GIB: Overview & Initial Rx - Spotting the Source
- Types: UGIB (proximal to Lig. of Treitz), LGIB (distal). Overt (visible) vs. Occult (FOBT+).
- Initial Rx (ABCDE):
- Assess hemodynamics (Shock Index: $HR/SBP$ > 0.9 indicates shock).
- Secure airway; 2 large-bore IV cannulas.
- Fluid resuscitation: Crystalloids. Blood if Hb < 7 g/dL (or < 9 g/dL in CAD).
- Correct coagulopathy (FFP, Vit K).
- Spotting Source:
- History (NSAIDs, EtOH), exam.
- NG lavage (UGIB), proctoscopy (fresh PR bleed).
- Endoscopy: EGD for UGIB, Colonoscopy for LGIB.

⭐ Most common cause of significant UGIB is peptic ulcer disease.
UGIB: Causes & Management - Above Treitz Terrors
Bleeding proximal to Ligament of Treitz.
Causes:
- Non-Variceal (80%): PUD (H. pylori, NSAIDs), Mallory-Weiss, Erosions, Dieulafoy's.
- Variceal (20%): Esophageal/Gastric varices (portal HTN). 📌 Causes: Mallory, Esophagitis, Dieulafoy, Inflammation (gastritis), Cancer, Ulcer, Varices. (MEDIC UV)
Management:
- Resuscitation: ABCs, IV fluids, blood (Hb < 7 g/dL). PPI (non-variceal), Octreotide + Abx (variceal).
- Risk Stratify: Glasgow-Blatchford (GBS > 0 high risk), Rockall.
- Endoscopy (OGD): Within 24h. Diagnose & treat.
- Non-variceal: Forrest class. Clips, thermal, adrenaline.
- Variceal: Banding, sclerotherapy.
- Post-Endo: PPI, H. pylori eradication. beta-blockers (varices). TIPS if refractory.
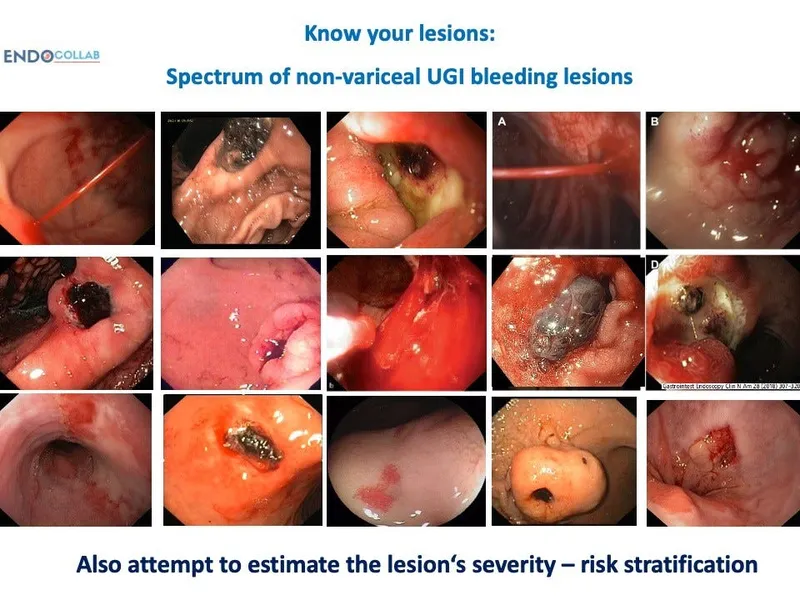
⭐ Forrest Ia (spurting arterial bleed) has ~55% rebleed risk without endoscopic therapy.
LGIB: Causes & Management - Below Treitz Troubles
- Bleeding distal to Ligament of Treitz.
- Common Causes:
- Diverticulosis: Most common cause of massive LGIB; typically painless, arterial bleed.
- Angiodysplasia: Vascular ectasias, common in elderly, right colon; often occult or recurrent.
- Colitis: IBD, ischemic, infectious; usually associated with pain, bloody diarrhea.
- Neoplasms/Polyps: Can cause chronic occult or acute frank bleeding.
- Anorectal: Hemorrhoids, fissures; bright red blood on toilet paper (BRBPR).
- Diagnosis:
- Initial: Exclude UGIB if suspected.
- Stable patients: Colonoscopy (diagnostic & therapeutic).
- Active/Massive bleed: CTA (preferred if bleed >0.3-0.5 mL/min) or Tagged RBC scan (detects bleed >0.1-0.5 mL/min).
- Management:
- Resuscitation: ABCs, 2 large-bore IV lines, fluids, blood products.
- Therapeutic Colonoscopy: Clips, thermal coagulation, epinephrine injection.
- Angiographic embolization: For active bleeding identified on CTA/RBC scan.
- Surgery: Segmental resection or subtotal colectomy for refractory/unlocalized severe bleeding.
⭐ Diverticulosis is the most common cause of major LGIB. Bleeding stops spontaneously in ~80% of cases, but recurrence is common (20-40%).
OGIB & Small Bowel - Elusive Escapes
- Obscure GI Bleed (OGIB): Persistent/recurrent bleeding despite negative UGI endoscopy & colonoscopy.
- Overt: Melena, hematochezia.
- Occult: FOBT positive, iron deficiency anemia.
- Small bowel is the source in ~75% of OGIB cases.
- Key Investigations:
- Video Capsule Endoscopy (VCE): First-line for suspected small bowel source.
⭐ VCE boasts the highest diagnostic yield for detecting small bowel bleeding causes.
- Device-Assisted Enteroscopy (DAE): For diagnosis & intervention.
- CT/MR Enterography; Angiography for active bleed.
- Video Capsule Endoscopy (VCE): First-line for suspected small bowel source.
- Common Causes: Angiodysplasia (most common), tumors, NSAID enteropathy, Crohn's.
High‑Yield Points - ⚡ Biggest Takeaways
- UGIB is more common; LGIB often from diverticulosis or angiodysplasia.
- Peptic ulcer disease is the leading cause of UGIB.
- Initial management for severe bleeding: Resuscitation (fluids, blood products).
- Early endoscopy (within 24h) is key for UGIB diagnosis & therapy.
- Rockall and Glasgow-Blatchford scores assess risk in UGIB.
- Variceal bleeds: manage with octreotide, antibiotics, & EVL.
- Massive LGIB may need angiography/embolization or surgery.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

