Overview & Pathways - Sinus Sneak Attack
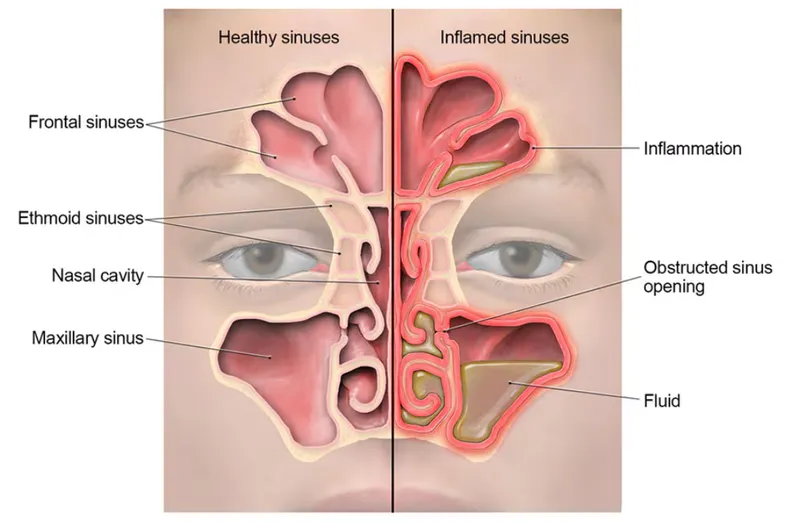
- Routes of Spread:
- Direct: Through sinus walls (osteitis); common for orbital issues.
- Hematogenous: Via valveless diploic veins (Batson's plexus).
- Lymphatic: Less common.
- Predisposing Factors:
- Pathogen virulence (toxins, biofilms).
- Host immunity (↓ e.g., diabetes, HIV).
- Sinus anatomy (e.g., OMC obstruction).
- Key Pathogens:
- Strep. pneumoniae, H. influenzae (non-type B), M. catarrhalis.
- Staph. aureus (chronic/post-op).
- Anaerobes (Bacteroides, Peptostreptococcus) in chronic cases.
⭐ Frontal sinusitis is most commonly associated with intracranial complications (e.g., epidural abscess, meningitis).
Orbital Complications - Eye-Popping Perils
Orbital complications of sinusitis, mainly from ethmoiditis, are critical. Chandler's Classification (I-V) guides diagnosis (CT scan essential) and management.
- Chandler's Classification:
- I: Inflammatory Edema (Preseptal): Lid swelling, erythema. Vision, EOMs normal. Rx: Antibiotics.
- II: Orbital Cellulitis: Proptosis, chemosis, ophthalmoplegia, ↓ vision. Rx: IV antibiotics.
⭐ Proptosis with ophthalmoplegia and decreased vision indicates orbital involvement (Stage II+), mandating urgent CT.
- III: Subperiosteal Abscess: Globe displacement, proptosis. Rx: IV antibiotics; drainage if no improvement in 24-48h or vision loss.
- IV: Orbital Abscess: Severe proptosis, ophthalmoplegia, marked ↓ vision. Rx: Urgent surgical drainage, IV antibiotics.
- V: Cavernous Sinus Thrombosis: Bilateral signs, CN palsies (III,IV,V,VI), sepsis. Rx: High-dose IV antibiotics, anticoagulation.
📌 Mnemonic: "Pretty Orbitals Sometimes Offer Chaos" (Preseptal, Orbital cellulitis, Subperiosteal abscess, Orbital abscess, Cavernous sinus thrombosis).

Intracranial Complications - Brain Under Siege
Sinus infection breaching skull. Life-threatening. Early diagnosis vital.
-
Key Complications: 📌 MEBS-C
- Meningitis: Meningeal inflammation. Headache, fever, neck stiffness.
- Epidural Abscess (EDA): Pus: dura-skull. Fever, localized headache.
- Subdural Empyema (SDE): Pus in subdural space. Rapid decline. Neurosurgical emergency.
⭐ Subdural empyema is a neurosurgical emergency often secondary to frontal or ethmoidal sinusitis.
- Brain Abscess (BA): Intraparenchymal pus. Focal deficits, ↑ICP signs.
- Cavernous Sinus Thrombosis (CST): Clot. Proptosis, ophthalmoplegia (CN III, IV, VI), chemosis.
-
Warning Signs (Red Flags):
- Headache (severe, persistent)
- Fever (high)
- Focal Neurological Deficits (e.g., weakness, CN palsy)
- Seizures
- Altered mental status
-
Diagnosis:
- CT with contrast: Initial scan.
- MRI with gadolinium: Gold standard for detail, early changes, venous thrombosis.
-
Management:
- Medical: High-dose IV antibiotics (broad-spectrum, CNS penetrating).
- Surgical: Urgent drainage of abscess/empyema & infected sinuses.

Osseous & Other Issues - Bone Deep & Beyond
- Osteomyelitis: Bone infection/inflammation.
- Pott's Puffy Tumor: Frontal bone osteomyelitis with subperiosteal abscess. Classic: doughy, tender frontal swelling.
⭐ Pott's Puffy Tumor presents as a doughy, tender swelling over the frontal sinus.

- Pott's Puffy Tumor: Frontal bone osteomyelitis with subperiosteal abscess. Classic: doughy, tender frontal swelling.
- Mucocele & Pyocele:
- Mucocele: Mucus-filled, expansile cyst from blocked sinus ostium. Common: frontal, ethmoid. (📌 FEMS)
- Pyocele: Infected mucocele (pus-filled).
- Symptoms: Mass effect (headache, proptosis, diplopia).
- CT: Homogenous, expansile lesion, bony erosion. Pyocele may rim-enhance.
- Treatment: Surgical: marsupialization or excision.
High‑Yield Points - ⚡ Biggest Takeaways
- Orbital complications are most common: preseptal/orbital cellulitis, subperiosteal/orbital abscess, cavernous sinus thrombosis.
- Pott's puffy tumor: frontal bone osteomyelitis due to frontal sinusitis, presenting as forehead swelling.
- Intracranial spread leads to meningitis, brain abscess, epidural/subdural abscesses.
- Cavernous sinus thrombosis: ophthalmoplegia, proptosis, CN palsies (III, IV, V1, V2, VI).
- Mucocele/Pyocele: Chronic expanding lesions, typically frontoethmoidal.
- Orbital apex syndrome: involves CN II, III, IV, V1, VI; indicates posterior orbital involvement.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

