One Health & Principles - Zoonoses United
- Zoonoses: Diseases/infections naturally transmitted between vertebrate animals and humans.
- Prevention & Control Principles:
- Source Reduction: Control/eliminate pathogens in animal reservoirs (e.g., culling, animal vaccination).
- Breaking Transmission: Interrupt pathways (e.g., vector control, food safety, hygiene).
- Protecting Susceptible Hosts: Vaccination, chemoprophylaxis, health education for humans.
- One Health Triad: Interconnected health of Humans, Animals, Environment. Key for zoonoses.
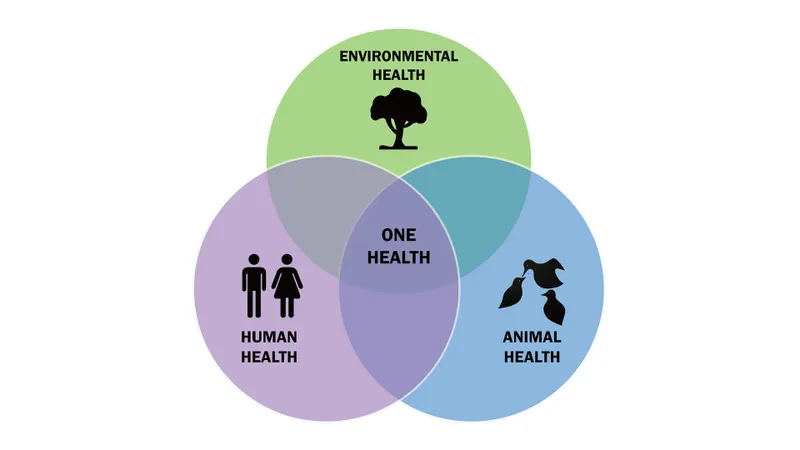
- Intersectoral Coordination: Vital collaboration: medical, veterinary, public health, environmental agencies for surveillance & response.
⭐ India's National One Health Programme for Prevention and Control of Zoonoses highlights this coordinated strategy.
Animal Reservoir Control - Critter Shield Up
- Animal Vaccination: Key defense.
- Dogs: Mass anti-rabies vaccination.
- Livestock: Anthrax, Brucellosis vaccines.
- Quarantine: Isolate infected/exposed animals.
- Culling/Slaughter: For highly contagious diseases (e.g., Avian Influenza).
- Vector Control: For JE, KFD.
- Chemical (insecticides), Biological (Gambusia fish), Environmental (source reduction, e.g., draining water).

- Chemical (insecticides), Biological (Gambusia fish), Environmental (source reduction, e.g., draining water).
- Animal Husbandry & Hygiene: Biosecurity, clean housing, proper waste disposal.
⭐ Mass dog vaccination (>70% coverage) is the most cost-effective measure for human rabies prevention.
Human & Environmental Control - Safety Bubble
- Personal Protective Equipment (PPE):
- Essential for high-risk occupations (vets, farmers, lab workers): gloves, masks, gowns, eye protection.
- Food Safety Practices:
- Thorough cooking of meat/eggs; pasteurization of milk (e.g., Brucellosis, Listeriosis).
- Hand hygiene: critical for preventing Salmonellosis, Taeniasis.

- Safe Water & Sanitation:
- Access to potable water; proper sewage & animal waste disposal.
- Environmental Decontamination:
- Disinfection of contaminated sites (e.g., anthrax); vector control; safe animal carcass disposal.
- Human Vaccination:
- Pre-exposure prophylaxis (PrEP) for Rabies (high-risk), Japanese Encephalitis, Yellow Fever.
- Post-Exposure Prophylaxis (PEP):
- Immediate, thorough wound washing (soap & water for 15 minutes).
- Specific PEP protocols, e.g., Rabies (RIG + vaccine).
⭐ Rabies: wound washing with soap and water for 15 minutes is a critical first step in PEP.
Surveillance & Outbreak Management - Disease Trackers
- Early Detection & Rapid Response: Paramount for effective control and limiting zoonotic disease spread.
- National Surveillance Programs:
- Key example: India's Integrated Disease Surveillance Programme (IDSP) for early warnings.
⭐ Integrated Disease Surveillance Programme (IDSP) is key for early warning signals of outbreaks in India.
- Essential Systems:
- Clear, standardized case definitions.
- Prompt, mandatory case reporting and notification.
- Outbreak Investigation Steps:
- Laboratory Role: Crucial for accurate diagnosis, case confirmation, and ongoing pathogen surveillance.
- Global Cooperation & Regulations:
- Adherence to International Health Regulations (IHR).
- Partnerships: WHO, OIE (World Organisation for Animal Health), FAO.
High‑Yield Points - ⚡ Biggest Takeaways
- One Health approach: Essential for integrating human, animal, environmental health.
- Surveillance & Reporting: Critical for early detection (IDSP) and rapid response.
- Vaccination: Key for animals (rabies, FMD, brucellosis) & humans (rabies, JE).
- Vector Control: Crucial for KFD, JE, Scrub Typhus, CCHF.
- Safe Practices: Vital in animal husbandry, food processing (hygiene, pasteurization).
- Inter-sectoral Coordination: Health, veterinary, wildlife, environment sectors must collaborate.
- Post-Exposure Prophylaxis (PEP): Lifesaving for rabies, anthrax; plus Chemoprophylaxis_
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

