Overview & Pathways Intro - Cascade Crew
- System of ~30 plasma proteins (mainly liver-derived) acting sequentially in a cascade.
- Key component of innate immunity; bridges to adaptive immunity.
- Key Functions (📌 O-I-L-C):
- Opsonization (e.g., C3b) to enhance phagocytosis.
- Inflammation (anaphylatoxins: C3a, C5a).
- Lysis of pathogens (Membrane Attack Complex: C5b-C9).
- Clearance of immune complexes.
- Three Main Activation Pathways: Classical, Alternative, Lectin. All converge on C3 activation.
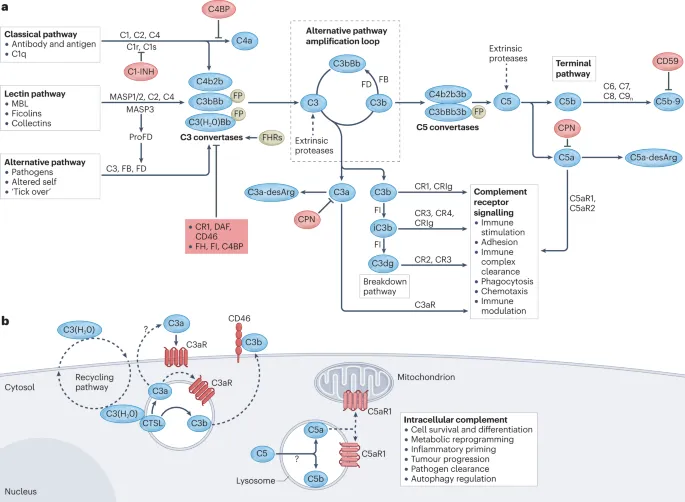
⭐ The complement system acts as a crucial bridge between innate and adaptive immunity, enhancing both pathogen clearance and antibody responses.
Activation Pathways - Triple Ignition
- Classical Pathway: (Adaptive immunity link)
- Trigger: Ag-Ab complexes (IgM is most efficient; also IgG1, IgG2, IgG3). C1q binds Fc of Ab.
- Initiation: C1 complex (C1q, C1r, C1s) activates. C1s (serine protease) cleaves C4 $\rightarrow$ C4b; C2 $\rightarrow$ C2b.
- C3 Convertase: $C4b2a$.
- Alternative Pathway: (Innate immunity; Antibody-independent)
- Trigger: Spontaneous C3 hydrolysis ($C3(H_2O)$ "tick-over"); direct C3b binding to pathogen surfaces (LPS, zymosan).
- Key Factors: C3b binds Factor B; Factor D cleaves Factor B (bound to C3b) $\rightarrow$ Bb. Properdin (P) stabilizes $C3bBb$.
- C3 Convertase: $C3bBb$.
- 📌 Alternative: Always active at low levels, rapid response.
- Lectin Pathway: (Innate immunity; Antibody-independent)
- Trigger: Mannose-Binding Lectin (MBL) or Ficolins bind specific microbial carbohydrates (e.g., mannose, N-acetylglucosamine).
- Initiation: MBL-Associated Serine Proteases (MASPs: MASP-1, MASP-2) activate. MASP-2 cleaves C4 and C2 (like C1s).
- C3 Convertase: $C4b2a$.
⭐ The generation of C3 convertase (e.g., $C4b2a$ for classical/lectin, $C3bBb$ for alternative) is the central and most critical amplification step in all complement pathways, cleaving many C3 molecules.
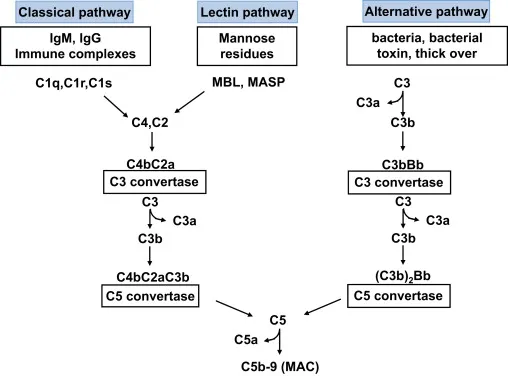
Effector Functions & Regulation - Power & Control
- Effector Functions (CRITICAL Outcomes):
- Opsonization & Phagocytosis: C3b (major), C4b.
- Inflammation: Anaphylatoxins C5a (potent), C3a, C4a → histamine release, ↑vascular permeability. C5a: neutrophil chemotaxis.
- Cell Lysis: Membrane Attack Complex (MAC) C5b-9 → pores, lysis.
- Immune Complex Clearance: C3b binds complexes → splenic/hepatic removal.
- Regulation (Preventing Host Damage):
- C1 Inhibitor (C1-INH): Serpin; dissociates C1r/C1s from C1q. Deficiency → Hereditary Angioedema (HAE).
- Factor H: Cofactor for Factor I → cleaves C3b to iC3b.
- Decay-Accelerating Factor (DAF/CD55): Dissociates C3 convertases (C4b2a, C3bBb).
- Protectin (CD59): Blocks C9 binding, prevents MAC assembly on host cells.
- S-protein (Vitonectin): Binds fluid-phase C5b-7, prevents bystander lysis.
- Carboxypeptidase N: Inactivates C3a, C5a.
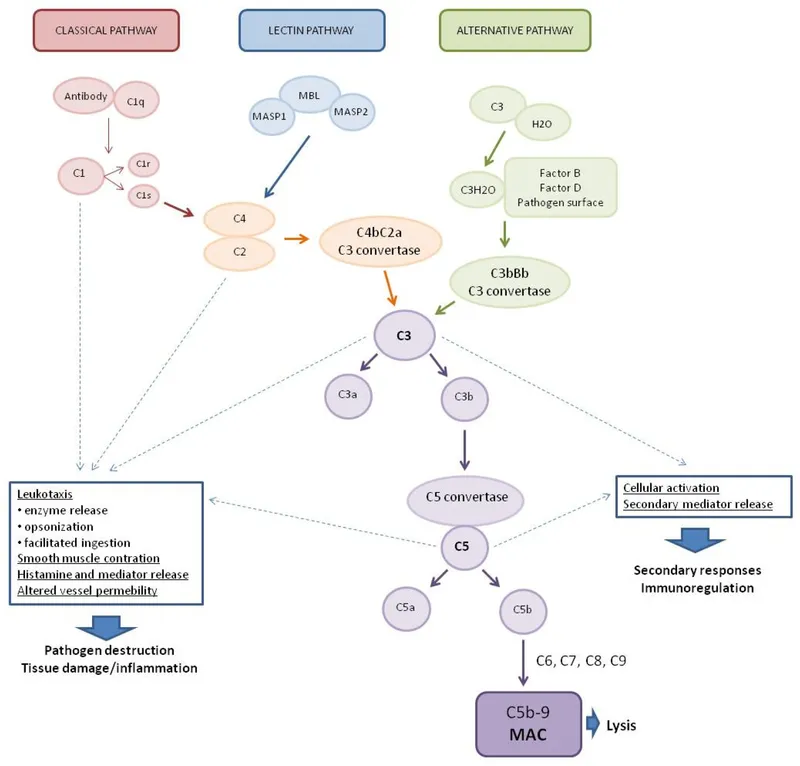
⭐ C3b is the primary opsonin of the complement system, facilitating phagocytosis, while C5a is a potent anaphylatoxin and chemoattractant for neutrophils.
Clinical Significance - System Under Siege
- Deficiencies & Disease:
- Early (C1q, C2, C4): SLE-like, pyogenic infections.
- C3: Severe pyogenic infections, GN.
- Properdin: ↑ Neisseria risk.
⭐ Deficiencies in terminal complement components (C5-C9) lead to a significantly increased susceptibility to recurrent infections by Neisseria species (e.g., N. meningitidis, N. gonorrhoeae).
- Dysregulation & Disease:
- PNH (CD55/CD59↓): IV hemolysis.
- HAE (C1-INH↓): Angioedema (bradykinin↑).
- aHUS (Factor H/I/MCP↓): TMA.
- Diagnostics:
- CH50: Classical/terminal screen.
- AH50: Alternative pathway screen.
High‑Yield Points - ⚡ Biggest Takeaways
- Three pathways activate complement: Classical (antibody-driven), Alternative (pathogen surfaces), and Lectin (mannose-binding lectin).
- All pathways converge to form C3 convertase; C3b is crucial for opsonization and forming C5 convertase.
- C5a is a potent anaphylatoxin and neutrophil chemoattractant; C3a is a weaker anaphylatoxin.
- The Membrane Attack Complex (MAC), C5b-C9, forms pores that lyse target cells, especially gram-negative bacteria.
- Key regulators like DAF (CD55) and CD59 (Protectin) prevent complement activation on host cells.
- C3 deficiency leads to severe, recurrent pyogenic infections and immune-complex disease.
- C5-C9 deficiencies (MAC defects) cause recurrent infections with Neisseria species (e.g., meningitis, gonorrhea).
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

