AST Foundations - Sizing Up The Bugs
- Purpose: Guides therapy, tracks resistance.
- MIC (Minimum Inhibitory Concentration): Lowest drug level preventing visible growth. 📌 MIC 'Inhibits'.
⭐ The MIC is the lowest concentration of an antimicrobial that prevents visible growth of a microorganism after overnight incubation.
- MBC (Minimum Bactericidal Concentration): Lowest drug level killing 99.9% of bacteria. 📌 MBC 'Kills'.
- Breakpoints (CLSI/EUCAST): Standardized values defining S/I/R categories.
| Category | Interpretation |
|---|---|
| S (Susceptible) | Therapy likely effective. |
| I (Intermediate) | Uncertain success; dose ↑ or site-specific use. |
| R (Resistant) | Therapy likely to fail. |
Diffusion & Dilution - Classic AST Tactics
1. Kirby-Bauer Disk Diffusion Test:
- Medium: Mueller-Hinton Agar (MHA).
- Inoculum: Standardized to 0.5 McFarland turbidity. 📌 'King Bauer's MHArena for 0.5 McChampions'.
- Procedure: Antibiotic-impregnated discs placed on inoculated MHA.
- Incubation: 35°C for 16-20h (aerobic, ambient air).
- Result: Measure zone of inhibition diameter (mm); interpret as Susceptible (S), Intermediate (I), or Resistant (R) using CLSI/EUCAST guidelines.

2. Dilution Methods (Determine Minimum Inhibitory Concentration - MIC):
- Broth Dilution (Microdilution & Macrodilution):
- Serial twofold dilutions of antibiotic in broth (e.g., Mueller-Hinton Broth).
- Inoculated with standardized bacterial suspension.
- MIC: Lowest antibiotic concentration showing no visible growth after incubation (35°C, 16-20h).

- Agar Dilution:
- Antibiotic incorporated into agar medium at various concentrations.
- Reference method, less common in routine labs.
⭐ Mueller-Hinton agar is the recommended medium for routine susceptibility testing of non-fastidious bacteria by the Kirby-Bauer method.
Comparison: Disk Diffusion vs. Broth Dilution
| Feature | Disk Diffusion (Kirby-Bauer) | Broth Dilution |
|---|---|---|
| Principle | Antibiotic diffusion in agar | Serial antibiotic dilution |
| Result | Zone diameter (S/I/R) | MIC (µg/mL) |
| Nature | Qualitative/Semi-quantitative | Quantitative |
| Primary Use | Routine screening | Precise MIC, research |
Gradient & Automation - Modern AST Upgrades
- E-test (Epsilometer test):
- Uses a strip with a predefined, continuous antibiotic gradient.
- Placed on an inoculated agar plate, forms an elliptical zone of inhibition.
- MIC is read directly where the inhibition ellipse edge intersects the strip.

- Automated Systems (e.g., VITEK, BD Phoenix, MicroScan):
- Principle: Turbidimetry (measures growth by ↑ turbidity) or colorimetry (detects metabolic activity via color change).
- Advantages: Rapid results (e.g., 4-18 hrs), standardization, data management, high throughput.
- Disadvantages: High cost, specific consumables, may miss certain resistance mechanisms (e.g., inducible resistance).
⭐ The E-test is particularly useful for determining MICs of fastidious organisms and for drugs not available in disk format for Kirby-Bauer.
Resistance Spotlight - Unmasking Superbugs
- Key Resistance Mechanisms & Detection:
| Resistance | Common Bugs | Screening | Confirmatory Tests |
|---|---|---|---|
| MRSA | S. aureus | Cefoxitin (≤ 21 mm S.a, ≤ 24 mm CoNS) | mecA/PBP2a detection |
| VRE | Enterococcus spp. | Vancomycin screen agar (growth at 6 µg/mL) | - |
| ESBLs | E. coli, Klebsiella | Indicator cephalosporins (e.g., CTX, CAZ) | Phenotypic: DDS, CDT + Clavulanate 📌 'ESBL needs a CLAVenger hunt' |
| AmpC β-lactamases | GNBs (Enterobacter, Serratia, Citrobacter) | Cefoxitin resistance | Inferred. (D-test for inducible clinda-R context-specific, not primary for AmpC) |
| Carbapenemases (CRE) | Klebsiella, E. coli, Acinetobacter | Ertapenem/Meropenem resistance | Phenotypic: mCIM/eCIM, Carba NP. Genotypic (KPC, NDM, OXA-48). MHT (historical). |
| Double-disk synergy test (ESBL) |
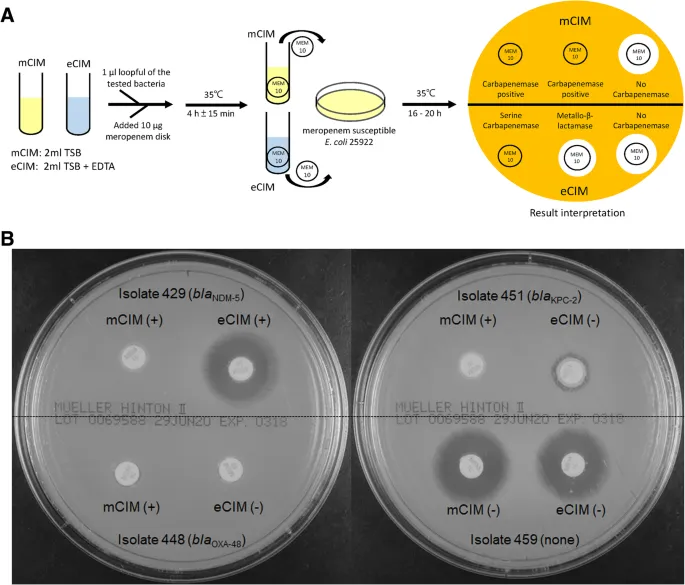 mCIM positive result (Carbapenemase)
mCIM positive result (Carbapenemase)
⭐ The presence of ESBLs is confirmed by demonstrating synergy between an indicator cephalosporin and clavulanic acid.
- Carbapenemase Detection Algorithm (Phenotypic):
High‑Yield Points - ⚡ Biggest Takeaways
- Kirby-Bauer disc diffusion measures zones of inhibition to determine susceptibility.
- MIC (Minimum Inhibitory Concentration) is the lowest antibiotic concentration preventing visible bacterial growth.
- MBC (Minimum Bactericidal Concentration) is the lowest antibiotic concentration killing 99.9% of bacteria.
- E-test (epsilometer test) determines MIC using a strip with an antibiotic gradient.
- CLSI guidelines standardize AST methods and interpretation criteria.
- Key resistance mechanisms detected include ESBLs, MRSA, and VRE.
- Automation (e.g., VITEK, MicroScan) provides rapid and standardized AST results for high-throughput labs.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

