CNS Complications: Stroke & Seizures - Brainy Blues
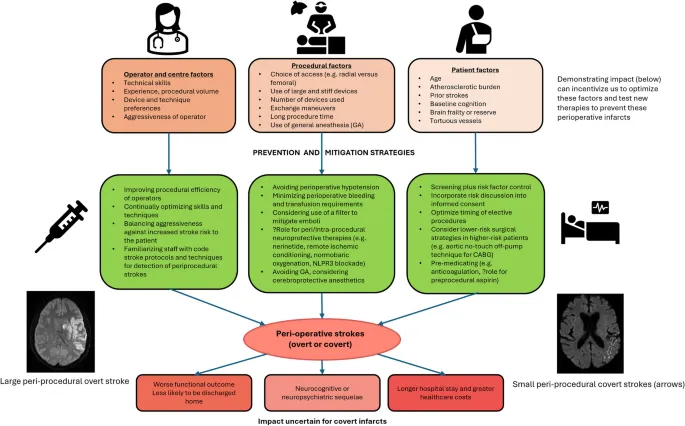
- Perioperative Stroke:
- Incidence: 0.1-1%; ↑ risk in cardiac, neuro, major vascular surgery.
- Types: Ischemic (~80%; e.g., hypotension, embolism); Hemorrhagic (e.g., HTN, anticoagulation).
- Risk Factors: Age >65, prior stroke, HTN, DM, AF.
- Prevention: Maintain MAP ±20% baseline; avoid severe hypocapnia; glycemic control.
- Mgmt: ABCs, neuro consult, imaging, specific therapy.
- Perioperative Seizures:
- Causes: Hypoxia, hypoglycemia, electrolytes (Na↓, Ca↓, Mg↓), drugs (LA toxicity, meperidine, tramadol), withdrawal, epilepsy.
- Mgmt:
- ABCs, 100% O2.
- Terminate: Benzodiazepines (IV lorazepam 0.1 mg/kg).
- Second-line: Phenytoin, levetiracetam.
- Treat cause.
⭐ Perioperative strokes are predominantly ischemic, often linked to intraoperative hypotension or embolic events.
Cognition & Awareness - Mind Matters
- Postoperative Cognitive Dysfunction (POCD):
- Subtle, persistent decline in cognitive functions (memory, concentration) post-surgery.
- Risk factors: Age >60 years, pre-existing cognitive impairment, major surgery (especially cardiac), longer anaesthesia duration.
- Prevention: Multimodal approach; optimize baseline health, consider regional techniques, effective pain management.
- Postoperative Delirium:
- Acute, fluctuating disturbance in attention, awareness, and cognition.
- Risk factors: Elderly, polypharmacy (benzodiazepines, anticholinergics), infection, metabolic disturbances, ICU stay.
- Assessment: Confusion Assessment Method (CAM).
- Management: Treat underlying cause, supportive care, reorientation, environmental modifications.
- Awareness with Recall (AWR):
- Explicit recall of intraoperative events. Incidence: 0.1-0.2%.
- Higher risk: Cardiac surgery, trauma, C-sections, TIVA, inadequate anaesthetic depth, muscle relaxant use.
- Prevention: Depth of anaesthesia monitoring (e.g., BIS target 40-60), end-tidal anaesthetic concentration (ETAC) monitoring.
- 📌 Mnemonic AWARE: Anaesthesia depth inadequate, Woman (higher risk), Anaesthetic delivery issues, Relaxants used, Emergency surgery/trauma.
⭐ BIS monitoring with a target range of 40-60 is a key strategy to minimize the risk of Awareness with Recall during general anaesthesia.
Spinal Cord & PNS Injuries - Nerve Knots
- Neuraxial Catheter Knotting:
- A rare complication involving epidural or spinal catheters.
- Risk factors: excessive insertion length (e.g., > 5 cm beyond needle tip for epidural; > 2-3 cm for spinal), coiling of catheter, significant patient movement.
- Clinical signs: difficulty with injection or aspiration, unusual resistance during catheter removal, new-onset paresthesia.
- Management: gentle, steady traction; altering patient position; injecting saline to distend space; fluoroscopic guidance for removal. Surgical intervention is rarely required.
- Prevention: limit catheter insertion depth to minimum effective length, secure catheter properly.
- Focal Nerve Lesions (Perceived as "Knots"):
- Etiology: direct trauma from needle, sustained compression (e.g., improper patient positioning), hematoma formation, excessive nerve stretch.
- Commonly affected nerves: ulnar nerve (at elbow), brachial plexus, common peroneal nerve (at fibular head), sciatic nerve.
- Symptoms: localized pain, paresthesia, numbness, or motor weakness corresponding to the affected nerve's distribution.
- Prevention: meticulous anesthetic technique, careful patient positioning with adequate padding, avoiding extreme joint positions, regular checks.
⭐ Ulnar neuropathy is the most frequently reported perioperative peripheral nerve injury, typically resulting from compression or stretch of the nerve at the elbow.
Prevention & Management - Safe Signals
- Prevention Strategies:
- Pre-anesthetic: Detailed neuro Hx, risk stratification (elderly, DM, PVD, prior neuro deficit).
- Positioning: Careful padding, limit extreme positions, avoid nerve compression/stretch (brachial plexus, ulnar, common peroneal).
- Physiological: Maintain normotension (MAP >65-70 mmHg), normoxia, normocapnia, euglycemia, normothermia.
- Regional: Ultrasound guidance, low injection pressure, incremental dosing, avoid neurotoxic additives.
- Intraoperative Monitoring (Safe Signals):
- Standard ASA monitors. Consider arterial line for beat-to-beat BP.
- Advanced (high-risk): IONM (SSEP, MEPs, BAEPs, EMG) to detect early compromise.
- Post-operative Management Protocol:
⭐ During regional anesthesia, if patient reports sharp pain or paresthesia on injection ("electric shock"), withdraw needle immediately to prevent intraneural injection. (📌 Mnemonic: Stop Pain Alerts Nerve = SPAN)
High‑Yield Points - ⚡ Biggest Takeaways
- POCD & delirium are frequent post-op, especially in elderly patients.
- Perioperative stroke risk factors: hypotension, hypoxia, major cardiac/carotid surgery.
- Seizures can be due to LA toxicity, hypoxia, hypoglycemia, or specific drugs.
- Awareness with recall: Higher risk with TIVA, muscle relaxants, difficult intubation.
- Ulnar nerve is the most common peripheral nerve injury from malpositioning.
- Spinal epidural hematoma/abscess: Rare but critical causes of post-neuraxial cord injury.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

