Tularemia Basics - Rabbit Fever Rundown
- Causative Agent: Francisella tularensis
- Gram-negative coccobacillus
- Strictly aerobic
- Facultative intracellular pathogen
- Non-motile, non-spore-forming
- Requires cysteine for growth (e.g., Buffered Charcoal Yeast Extract agar - BCYE)
- Common Names: Rabbit fever, Deer-fly fever, Ohara's disease.
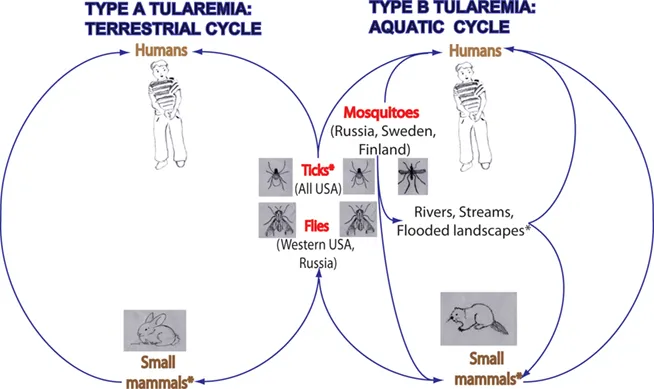
- Transmission:
- Arthropod vectors (ticks like Dermacentor, Amblyomma; deer flies like Chrysops)
- Contact with infected animal tissues (especially rabbits, hares, rodents)
- Ingestion of contaminated food/water
- Inhalation of infectious aerosols
- Key Feature: Extremely low infective dose (as few as 10-50 organisms can cause disease).
- Reservoirs: Rabbits, hares, rodents, ticks.
⭐ Francisella tularensis is a Category A bioterrorism agent due to its high infectivity, ease of aerosol dissemination, and ability to cause severe illness and mortality.
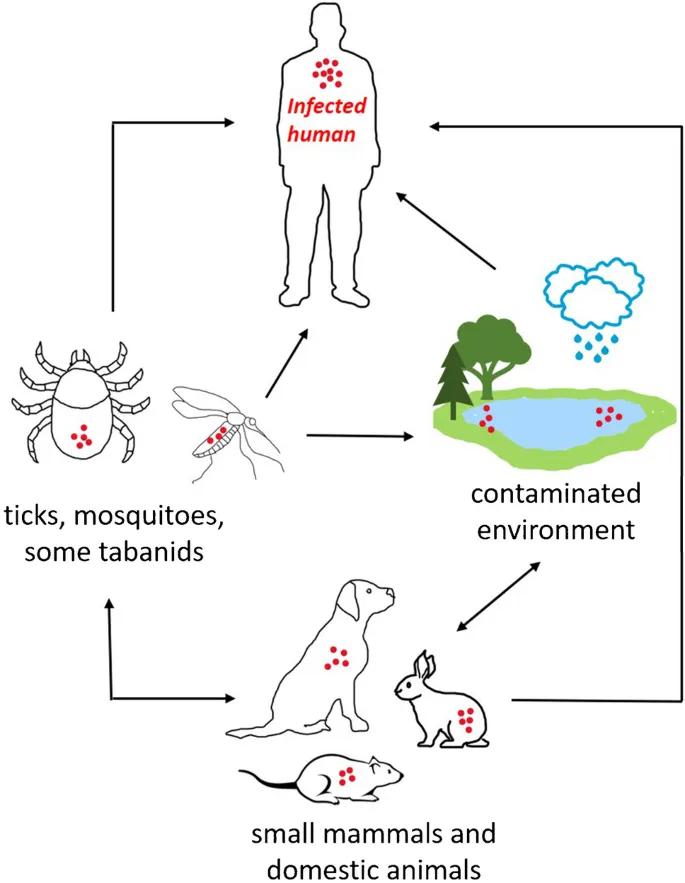
Transmission & Forms - How It Spreads & Shows
- Reservoirs: Rabbits, hares, rodents (muskrats, beavers), ticks.
- Vectors: Ticks (Dermacentor, Amblyomma), deer flies (Chrysops).
- Transmission Routes:
- Arthropod bites (most common)
- Handling infected animal tissues
- Ingestion (contaminated food/water)
- Inhalation of aerosols (F. tularensis - bioterrorism)
- Direct contact (skin/mucous membranes)
Clinical Forms:
| Form | Key Features | Portal of Entry |
|---|---|---|
| Ulceroglandular | Skin ulcer at entry + regional lymphadenopathy (75-85% cases) | Skin (bite, cut) |
| Glandular | Regional lymphadenopathy, no ulcer | Skin (bite, cut) |
| Oculoglandular | Conjunctivitis, preauricular lymphadenopathy | Eye |
| Oropharyngeal | Pharyngitis, tonsillitis, cervical lymphadenopathy | Ingestion |
| Pneumonic | Cough, dyspnea, chest pain; high mortality; primary/secondary | Inhalation, Blood |
| Typhoidal | Fever, sepsis, no clear focus; high mortality | Systemic/Blood |
Diagnosis & Management - Spotting & Stopping It
- Diagnosis:
- Culture: F. tularensis on cysteine media (BCYE, choc agar). BSL-3 lab.
- Serology: Agglutination ≥1:160, ELISA. Paired sera (4-fold rise).
- PCR: Rapid, specific. Early diagnosis from samples.
- Management:
- Drug of Choice (DOC): Streptomycin 1g IM BID or Gentamicin 5mg/kg/d for 10-14 days.
- Alternatives: Doxycycline 100mg BID or Ciprofloxacin 500-750mg BID for 14-21 days (mass casualty/mild).
- Post-Exposure Prophylaxis (PEP): Doxycycline or Ciprofloxacin for 14 days.
⭐ F. tularensis: Category A agent. Highly infectious (ID50: 10-50 organisms via aerosol); high morbidity.
Bioterrorism Threat - Weaponized Worry
- CDC Category A: highest priority bioterror agent.
- Highly infectious: low ID₅₀ (10-50 organisms); easily aerosolized.
- Causes severe morbidity; high panic potential.
- Weaponizable due to environmental persistence.
⭐ F. tularensis can remain viable for weeks in diverse environments (water, soil, carcasses), enhancing its weaponization potential.
High‑Yield Points - ⚡ Biggest Takeaways
- Agent: Francisella tularensis, a highly infectious Gram-negative coccobacillus.
- Transmission: Primarily via ticks, deer flies, and contact with infected rabbits/rodents.
- Ulceroglandular: Most common form; skin ulcer with painful lymphadenopathy.
- Pneumonic Tularemia: Key bioterrorism concern; high mortality, aerosol transmission.
- Diagnosis: Serology is mainstay; culture requires special cysteine-enriched media.
- Treatment: Streptomycin or gentamicin are drugs of choice.
- Low Infective Dose: As few as 10-50 organisms can cause infection_._
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

