Teratogens: Principles & Timing - Bad News Bearers
- Teratogen: Agent (e.g., drug, infection, radiation) causing congenital anomalies (structural/functional).
- Key Principles (Wilson's):
- Susceptibility: Varies (maternal/fetal genotype, developmental stage).
- Critical Periods: Organ-specific vulnerability windows (e.g., CNS continuous; Heart: wks 3-6; Limbs: wks 4-7).
- Dose-Response: ↑dose generally → ↑effect severity; threshold may exist.
- Specific Mechanisms: Unique pathways leading to defined outcomes.
- Outcomes: Death, malformation, growth restriction, functional deficits.
- Significance of Timing:
- Pre-implantation (<2 weeks post-conception): "All-or-none" effect (embryo death or normal development).
- Embryonic Period (3-8 weeks): Peak susceptibility; major structural anomalies.
- Fetal Period (>8 weeks to birth): Functional defects, minor structural anomalies, growth issues.
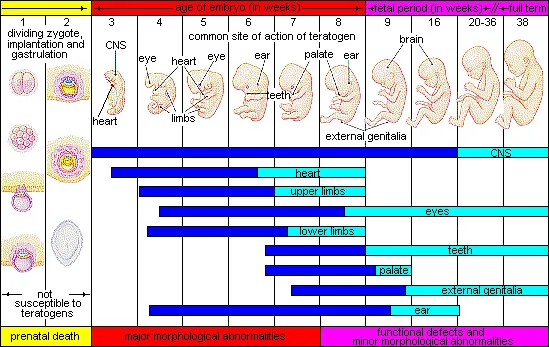
⭐ The first 2 weeks post-conception are often considered an 'all-or-none' period for teratogenic effects.
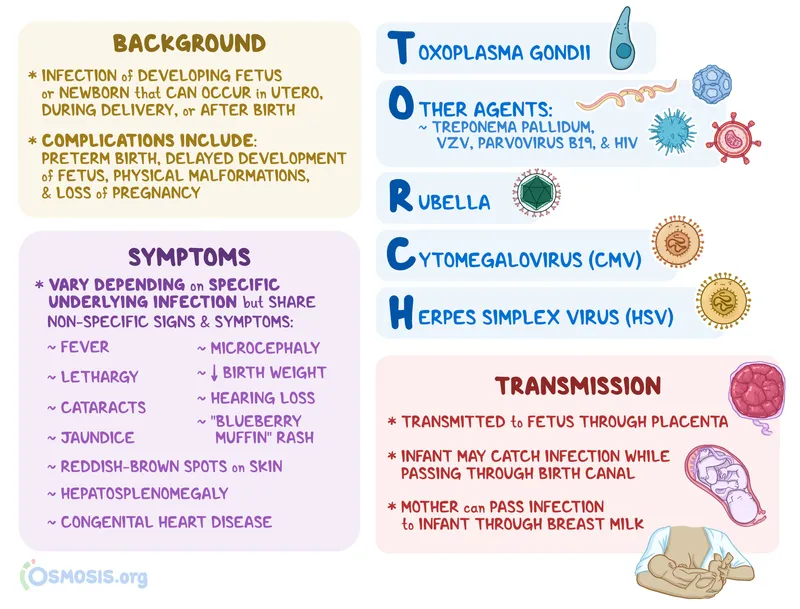
Infectious Teratogens: TORCH - Tiny Trouble Makers
📌 TORCH complex: Key group of congenital infections causing significant neonatal morbidity. Early maternal diagnosis & intervention are crucial.
| Agent | Key Manifestations | Notes/Prevention |
|---|---|---|
| Toxoplasmosis | Triad: Chorioretinitis, hydrocephalus, intracranial calcifications | Avoid raw meat, cat litter. |
| Other: Syphilis | Hutchinson's triad (keratitis, teeth, deafness), saddle nose | Maternal screen (VDRL/RPR) & penicillin. |
| Other: VZV | Limb hypoplasia, skin scars, microcephaly | Pre-pregnancy vaccine; VZIG if exposed. |
| Other: Parvo B19 | Hydrops fetalis, severe anemia | Supportive; IUT for severe anemia. |
| Rubella | Deafness, cataracts, cardiac (PDA), "blueberry muffin" rash | MMR vaccine (pre-pregnancy). |
| CMV | Hearing loss (commonest), periventricular calcifications, microcephaly | Hand hygiene. Ganciclovir if symptomatic. |
| HSV | Skin vesicles, encephalitis, keratoconjunctivitis | C-section (active lesions); Acyclovir. |
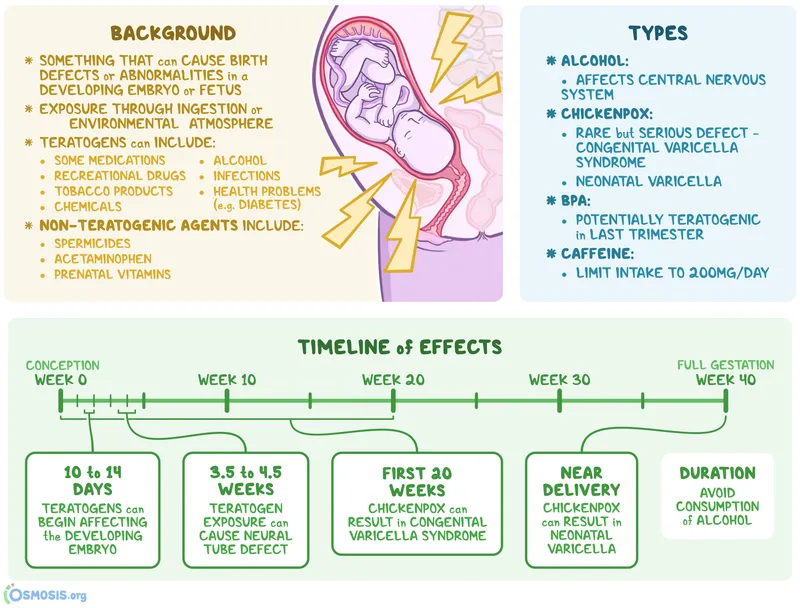
Chemical & Drug Teratogens - Potions & Poisons
Key teratogens, critical exposure periods, and primary effects:
| Teratogen | Critical Period (Gestation) | Primary Effects |
|---|---|---|
| Thalidomide | Weeks 4-8 | Phocomelia, limb defects |
| Alcohol (FAS) | Throughout | Microcephaly, facial dysmorphism. 📌 FAS Craniofacial, AIUGR, Neuro |
| Valproate | 1st trimester (esp. <30d) | Neural Tube Defects (NTDs), cardiac/limb defects |
| Phenytoin | Throughout | Fetal Hydantoin Syndrome (craniofacial, hypoplastic nails) |
| ACE Inhibitors | 2nd/3rd trimester | Renal dysgenesis, oligohydramnios |
| Isotretinoin | Weeks 2-5 | CNS, craniofacial, cardiac defects. Highly teratogenic. |
| Warfarin | Weeks 6-9 | Nasal hypoplasia, stippled epiphyses |
| Lithium | 1st trimester (<8wks) | Ebstein's anomaly (cardiac) |
| Lead | Throughout | Neurodevelopmental deficits, miscarriage |
| Mercury (Organic) | Throughout | Minamata disease (severe CNS damage) |
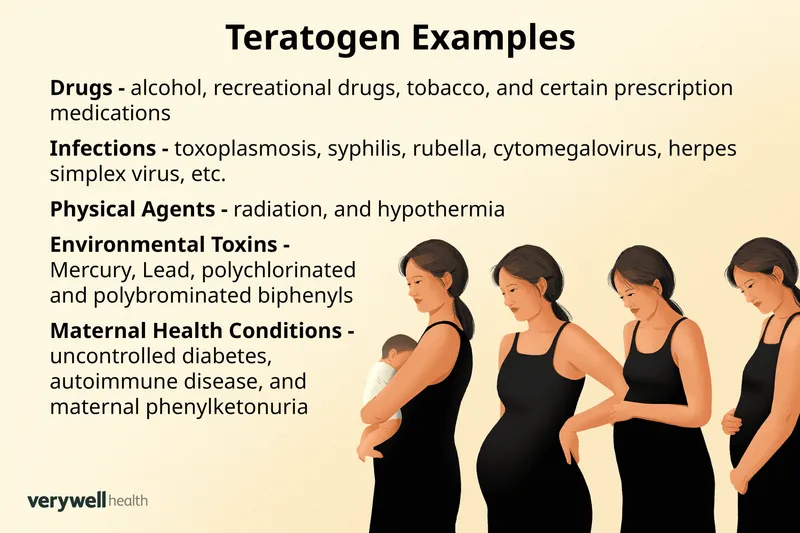
Physical & Maternal Factors - Womb Worries
- Radiation Exposure:
- Teratogenic, esp. organogenesis (2-8 weeks).
- CNS most sensitive: microcephaly, intellectual disability (ID).
- Risk if > 5-10 rads (0.05-0.1 Gy).
- Hyperthermia:
- Maternal fever > 38.9°C (1st trimester).
- Linked to Neural Tube Defects (NTDs), cardiac defects, facial clefts.
- Maternal Metabolic Conditions:
- Diabetes (Pre-gestational): Poor control → caudal regression, cardiac defects, NTDs, macrosomia.
- Phenylketonuria (PKU): ↑ Phenylalanine → microcephaly, ID, Congenital Heart Disease (CHD). Strict diet vital.
- Nutritional Deficiencies:
- Folic Acid: Deficiency → NTDs (spina bifida, anencephaly).
- Iodine: Deficiency → cretinism.
⭐ Maternal folic acid supplementation significantly reduces the risk of neural tube defects.
High‑Yield Points - ⚡ Biggest Takeaways
- TORCH infections (Toxoplasmosis, Rubella, CMV, HSV, Syphilis) are key causes of congenital anomalies.
- Fetal Alcohol Syndrome shows characteristic facial dysmorphism, growth retardation, and CNS defects.
- Thalidomide is linked to phocomelia (severe limb reduction defects).
- Valproic acid exposure significantly ↑ risk of neural tube defects.
- ACE inhibitors in 2nd/3rd trimesters cause renal dysgenesis and oligohydramnios.
- Maternal diabetes links to macrosomia, cardiac defects, and caudal regression syndrome.
- Radiation exposure (especially 8-15 weeks gestation) causes microcephaly and intellectual disability.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

