Bacterial Zoonoses Intro - Animal Kingdom's Bugs
- Bacterial infections naturally transmissible from vertebrate animals to humans (and vice-versa: anthropozoonoses).
- Causative Agents: Diverse pathogenic bacteria.
- Animal Reservoirs: Include domestic (livestock, pets) and wild animals.
- Modes of Transmission:
- Direct contact: With infected animals, their tissues, or body fluids.
- Indirect contact: Via vectors (e.g., ticks, fleas), fomites, contaminated environment.
- Ingestion: Contaminated food (meat, milk) or water.
- Inhalation: Aerosolized particles.
- Represent a major global public health burden.

⭐ Many bacterial zoonoses are occupational hazards for veterinarians, farmers, and abattoir workers.
Anthrax & Listeriosis - Positive Perils
-
Anthrax (Bacillus anthracis): G+ spore-forming rod. From animals/products.
- Cutaneous: Painless black eschar, surrounding edema. Most common.
- Inhalational: Flu-like → hemorrhagic mediastinitis, shock. CXR: Widened mediastinum.
- Virulence: Poly-D-glutamate capsule, tripartite toxin (PA, EF, LF).
- Rx: Ciprofloxacin or Doxycycline.
- Cutaneous: Painless black eschar, surrounding edema. Most common.
-
Listeriosis (Listeria monocytogenes): G+ rod, intracellular.
- Transmission: Contaminated food (unpasteurized dairy, deli meats). Grows at 4°C (refrigeration).
- Clinical:
- Pregnant: Flu-like, risk to fetus (granulomatosis infantiseptica).
- Neonates/Immunocompromised: Meningitis, sepsis.
- Motility: Tumbling motility at 20-25°C; actin rockets.
- Rx: Ampicillin (+/- gentamicin).
⭐ Anthrax: Inhalational anthrax classically presents with a widened mediastinum on chest X-ray due to hemorrhagic mediastinitis.
Brucellosis & Plague - Notorious Nasties
Brucellosis (Undulant Fever / Malta Fever)
- Causative Agent: Brucella spp. (Gram-negative coccobacilli).
- Transmission: Unpasteurized dairy, contact with infected animals.
- Clinical: Undulant fever (rising & falling), sweats, arthralgia, hepatosplenomegaly.
- Diagnosis: Blood culture (Castaneda), Rose Bengal test, SAT.
- Treatment: Doxycycline + Rifampicin (standard 6 weeks).
Plague (Black Death)
- Causative Agent: Yersinia pestis (Gram-negative rod, bipolar "safety pin" staining).
- Vector: Rat flea (Xenopsylla cheopis).
- Forms & Features:
- Bubonic: Painful swollen lymph nodes (buboes).
- Septicemic: DIC, shock.
- Pneumonic: Highly infectious, hemoptysis.
- Treatment: Streptomycin or Gentamicin.
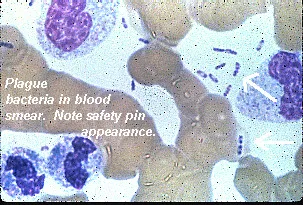
⭐ Yersinia pestis exhibits characteristic bipolar staining (Wayson or Giemsa stain), appearing like a "safety pin".
Leptospirosis & Q Fever - Query & Quagmire
Leptospirosis (Weil's Disease)
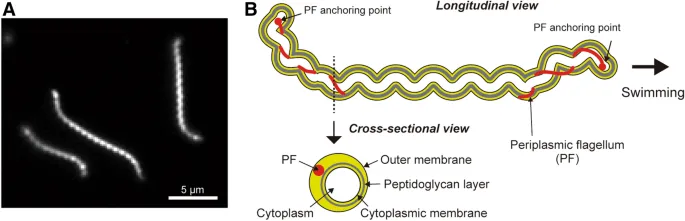
- Causative Agent: Leptospira interrogans (spirochete).
- Transmission: Contact with rodent urine-contaminated water/soil.
- Clinical: Biphasic illness.
- 1st phase (septicemic): Fever, myalgia (esp. calves), conjunctival suffusion.
- 2nd phase (immune/Weil's): Jaundice, renal failure, hemorrhage. 📌 JHK: Jaundice, Hemorrhage, Kidney failure.
- Diagnosis: Microscopic Agglutination Test (MAT) - Gold Standard.
- Treatment: Doxycycline, Penicillin G.
Q Fever (Query Fever)
- Causative Agent: Coxiella burnetii (obligate intracellular bacterium).
- Transmission: Inhalation of aerosols from infected livestock (esp. parturient products).
- Clinical:
- Acute: Abrupt fever, headache, atypical pneumonia, hepatitis. No rash.
- Chronic: Endocarditis (culture-negative), osteomyelitis.
- Diagnosis: Serology (IFA for phase I & II antibodies).
⭐ Coxiella burnetii endocarditis is a classic cause of culture-negative endocarditis.
- Treatment: Doxycycline (acute); Doxycycline + Hydroxychloroquine (chronic).
High‑Yield Points - ⚡ Biggest Takeaways
- Brucellosis: Undulant fever, B. melitensis commonest; occupational hazard (farmers, vets).
- Leptospirosis: Weil's disease (jaundice, renal failure, hemorrhage); from rodent urine.
- Plague: Yersinia pestis; bubonic (flea), pneumonic (droplet); bipolar staining (safety-pin).
- Anthrax: Bacillus anthracis; cutaneous eschar, inhalational (widened mediastinum); from livestock.
- Q Fever: Coxiella burnetii; atypical pneumonia, culture-negative endocarditis; from livestock aerosols.
- Tularemia: Francisella tularensis; ulceroglandular form; from ticks/rabbits.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more


