MHC Basics - Gene Scene Unveiled
- Definition: Cell surface glycoproteins for adaptive immune recognition.
- Function: Bind antigen fragments; present to T-lymphocytes; key for self/non-self discrimination.
- Gene Locus: Human Leukocyte Antigen (HLA) complex on chromosome 6 (short arm). 📌 "MHC Six".
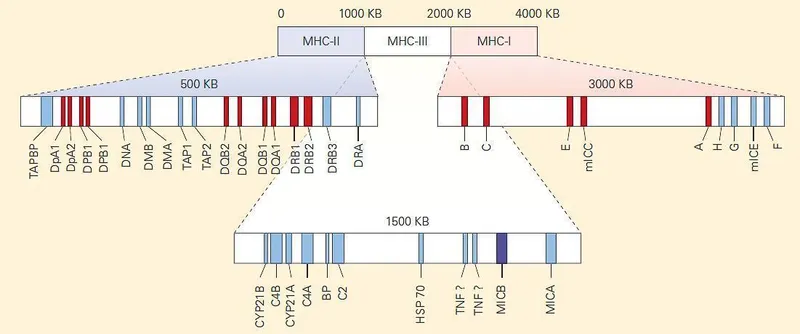
- Major Classes:
- MHC Class I: On all nucleated cells; presents to CD8+ T cells.
- MHC Class II: On Antigen Presenting Cells (APCs); presents to CD4+ T cells.
- MHC Class III: Encodes other immune proteins (complement, TNF-α).
⭐ MHC Restriction: T-cells recognize antigens only when presented by a specific self-MHC molecule.
MHC Class I - Cell's ID Card
- Structure: Heavy α chain (α1, α2, α3) & β2-microglobulin (β2m).
- Peptide Binding Cleft: Formed by α1 & α2; closed ends. Binds peptides of 8-10 aa.
- Antigen Source: Endogenous (intracellular, e.g., viral, tumor proteins).
- Antigen Processing: Cytosolic proteins → Proteasome → Peptides → TAP transporter to ER → MHC I loading.
- Expressed on: All nucleated cells.
- Presents to: CD8+ T cells (Cytotoxic T Lymphocytes).
- 📌 Mnemonic: Class I, CD8+ T cells: $1 \times 8 = 8$.
⭐ β2-microglobulin is crucial for MHC I expression on the cell surface; its non-covalent association with the α chain stabilizes the complex.
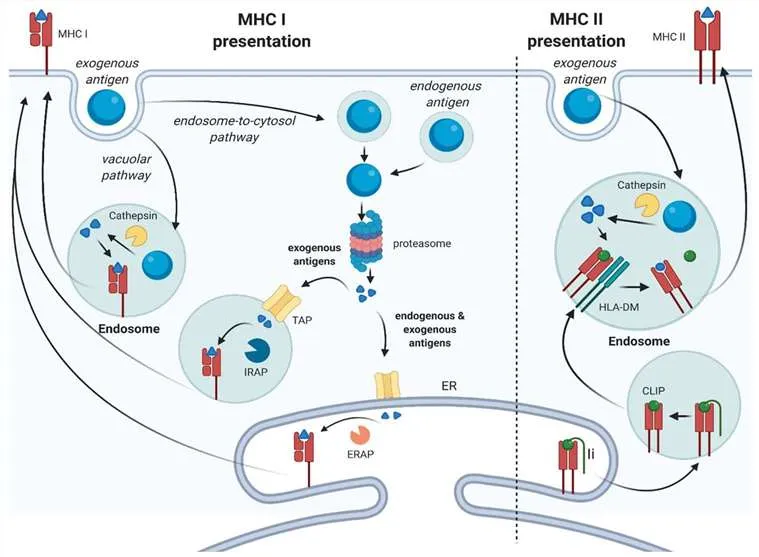
MHC Class II - Immune System's Scout
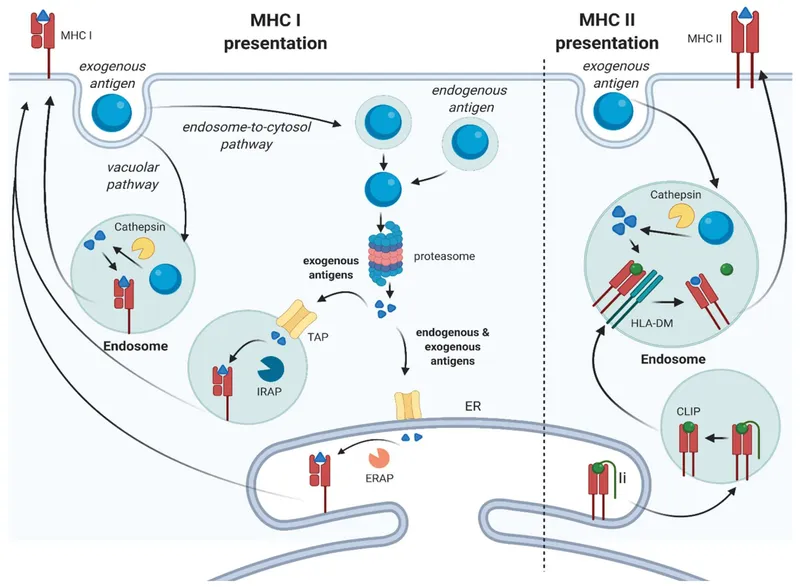
- Structure: Composed of one α chain and one β chain, both transmembrane.
- Peptide Binding Cleft: Open at both ends; binds peptides of 13-18 aa (or longer).
- Antigen Source: Exclusively exogenous antigens (e.g., bacteria) internalized by APCs.
- Expressed on: Professional Antigen Presenting Cells (APCs): Dendritic cells, Macrophages, B-lymphocytes.
- T-cell Interaction: Presents peptides to CD4+ T helper cells (Th). 📌 Mnemonic: MHC II interacts with CD4 ($2 \times 4 = 8$).
⭐ The Invariant chain (Ii) blocks the peptide-binding groove of MHC Class II in the ER, preventing premature binding, and directs it to endocytic vesicles for antigen loading.
HLA & Genetics - Diversity's Power Play
- Human Leukocyte Antigen (HLA): Human MHC proteins, crucial for immune recognition.
- Genetic Loci (Chromosome 6p21.3):
- Class I: HLA-A, HLA-B, HLA-C (on most nucleated cells).
- Class II: HLA-DP, HLA-DQ, HLA-DR (on antigen-presenting cells).
- Key Genetic Principles:
- Polymorphism: Numerous alleles for each gene; ensures population diversity.
- Polygeny: Multiple distinct genes for Class I & II molecules.
- Co-dominant Expression: Both maternal and paternal alleles are expressed.
- Haplotype Inheritance: HLA genes inherited as a set from each parent.

⭐ HLA genes exhibit linkage disequilibrium: certain alleles at different loci are inherited together more or less frequently than expected by chance due to close physical proximity on the chromosome.
MHC in Disease - Clinical Crossroads
- Transplantation: HLA typing is vital for organ/tissue compatibility, minimizing graft rejection. Mismatched MHC molecules are primary targets for recipient T-cell attack.
- Autoimmune Disease Associations: Specific HLA alleles predispose to autoimmunity:
HLA Allele Associated Disease(s) HLA-B27 Ankylosing Spondylitis (📌 AS) HLA-DR3/DR4 Type 1 Diabetes Mellitus HLA-DR4 Rheumatoid Arthritis - Infectious Diseases: MHC variants influence susceptibility and clinical course (e.g., HIV progression, Hepatitis B outcome).
⭐ HLA-B*5701 screening is mandatory before abacavir initiation to prevent severe drug hypersensitivity.
High‑Yield Points - ⚡ Biggest Takeaways
- MHC molecules present peptide antigens to T cells, crucial for adaptive immunity.
- MHC Class I (on all nucleated cells) presents endogenous antigens (e.g., viral, tumor) to CD8+ cytotoxic T cells.
- MHC Class II (on Antigen Presenting Cells) presents exogenous antigens to CD4+ helper T cells.
- HLA genes on chromosome 6p are highly polymorphic, key in transplant rejection and disease susceptibility.
- T cell activation requires recognition of antigen-MHC complex (MHC restriction).
- Strong HLA associations: HLA-B27 with ankylosing spondylitis; HLA-DR3/DQ2 with celiac disease.
- Bare Lymphocyte Syndrome: defects in MHC expression leading to severe immunodeficiency.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

