Basics & Clinical Clues - The Red Alert
- Definition: Injury to arteries or veins, potentially limb/life-threatening.
- Mechanisms:
- Penetrating: Gunshot, stab.
- Blunt: Fractures, dislocations, crush.
- Initial Steps: ABCDEs; control hemorrhage (direct pressure).
- Hard Signs (⚠️ RED ALERT - Direct to OT):
- Pulsatile bleeding
- Expanding hematoma
- Palpable thrill / Audible bruit
- Absent distal pulses
- Distal ischemia (6 P's)
- Soft Signs (Investigate: ABI, CT Angio):
- History of arterial bleeding
- Injury proximity to major vessel
- Small, stable hematoma
- Associated nerve injury
- Diminished pulses
- 📌 6 P's of Acute Limb Ischemia: Pain, Pallor, Pulselessness, Paresthesia, Paralysis, Poikilothermia.

⭐ Hard signs of vascular injury mandate immediate surgical exploration, often bypassing further imaging.
Diagnostic Workup - Spotting the Leak
- Initial step: Differentiate hard vs. soft signs of vascular injury.
- Hard signs: Active hemorrhage, expanding hematoma, thrill/bruit, absent distal pulses, ischemia (📌 6 P's) → Immediate OR.
- Soft signs: Hx of significant bleed, diminished pulses, proximity injury, nerve deficit → Further workup.
- Investigations for Soft Signs/Proximity:
- Ankle-Brachial Index (ABI): Bedside. ABI < 0.9 indicates likely arterial injury.
- Duplex Ultrasonography (DUS): Non-invasive, operator-dependent. Good for neck, extremity.
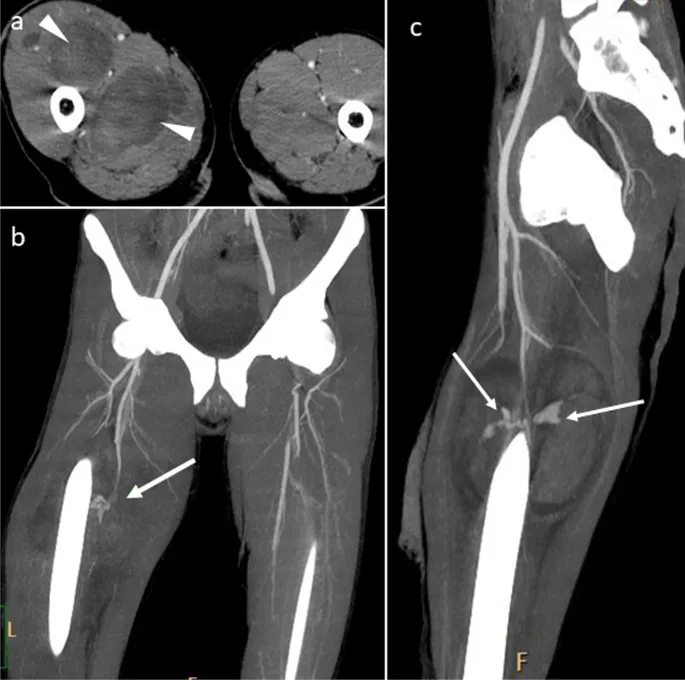
- CT Angiography (CTA): Modality of choice for stable patients. High sensitivity & specificity.
⭐ CTA is the gold standard for diagnosing hemodynamically stable patients with suspected peripheral vascular trauma, offering detailed anatomical information.
- Conventional Angiography: Invasive. Gold standard if therapeutic intervention (e.g., embolization, stenting) is anticipated.
Treatment Strategies - Plugging the Holes
- Initial Control & Resuscitation:
- Direct pressure; tourniquet (last resort, document application time).
- ATLS: Permissive hypotension (target SBP 80-90 mmHg) until definitive hemorrhage control.
- Balanced transfusion: 1:1:1 (PRBC:FFP:Platelets).
- Surgical Principles & Techniques:
- Achieve proximal & distal vascular control. Use vessel loops, clamps, or Fogarty catheter for temporary occlusion.
- Repair Options:
- Lateral arteriorrhaphy (simple lacerations).
- End-to-end anastomosis (clean transections).
- Interposition graft: Autologous vein (e.g., saphenous) ideal, especially in contamination. Prosthetic if vein unavailable/large vessel.
- Ligation: For non-critical arteries if limb perfusion adequate.
- Damage Control Surgery (DCS): Temporary Intravascular Shunt (TIVS) to restore flow quickly in unstable patients or complex injuries.
- Adjunctive Measures:
- Fasciotomy: Mandatory for established compartment syndrome or prophylactically if ischemia > 4-6 hours.
- Endovascular Management (selected cases): Covered stents for pseudoaneurysms/fistulas; embolization for non-critical vessel bleeding.
⭐ Prophylactic fasciotomy is indicated if revascularization occurs after 4-6 hours of warm ischemia time to prevent reperfusion injury and compartment syndrome.

Complications & Regional Injuries - Aftermath & Hotspots
- Immediate/Early Complications:
- Persistent Hemorrhage, Re-thrombosis
- Compartment Syndrome (⚠️ intracompartmental pressure >30 mmHg or ΔP < 30 mmHg; requires fasciotomy)
- Infection, Missed associated injuries
- Late Sequelae:
- Pseudoaneurysm, Arteriovenous Fistula (AVF)
- Chronic Limb Ischemia, Claudication
- Venous Thromboembolism (VTE), Neuropathy, Chronic Pain
- Amputation
- Key Regional Considerations:
- Neck (Zones I,II,III): Vertebral artery injury (posterior stroke risk).
- Thorax: Great vessel injury (e.g., Aorta, SVC, PA); high mortality.
- Abdomen: Retroperitoneal hematoma; Aorto-iliac/caval injuries.
- Extremities:
- Popliteal artery (⚠️ highest amputation risk if repair delayed > 6-8 hrs).
- Brachial artery (risk of Volkmann's ischemic contracture).
⭐ Hard signs of vascular injury (Pulsatile bleeding, Palpable thrill, Audible bruit, Expanding hematoma, Signs of distal ischemia) mandate surgical exploration.
High‑Yield Points - ⚡ Biggest Takeaways
- Hard signs (pulsatile bleed, expanding hematoma, absent pulse, thrill/bruit) mandate surgical exploration.
- Soft signs (history of bleed, diminished pulse, nerve deficit) warrant CTA or Doppler.
- ABI < 0.9 indicates arterial injury in extremity trauma; investigate.
- Compartment syndrome (pain out of proportion, 6 Ps) requires urgent fasciotomy.
- Temporary shunts are limb-saving in damage control or delayed repair.
- Proximal and distal control is key before vascular repair.
- Blunt aortic injury commonly occurs at the aortic isthmus.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

