SCC Basics - Sunny Side Scourge
- Malignant tumor of epidermal keratinocytes, often showing keratinization (keratin pearls).
- Second most common skin cancer (after BCC); higher metastatic potential than BCC.
- Key Risk Factors:
- Sun Exposure: Chronic UVB > UVA. Main cause for cutaneous SCC.
- Immunosuppression: Organ transplant recipients (↑65-250x risk), HIV.
- Chronic Inflammation: Scars (Marjolin's ulcer), chronic ulcers, sinuses (e.g., osteomyelitis).
- HPV: Esp. types 16, 18 (anogenital, periungual, oral SCC).
- Chemicals: Arsenic, tar, soot.
- Radiation: Ionizing radiation.
- Genetic: Xeroderma Pigmentosum (XP), Albinism, Epidermolysis Bullosa.
- Precursors: Actinic keratosis (AK), Bowen's disease (SCC in situ), Leukoplakia.
⭐ UVB radiation (290-320 nm) is the most implicated etiological factor for cutaneous SCC, primarily through formation of pyrimidine dimers.
 oka
oka
Clinical Canvas - Spot the Suspect
- Presentation: Firm, indurated papules, plaques, or nodules; often scaly, crusted, ulcerated, or hyperkeratotic. Friable, bleeds easily.
- Common sites: Sun-exposed skin (face, ears, lower lip, hands), mucous membranes.
- Key Variants:
- SCC in situ (Bowen's Disease): Well-defined, erythematous, scaly patch/plaque. Non-invasive.
- Genital variant: Erythroplasia of Queyrat.
- Keratoacanthoma (KA): Rapidly growing, dome-shaped nodule with central keratin plug. "Crateriform."
- ⭐ Marjolin's Ulcer:
Marjolin's ulcer, an SCC arising in chronic wounds, burns, or scars (e.g., chronic osteomyelitis sinus tracts), is often more aggressive and has a higher metastatic potential.
- SCC in situ (Bowen's Disease): Well-defined, erythematous, scaly patch/plaque. Non-invasive.
- Symptoms: Often asymptomatic; may be tender or pruritic. Perineural invasion (PNI) can cause pain, paresthesia.
Microscopic Clues & Staging - Deep Dive Diagnosis
- Biopsy is Gold Standard: Confirms SCC.
- Histopathology (HPE):
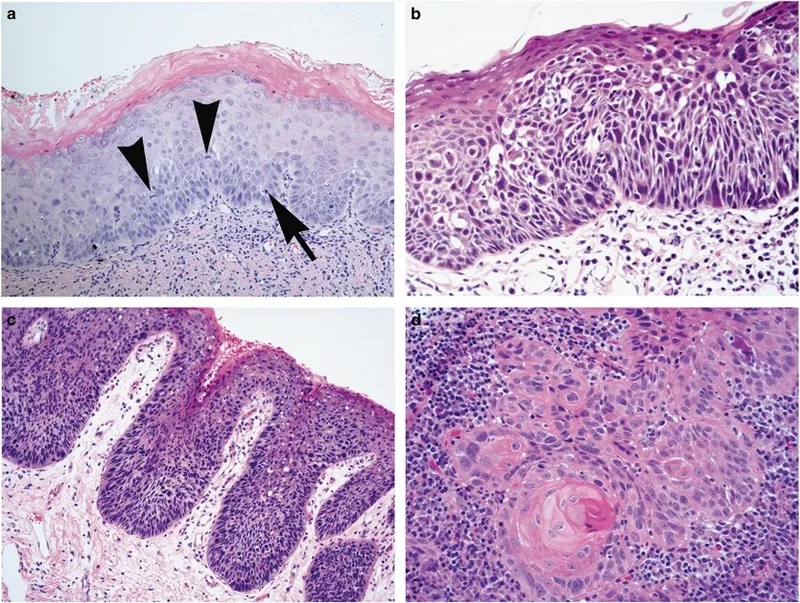
- Atypical squamous cells: Invasive cords/nests.
- Keratin pearls (📌 "Onion rings").
- Intercellular bridges (desmosomes).
- Cellular pleomorphism, hyperchromasia, ↑mitotic activity.
- Grading: Well, moderately, poorly differentiated.
⭐ Histopathologically, SCC is characterized by invasive cords and nests of atypical squamous epithelial cells with features like keratin pearls, intercellular bridges, and varying degrees of differentiation.
- Histopathology (HPE):
- Staging (AJCC TNM 8th Ed.): Guides prognosis & treatment.
- T (Tumor): Size & invasion depth.
- T1: ≤ 2 cm. T2: >2-4 cm. T3: >4 cm/PNI/deep invasion. T4: Bone/skull base.
- N (Nodes): Regional lymph node spread.
- N1: Single ipsilateral ≤ 3 cm.
- M (Metastasis): Distant spread.
- M1: Present.
- T (Tumor): Size & invasion depth.
Treatment Tactics - Eradication Roadmap
- Risk Stratification: Guides therapy (Low vs. High-risk).
- Surgical (Primary):
- Excision: Margins 4-6 mm (low-risk), 6-10 mm (high-risk).
- Curettage & Electrodessication (C&E): Small, low-risk.
- Cryosurgery: Superficial, low-risk.
⭐ Mohs Micrographic Surgery (MMS) is the treatment of choice for high-risk SCCs (e.g., large size, aggressive histology, recurrent, critical anatomical sites like face/ears/hands) due to its high cure rate and maximal tissue conservation.
- Non-Surgical:
- Radiotherapy (RT): Primary or adjuvant.
- Topical: 5-Fluorouracil (5-FU), Imiquimod (SCC in situ/Bowen's).
- Advanced/Metastatic: Systemic (Immunotherapy, Chemotherapy, EGFR inhibitors).
- Adjuvant: RT for high-risk features (PNI, +margins).
- Prevention: Sun protection, skin checks.

High‑Yield Points - ⚡ Biggest Takeaways
- Second most common skin cancer, arises from epidermal keratinocytes.
- Major risk: Chronic sun exposure (UVB). Others: immunosuppression, HPV, chronic scars (Marjolin's ulcer), arsenic.
- Precursors: Actinic keratosis, Bowen's disease (SCC in situ).
- Clinically: Indurated, scaly, crusted, or ulcerated lesion, often bleeds easily.
- Higher metastatic risk than BCC; lip/ear lesions, perineural invasion, and immunosuppression are high-risk factors.
- Diagnosis: Full-thickness biopsy. Treatment: Surgical excision; Mohs for high-risk lesions.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

