AST Fundamentals - Test Tube Tales
- Purpose: Guides therapy, tracks resistance.
- Core Terms:
- MIC: Minimum Inhibitory Concentration; lowest drug level inhibiting visible growth.
- MBC: Minimum Bactericidal Concentration; lowest drug level killing 99.9% of bacteria.
- Breakpoint: MIC threshold defining Susceptible (S), Intermediate (I), Resistant (R).
- Breakpoint Utility:
- Clinical: Predicts treatment success.
- Epidemiological: Monitors resistance trends.
⭐ MIC is the lowest concentration of an antimicrobial that inhibits visible growth of a microorganism after overnight incubation.
Diffusion Methods - Zone Rangers
- Kirby-Bauer (Disk Diffusion) Test:
- Medium: Mueller-Hinton Agar (MHA), depth 4mm.
- Inoculum: Standardized to 0.5 McFarland turbidity.
- Incubation: 35°C for 16-18 hours (aerobic).
- Disks: Antibiotic-impregnated paper disks.
- Result: Measure zone of inhibition (ZOI) diameter.
- Zone Interpretation:
- Compare ZOI diameter to standards (CLSI/EUCAST).
- Categories: Susceptible (S), Intermediate (I), Resistant (R).
- Factors Affecting Zone Size:
- Inoculum density (↑ density → ↓ zone).
- Agar depth (↓ depth → ↑ zone).
- Temperature & time of incubation.
- Drug diffusion rate.
- Bacterial growth rate.
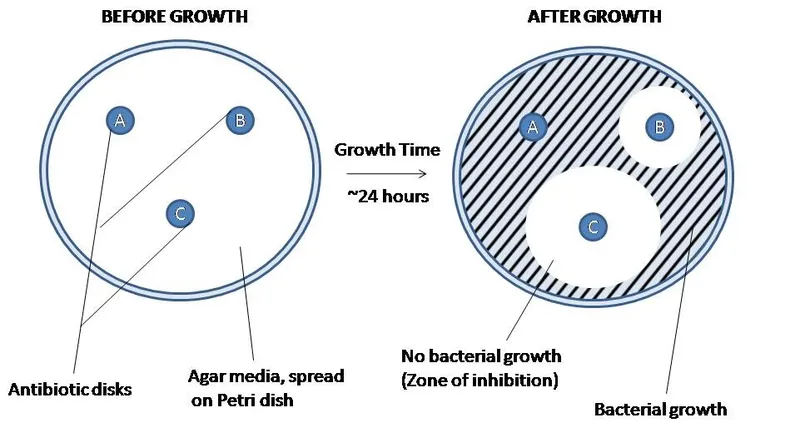
⭐ Mueller-Hinton Agar (MHA) is the standard medium for Kirby-Bauer testing due to its defined composition and minimal inhibition of common antimicrobials like sulfonamides and trimethoprim.
Dilution & Gradient Methods - Potion Potency
- Broth Dilution (Micro/Macro):
- Serial dilutions of antimicrobial in broth.
- Minimum Inhibitory Concentration (MIC): Lowest concentration inhibiting visible bacterial growth.
- Minimum Bactericidal Concentration (MBC): Lowest concentration killing ≥99.9% of bacteria (determined by subculturing from clear MIC tubes).
⭐ MBC is the lowest concentration of an antimicrobial that kills ≥99.9% of the initial inoculum.
- Agar Dilution:
- Antimicrobial incorporated into agar medium at various concentrations.
- MIC: Lowest concentration preventing visible colony formation.
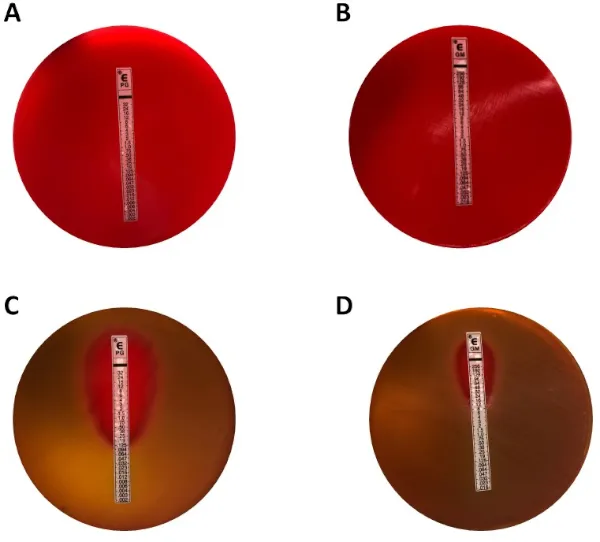
- E-test (Epsilometer test):
- Plastic strip with a predefined antimicrobial gradient on an inoculated agar plate.
- MIC: Read where the elliptical zone of inhibition intersects the calibrated strip.
Resistance & Special Tests - Superbug Sleuthing
-
MRSA: Screen: Cefoxitin disk (zone ≤ 21mm for S. aureus). Confirm: mecA gene PCR.
-
ESBLs: Screen with indicator cephalosporins (e.g., Cefotaxime, Ceftazidime). Confirm: DDST (keyhole effect) or Combination disk test (drug + Clavulanate vs. drug alone, zone diameter difference ≥ 5mm).
-
AmpC β-lactamases: Often resistant to Cefoxitin. Detection challenging; use inhibitor-based tests (e.g., with cloxacillin) or AmpC disk test.
-
Carbapenemases: Modified Carbapenem Inactivation Method (mCIM): Test isolate inactivates meropenem. Carba NP test: Color change. Hodge test (historical).
-
Inducible Clindamycin Resistance: D-test.

⭐ A positive D-test (flattening of clindamycin zone ["D" shape] adjacent to an erythromycin disk) indicates inducible erm gene-mediated resistance to clindamycin, predicting potential clinical failure despite in vitro susceptibility to clindamycin alone.
High‑Yield Points - ⚡ Biggest Takeaways
- Kirby-Bauer (disk diffusion) assesses susceptibility via zone of inhibition (ZOI) diameter.
- MIC is the lowest drug level preventing visible bacterial growth in vitro.
- MBC is the lowest drug level killing 99.9% of the initial bacterial inoculum.
- E-test uses an antibiotic gradient strip for direct MIC value determination.
- Broth dilution quantitatively determines MIC; can also find MBC.
- Interpret AST results (S, I, R) using current CLSI/EUCAST guidelines.
- Detection of MRSA, VRE, ESBLs requires specialized AST methods and criteria.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

