Basics & Importance - Germ Warfare 101
- Core Principle: Hand hygiene (HH) is the most effective measure to prevent Hospital Acquired Infections (HAIs).
- Mechanism: Interrupts pathogen transmission by contact.
- Targets: Bacteria (MRSA, VRE), viruses (Norovirus, Influenza), fungi.
- Impact: ↓ HAI rates, ↓ antimicrobial resistance (AMR), ↑ patient safety.
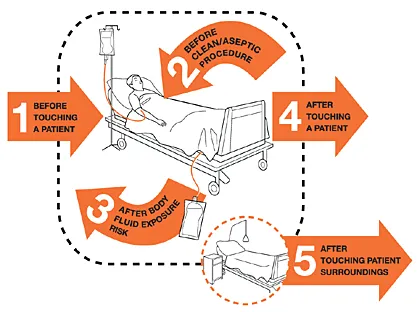
⭐ WHO's "My 5 Moments for Hand Hygiene": 1. Before patient contact. 2. Before aseptic task. 3. After body fluid exposure risk. 4. After patient contact. 5. After contact with patient surroundings.
WHO's 5 Moments - Hygiene Hotspots
- 1. Before Patient Contact:
- To protect the patient against harmful germs carried on your hands.
- 2. Before Clean/Aseptic Procedure:
- To protect the patient against harmful germs, including the patient’s own, from entering their body.
- 3. After Body Fluid Exposure Risk:
- To protect yourself and the healthcare surroundings from harmful patient germs.
- 4. After Patient Contact:
- To protect yourself and the healthcare surroundings from harmful patient germs.
- 5. After Contact with Patient Surroundings:
- To protect yourself and the healthcare surroundings from harmful patient germs.
⭐ Alcohol-based handrubs (ABHR) are the preferred method for routine hand hygiene when hands are not visibly soiled; effective duration is 20-30 seconds.
Techniques & Agents - Scrub & Rub Rituals
Core Principle: Adherence to WHO 6-steps for recommended duration is crucial.
1. Alcohol-Based Hand Rub (ABHR):
- Agent: Alcohol (60-80% Ethanol, Isopropanol); often with emollients.
- Duration: 20-30 seconds (until dry).
- Technique: Apply to dry hands, cover all surfaces using WHO 6 steps.
- Use: Preferred for routine decontamination if hands not visibly soiled.
- ⚠️ Ineffective against: C. difficile spores, Norovirus, protozoan oocysts; not for soiled hands.
2. Hand Wash (Soap & Water):
- Agent: Plain or antimicrobial soap.
- Duration: 40-60 seconds.
- Technique: Wet hands, apply soap, vigorous friction covering all surfaces (WHO 6 steps), rinse, dry thoroughly with clean towel.
- Use: Visibly soiled hands, after toilet use, before eating, suspected/confirmed C. difficile or Norovirus.
3. Surgical Hand Antisepsis:
- Agents: Chlorhexidine (CHG) 2-4%, Povidone-Iodine (PVP-I) 7.5-10%, or specific alcohol-based surgical rubs.
- Duration: 2-6 minutes for traditional scrub; ABHR application time as per manufacturer.
- Technique: From fingertips to elbows; clean under nails.

⭐ Alcohol-based hand rubs (ABHR) are ineffective against Clostridium difficile spores; meticulous hand washing with soap and water is essential in such cases.
Special Cases & Compliance - Beyond Routine & Sticking Power
- Clostridioides difficile (C. diff) & Other Spore-Formers (e.g., Anthrax):
- Alcohol-based hand rubs (ABHR) ineffective against spores.
- Mandatory: Soap & water handwash.
- Surgical Hand Antisepsis:
- Procedure: Pre-wash, then antiseptic agent (e.g., Chlorhexidine, Povidone-Iodine).
- Duration: 2-6 minutes.
- Area: Hands and forearms up to elbows.
- Improving Compliance:
- Key: WHO "My 5 Moments": 1. Before patient. 2. Before aseptic task. 3. After body fluid risk. 4. After patient. 5. After patient surroundings.
- Strategies: Education, visual reminders, audits & feedback, institutional support.
- "Bare below the elbows" policy.
⭐ In suspected or proven C. difficile infection, hand hygiene with soap and water is superior to ABHR due to alcohol's inefficacy against spores.
High‑Yield Points - ⚡ Biggest Takeaways
- Hand hygiene: Single most effective measure against HAIs.
- WHO's 5 Moments: Critical for interrupting pathogen transmission in patient care.
- Alcohol-based hand rubs (ABHRs): Preferred if hands not visibly soiled; rub for 20-30 seconds.
- Soap & water handwash: Essential for visibly soiled hands or with C. difficile; wash for 40-60 seconds.
- ABHRs: Must contain 60-80% alcohol for optimal germicidal activity.
- Non-compliance with hand hygiene is a major factor in HAI outbreaks.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

