester.
- Symptoms: Polyuria, polydipsia.
- Management: Desmopressin (DDAVP).
⭐ Gestational DI is caused by placental vasopressinase degrading ADH and typically resolves postpartum.
- Lymphocytic Hypophysitis:
- Autoimmune inflammation; late pregnancy/postpartum.
- Symptoms: Headache, visual defects, hypopituitarism (ACTH/TSH deficiency common).
- Management: Corticosteroids, hormone replacement.
High‑Yield Points - ⚡ Biggest Takeaways
- Physiological pituitary enlargement (due to lactotroph hyperplasia) is normal during pregnancy.
- Sheehan's syndrome: postpartum pituitary necrosis (often after PPH), causing failure of lactation and panhypopituitarism.
- Prolactinomas: most common; may enlarge. Use bromocriptine/cabergoline if visual fields compromised.
- Lymphocytic hypophysitis: autoimmune; late pregnancy/postpartum. Presents with headache, visual changes, hypopituitarism.
- Gestational Diabetes Insipidus: due to placental vasopressinase degrading ADH; responds to desmopressin (DDAVP).
- Pituitary apoplexy: rare emergency; sudden headache, visual loss, hypopituitarism. Urgent steroids treatment is crucial.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

