Chemical Mediators: Overview & Vasoactive Amines - Rapid Responders
- Overview of Mediators:
- Cell-derived: Preformed in granules (e.g., histamine) or newly synthesized (e.g., prostaglandins).
- Plasma-derived: Synthesized mainly in liver (e.g., complement, kinins); circulate as inactive precursors.
- Actions: Bind specific receptors; short-lived; tightly regulated; can stimulate other mediators.
- Vasoactive Amines (Rapid Responders):
- Histamine:
- Sources: Mast cells (primary), basophils, platelets.
- Release triggers: Physical injury, IgE cross-linking, C3a/C5a (anaphylatoxins), neuropeptides (Substance P), cytokines (IL-1, IL-8).
- Actions: Arteriolar dilation, ↑ venular permeability (via H1 receptors, endothelial contraction), bronchial constriction.
⭐ Histamine is pre-formed in mast cell granules.
- Serotonin (5-Hydroxytryptamine, 5-HT):
- Sources: Platelets, enterochromaffin cells.
- Actions: Similar to histamine (↑ vascular permeability); released during platelet aggregation. Also involved in vasoconstriction during clotting.
- Histamine:
Chemical Mediators: Arachidonic Acid Metabolites - Eicosanoid Orchestra
- Derived from membrane phospholipids via Phospholipase $A_2$ (inhibited by steroids).
- Cyclooxygenase (COX) Pathway:
- Yields Prostaglandins (PGs) & Thromboxane $A_2$ ($TXA_2$).
- PGs ($PGE_2, PGD_2, PGI_2$): Vasodilation, pain, fever. $PGI_2$ also inhibits platelet aggregation. $PGF_{2\alpha}$ causes vasoconstriction.
- $TXA_2$: Vasoconstriction, promotes platelet aggregation.
- 📌 Mnemonic: Prostaglandins = Pain, Pyrexia (fever); Thromboxane = Thrombosis.
- Lipooxygenase (LOX) Pathway:
- Yields Leukotrienes (LTs) & Lipoxins.
- $LTB_4$: Potent chemotactic agent.
- $LTC_4, LTD_4, LTE_4$ (SRS-A): Bronchoconstriction, ↑vascular permeability.
- Lipoxins ($LXA_4, LXB_4$): Anti-inflammatory, inhibit neutrophil chemotaxis & adhesion.
- Pharmacological Modulation:
- NSAIDs (e.g., Aspirin, Ibuprofen): Inhibit COX.
- Zileuton: Inhibits LOX.
- Montelukast: LT receptor antagonist.
⭐ Aspirin irreversibly inhibits cyclooxygenase (COX), affecting platelet function for their entire lifespan.
Chemical Mediators: Cytokines & Complement - Inflammation's Conductors
- Cytokines: Soluble proteins; orchestrate inflammatory responses.
- Pro-inflammatory:
- TNF-α, IL-1: Key acute inflammation mediators. Systemic: Fever, ↑endothelial adhesion molecules, ↑cytokines/chemokines; TNF → cachexia.
- IL-6: Induces liver's Acute Phase Protein synthesis (e.g., CRP); systemic fever.
- Chemokines (e.g., IL-8/CXCL8): Leukocyte chemotaxis, esp. neutrophils to injury site.
⭐ TNF, IL-1, and IL-6 are major cytokines mediating acute phase response.
- Pro-inflammatory:
- Complement System: Plasma proteins; activated via cascade.
- Activation Pathways: Classical (Antibody-Antigen complexes), Alternative (microbial surfaces), Lectin (mannose-binding lectin).
- Key Functions:
- C3b: Opsonization (tags microbes for phagocytosis). 📌 C3b Binds Bacteria.
- C3a, C5a: Anaphylatoxins (mast cell degranulation → histamine release, ↑vascular permeability); C5a also potent chemotactic agent.
- C5b-C9 (MAC): Cell lysis via Membrane Attack Complex. 📌 MAC punches holes.
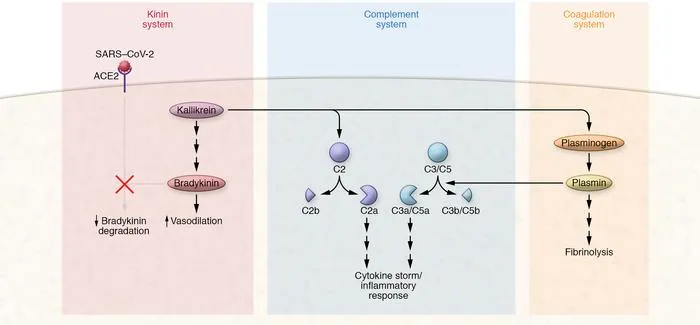
Chemical Mediators: Kinins, Clotting & Others - The Diverse Crew
- Kinin System: Plasma-derived; activated by Factor XII (Hageman factor).
- Bradykinin: ↑Vascular permeability, vasodilation, smooth muscle contraction, pain.
⭐ Bradykinin is a potent mediator of pain.
- Clotting System: Interlinked with inflammation.
- Thrombin: ↑Leukocyte adhesion, fibroblast proliferation.
- Fibrinopeptides: ↑Vascular permeability, chemotaxis.
- Platelet-Activating Factor (PAF): From diverse cells (platelets, leukocytes, endothelium). Actions: Vasodilation, ↑vascular permeability (potent: 100-10,000x > histamine), platelet aggregation, chemotaxis.
- Nitric Oxide (NO): Synthesized via $L-arginine \xrightarrow{NOS} NO$. Vasodilator, ↓platelet aggregation & adhesion, microbicidal.
- Lysosomal Components: From neutrophils & macrophages. Enzymes (e.g., elastase, collagenase) cause tissue damage.
- Oxygen Radicals: E.g., $O_2^{\cdot-}$, $H_2O_2$, $OH^{\cdot}$. Cause endothelial damage, inactivate antiproteases, injure cells.
High‑Yield Points - ⚡ Biggest Takeaways
- Histamine & Serotonin: Early vasodilation & ↑ vascular permeability.
- Prostaglandins (COX): PGE2 (pain, fever); PGI2 (vasodilation, inhibits platelet aggregation).
- Leukotrienes (LOX): LTB4 (chemotaxis); Cysteinyl LTs (bronchospasm, ↑ permeability).
- Cytokines (TNF, IL-1, IL-6): Drive fever, acute phase proteins, endothelial activation.
- Complement C3a & C5a: Anaphylatoxins; C5a also for chemotaxis & leukocyte activation.
- Bradykinin: Key mediator of pain and vasodilation.
- Chemokines (e.g., IL-8): Crucial for leukocyte recruitment (chemotaxis).
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

