Layers Unveiled - Layers Unveiled
Four fundamental layers (lumen outwards):
- Mucosa:
- Epithelium: Protection, secretion, absorption (region-specific).
- Lamina Propria: CT, glands, vessels, MALT.
- Muscularis Mucosae: Smooth muscle, local folds.
- Submucosa:
- Dense CT.
- Vessels, lymphatics.
- Meissner's plexus: Glandular secretion, blood flow.
- Muscularis Externa:
- Inner Circular (smooth muscle).
- Outer Longitudinal (smooth muscle).
- Auerbach's (Myenteric) plexus: Between layers, controls peristalsis.
- Serosa/Adventitia:
- Serosa: Mesothelium + CT (intraperitoneal).
- Adventitia: CT (retroperitoneal).
📌 Mnemonic: M.S.M.S. (Mucosa, Submucosa, Muscularis Externa, Serosa/Adventitia)

⭐ Auerbach's (Myenteric) plexus, between muscularis externa layers, is the primary controller of GI motility (peristalsis).
Esophagus & Stomach Secrets
- Esophagus:
- Epithelium: Non-keratinized stratified squamous (protection).
- Submucosa: Esophageal glands proper (mucus).
- Muscularis Externa: Upper 1/3 skeletal, middle 1/3 mixed, lower 1/3 smooth.
- Outer layer: Adventitia (thoracic), Serosa (abdominal).
- Gastroesophageal Junction (GEJ):
- Sharp epithelial change: Stratified squamous to simple columnar. Z-line.

- Sharp epithelial change: Stratified squamous to simple columnar. Z-line.
- Stomach:
- Epithelium: Simple columnar; surface mucous cells (alkaline mucus). Gastric pits & glands.
- Gastric Glands (Fundus/Body):
- Parietal (Oxyntic) cells: HCl, Intrinsic Factor. 📌 "P"arietal "P"umps "P"rotons & IF.
- Chief (Zymogenic) cells: Pepsinogen, gastric lipase.
- Enteroendocrine cells (e.g., G cells - gastrin; D cells - somatostatin).
- Pyloric Glands (Antrum): Primarily mucous cells, many G cells.
- Muscularis Externa: 3 layers (inner oblique, middle circular, outer longitudinal).
⭐ Barrett's esophagus: Intestinal metaplasia (goblet cells) in distal esophagus; ↑ risk of adenocarcinoma.
Absorption Architects - Absorption Architects
- Surface Area Amplification (SA↑):
- Plicae Circulares (Kerckring): Submucosal folds; prominent in jejunum.
- Villi: Mucosal projections; core: lamina propria, lacteal (fats).
- Microvilli: Enterocyte apical surface (striated/brush border).
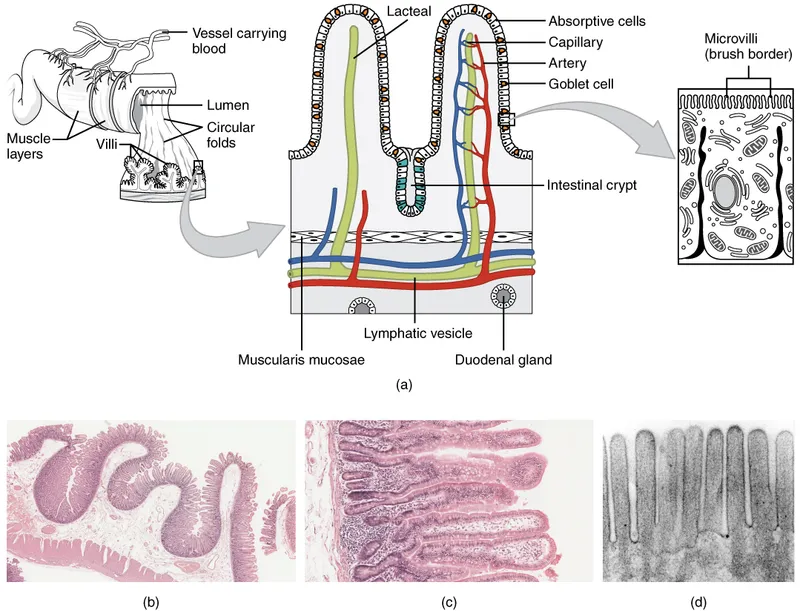
- Epithelial Cell Lineup:
- Enterocytes: Columnar, absorptive.
- Goblet Cells: Mucus; count ↑ distally (ileum).
- Paneth Cells: Crypt base; antimicrobial (lysozyme, defensins). Eosinophilic granules.
- Enteroendocrine Cells: Gut hormones.
- Regional Highlights (Proximal to Distal):
- Duodenum: Brunner's glands (submucosa, alkaline $HCO_3^-$). 📌 Brunner's = Bicarbonate. Leaf-shaped villi.
- Jejunum: Longest villi, maximal plicae. Primary absorption site.
- Ileum: Peyer's patches (submucosal lymphoid aggregates). Shortest villi. Vit B12/bile absorption.
⭐ Peyer's patches, large aggregates of lymphoid tissue, are a hallmark histological feature of the ileum's submucosa, crucial for gut immunity.
- Water & Waste Wranglers
- Large Intestine: Water absorption, mucus secretion, waste storage.
- Colon: No villi. Abundant goblet cells, straight crypts. Colonocytes (absorption). GALT. Muscularis externa: Taeniae coli, haustra. Appendices epiploicae.
- Rectum: Taeniae coli fuse. Transverse rectal folds (Valves of Houston).
- Anal Canal:
- Epithelial zones: Columnar → ATZ (strat. columnar/cuboidal) → Squamous (strat. squamous, keratinized at verge).
- Pectinate Line: Divides neurovascular supply & epithelium.
- Above: Columnar, autonomic (no pain), sup. rectal vessels (portal).
- Below: Squamous, somatic (pain), inf. rectal vessels (systemic).
- Sphincters: Internal (smooth), External (skeletal). Anal glands.
⭐ The pectinate line marks the transition from hindgut (endoderm) to proctodeum (ectoderm) derivatives.
 oka
oka
High‑Yield Points - ⚡ Biggest Takeaways
- Meissner's (submucosal) plexus and Auerbach's (myenteric) plexus control gut motility and secretion.
- Brunner's glands in duodenal submucosa secrete alkaline mucus, neutralizing gastric acid.
- Peyer's patches (lymphoid aggregates) are characteristic of the ileal lamina propria/submucosa.
- Paneth cells, containing eosinophilic granules (lysozyme, defensins), reside at the base of intestinal crypts.
- Goblet cell abundance increases progressively from the duodenum to the colon.
- Barrett's esophagus involves intestinal metaplasia: stratified squamous to columnar epithelium with goblet cells.
- Absence of ganglion cells in Auerbach's and Meissner's plexuses is diagnostic for Hirschsprung's disease (aganglionic megacolon).
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

