Bioterrorism Agents

On this page
🦠 Bioterrorism Arsenal: The Invisible Weapons of Mass Destruction
Bioterrorism agents represent a unique intersection of infectious disease, public health emergency, and national security-pathogens deliberately weaponized to cause mass casualties and societal disruption. You'll learn to recognize the clinical signatures that distinguish intentional outbreaks from natural disease, master the rapid diagnostic and treatment protocols that save lives in the critical first hours, and understand your essential role within the coordinated public health response system. This knowledge transforms you from a passive observer of hypothetical threats into a frontline sentinel capable of detecting an attack early, protecting patients and communities, and maintaining clinical composure when it matters most.
The strategic classification system divides bioterrorism agents into three distinct categories, each representing escalating levels of threat sophistication and potential impact:
- Category A Agents - The apex predators of biological warfare
- Highest priority for national security (6 primary agents)
- Easily disseminated or transmitted person-to-person
- High mortality rates (>30% case fatality for most agents)
- Major public health impact potential
- Anthrax (Bacillus anthracis) - mortality >80% untreated inhalational
- Smallpox (Variola virus) - 30% mortality in unvaccinated populations
- Plague (Yersinia pestis) - 100% mortality untreated pneumonic form
- Botulism (Clostridium botulinum toxin) - 60% mortality untreated
- Tularemia (Francisella tularensis) - 35% mortality untreated pneumonic
- Viral hemorrhagic fevers - 50-90% mortality depending on strain
📌 Remember: SPABVT - Smallpox, Plague, Anthrax, Botulism, VHF, Tularemia represent the "Big Six" Category A agents requiring immediate recognition and response protocols
- Category B Agents - Moderately easy to disseminate
- Moderate morbidity, low mortality rates (<10% case fatality)
- Require enhanced diagnostic capacity
- Q fever (Coxiella burnetii) - <2% mortality with treatment
- Brucellosis (Brucella species) - <5% mortality untreated
- Glanders (Burkholderia mallei) - 95% mortality untreated septicemic
- Typhus fever (Rickettsia prowazekii) - 10-40% mortality untreated
⭐ Clinical Pearl: Category A agents share three critical characteristics: aerosol transmissibility, high mortality without treatment, and potential for person-to-person spread creating secondary outbreaks
The weaponization potential of biological agents depends on multiple factors that determine their effectiveness as instruments of terror. Stability in aerosol form represents the primary delivery mechanism, with particles sized 1-5 micrometers optimal for deep lung penetration and systemic infection.
| Agent Category | Mortality Rate | Incubation Period | Contagiousness | Aerosol Stability | Treatment Window |
|---|---|---|---|---|---|
| Anthrax (inhalational) | >80% untreated | 1-6 days | Non-contagious | Excellent | <24 hours post-exposure |
| Smallpox | 30% unvaccinated | 7-17 days | Highly contagious | Good | 4 days post-exposure |
| Pneumonic Plague | 100% untreated | 1-6 days | Person-to-person | Moderate | <24 hours symptom onset |
| Botulism | 60% untreated | 12-72 hours | Non-contagious | Excellent | <24 hours optimal |
| Tularemia | 35% untreated | 3-5 days | Non-contagious | Good | <48 hours symptom onset |
Environmental persistence varies dramatically among agents, influencing their strategic utility. Bacillus anthracis spores remain viable for decades in soil, while Variola virus survives only days to weeks in optimal conditions. This persistence factor determines both immediate threat duration and long-term decontamination requirements.
⚠️ Warning: Francisella tularensis requires only 10-50 organisms to cause infection via aerosol route, making it among the most infectious agents known to medicine
The syndromic approach to bioterrorism recognition focuses on pattern identification rather than specific agent diagnosis. Fever with respiratory distress in multiple patients suggests aerosol exposure, while gastrointestinal symptoms in clustered cases indicate food or water contamination. Neurological presentations with descending paralysis specifically suggest botulinum toxin exposure.
Understanding bioterrorism agents requires mastering their dual nature as both natural pathogens and weaponized threats, where enhanced virulence through genetic modification or optimized delivery systems can dramatically alter expected clinical presentations and outcomes.
🦠 Bioterrorism Arsenal: The Invisible Weapons of Mass Destruction
⚔️ Category A Agents: The Apex Biological Weapons
Anthrax (Bacillus anthracis) stands as the prototype bioweapon, with spores surviving decades in environmental conditions while maintaining full virulence. The 2001 postal attacks demonstrated its psychological impact, causing 5 deaths from only 22 cases but generating nationwide panic and $6 billion in decontamination costs.
- Inhalational Anthrax - The weaponized form
- LD50: 8,000-10,000 spores via aerosol
- Mortality: >80% without early treatment, <45% with immediate antibiotics
- Incubation: 1-6 days (range: hours to 60 days)
- Clinical phases: Prodromal (flu-like, 1-3 days) → Brief improvement → Fulminant (respiratory failure, shock)
- Widened mediastinum on chest X-ray (>90% cases)
- Hemorrhagic pleural effusions
- Rapid progression to septic shock
📌 Remember: ANTHRAX - Aerosol transmission, No person-to-person spread, Toxin-mediated pathogenesis, High mortality untreated, Radiographic widening, Antibiotic responsive early, eXtremely stable spores
Smallpox (Variola virus) represents the only eradicated human disease, making any appearance immediately suspicious for bioterrorism. Routine vaccination ceased in 1980, leaving >70% of the global population susceptible to infection.
- Variola Major - The lethal strain
- Mortality: 30% in unvaccinated populations
- Contagiousness: Person-to-person via respiratory droplets
- Incubation: 7-17 days (average 12 days)
- Infectious period: Fever onset through scab separation (3-4 weeks)
- Centrifugal rash distribution (face and extremities first)
- Synchronous lesion development (same stage simultaneously)
- Deep-seated, firm vesicles and pustules
⭐ Clinical Pearl: Smallpox vs. Chickenpox differentiation - Smallpox shows synchronous lesions all in same stage, centrifugal distribution, and deep-seated pustules, while chickenpox displays asynchronous lesions in multiple stages with centripetal distribution
Plague (Yersinia pestis) transforms from endemic flea-borne disease to bioweapon through aerosol delivery, creating pneumonic plague with 100% mortality if untreated beyond 24 hours.
| Plague Form | Transmission | Mortality Untreated | Mortality Treated | Contagious Period |
|---|---|---|---|---|
| Bubonic | Flea bite | 60% | <5% | Non-contagious |
| Septicemic | Flea bite/progression | 100% | <15% | Non-contagious |
| Pneumonic | Aerosol/droplet | 100% | <15% | Highly contagious |
| Pharyngeal | Ingestion | 100% | <10% | Moderately contagious |
| Meningeal | Hematogenous spread | 100% | <25% | Non-contagious |
Botulinum toxin represents the most potent biological toxin known, with an LD50 of 1-3 nanograms per kilogram body weight. Type A toxin remains the primary bioweapon concern due to its stability and prolonged paralysis lasting 2-6 months.
- Clinical Presentation - Descending flaccid paralysis
- Cranial nerves first: Diplopia, dysarthria, dysphagia (4 D's)
- Respiratory muscles: Diaphragmatic paralysis within 24-72 hours
- Peripheral muscles: Symmetric, descending weakness
- Autonomic effects: Dry mouth, constipation, urinary retention
- No fever or altered mental status
- Normal sensation throughout
- Reflexes preserved initially
⚠️ Warning: Foodborne botulism typically affects 2-8 people from shared source, while bioterrorism would present as multiple simultaneous cases without common food exposure
Tularemia (Francisella tularensis) requires only 10-50 organisms for infection, making it extremely suitable for bioweapon development. Type A strains found in North America show higher virulence than Type B European strains.
- Pneumonic Tularemia - Bioweapon presentation
- Mortality: 35% untreated, <2% with appropriate antibiotics
- Incubation: 3-5 days (range 1-14 days)
- Clinical features: Acute pneumonia with systemic toxicity
- High fever (>39°C) with rigors
- Nonproductive cough progressing to purulent sputum
- Pleuritic chest pain and dyspnea
- Hilar lymphadenopathy on chest imaging
Viral Hemorrhagic Fevers (VHFs) encompass multiple virus families with case fatality rates ranging from 25-90% depending on specific agent and strain.
- Filoviruses (Ebola, Marburg) - 50-90% mortality
- Arenaviruses (Lassa, Argentine HF) - 15-30% mortality
- Bunyaviruses (Rift Valley fever, CCHF) - 30-50% mortality
- Flaviviruses (Yellow fever) - 20-50% mortality
Understanding Category A agents requires recognizing their engineered potential for mass destruction while maintaining clinical focus on early recognition patterns that enable life-saving interventions.
⚔️ Category A Agents: The Apex Biological Weapons
🎯 Recognition Patterns: Bioterrorism Clinical Signatures
Temporal Clustering represents the most reliable indicator of bioterrorism. Natural outbreaks typically show gradual onset over weeks to months, while bioweapon attacks create sharp epidemic curves with multiple simultaneous cases presenting within 24-72 hours.
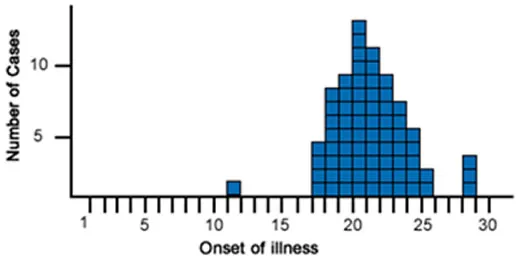
-
Natural Outbreak Characteristics
- Gradual increase in cases over 2-4 weeks
- Geographic spread following transportation routes
- Age-specific attack rates based on immunity patterns
- Seasonal variation consistent with pathogen ecology
- Point source: Single exposure with bell-shaped curve
- Propagated: Person-to-person with successive waves
- Continuous: Ongoing exposure with plateau pattern
-
Bioterrorism Attack Patterns
- Explosive onset with peak within 24-48 hours
- Geographic clustering around target locations
- Random age distribution affecting all demographics
- No seasonal pattern or environmental correlation
- Multiple simultaneous outbreaks in distant locations
- Unusual disease in unexpected geographic area
- Higher attack rates in indoor locations
📌 Remember: BIOTERROR - Bizarre epidemiology, Indoor clustering, Outbreak explosive, Temporal compression, Everyone affected equally, Rare disease appearing, Respiratory predominance, Odd geographic distribution, Rapid progression
Syndromic Surveillance focuses on symptom patterns rather than specific diagnoses, enabling earlier detection before laboratory confirmation. Emergency department chief complaints provide real-time monitoring of potential bioterrorism events.
| Syndrome | Key Features | Bioterrorism Agents | Timeline to Recognition |
|---|---|---|---|
| Respiratory | Fever + cough + dyspnea | Anthrax, Plague, Tularemia | 24-48 hours |
| Neurological | Descending paralysis | Botulism | 12-24 hours |
| Hemorrhagic | Fever + bleeding | VHFs | 48-72 hours |
| Vesicular | Fever + rash | Smallpox | 7-14 days |
| Gastrointestinal | Nausea + vomiting + diarrhea | Multiple agents | 6-24 hours |
Inhalational Anthrax Recognition requires distinguishing it from common respiratory infections. The biphasic presentation with initial improvement followed by rapid deterioration provides a critical diagnostic clue.
-
Phase 1 (Prodromal) - 1-3 days
- Flu-like symptoms: Fever, malaise, myalgia
- Mild respiratory symptoms: Dry cough, chest discomfort
- No rhinorrhea or sore throat (unlike influenza)
- Patients feel well enough to continue activities
- Fever: 38-40°C (100-104°F)
- Fatigue: Profound but non-specific
- Chest discomfort: Substernal pressure
-
Phase 2 (Fulminant) - 24-48 hours
- Sudden deterioration after brief improvement
- Severe respiratory distress and shock
- Widened mediastinum on chest X-ray (>90% cases)
- Hemorrhagic pleural effusions
- Stridor: Due to hemorrhagic mediastinitis
- Cyanosis: Rapid onset with respiratory failure
- Hypotension: Shock within hours
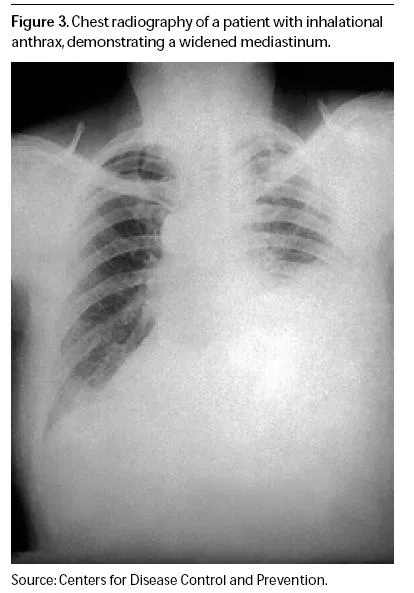
💡 Master This: Inhalational anthrax shows widened mediastinum in >90% of cases - any flu-like illness with mediastinal widening in multiple patients requires immediate bioterrorism response
Smallpox Recognition depends on rash characteristics that distinguish it from chickenpox and other vesicular diseases. The centrifugal distribution and synchronous development provide pathognomonic features.
-
Smallpox Rash Progression
- Day 1-2: Enanthem (oral lesions) appears first
- Day 3: Skin rash begins on face and forearms
- Day 4-5: Centrifugal spread to trunk and legs
- Day 6-8: Vesicles become deep pustules
- Synchronous lesions: All in same stage simultaneously
- Deep-seated: Firm, round, well-circumscribed
- Palms and soles: Involved in >90% cases
- Centrifugal: Higher density on face and extremities
-
Differential Diagnosis Clues
- Chickenpox: Asynchronous lesions, centripetal distribution, superficial vesicles
- Monkeypox: Lymphadenopathy prominent, slower progression
- Drug eruption: No fever, different distribution
- Hand-foot-mouth: Limited distribution, different morphology
Pneumonic Plague Recognition focuses on rapid progression from flu-like symptoms to respiratory failure within 24-48 hours. The absence of buboes in primary pneumonic plague distinguishes it from bubonic forms.
- Clinical Progression
- Hours 0-12: Sudden onset fever, chills, headache
- Hours 12-24: Cough develops, initially nonproductive
- Hours 24-36: Purulent sputum, often blood-tinged
- Hours 36-48: Respiratory failure and shock
- Hemoptysis: Bright red or rust-colored sputum
- Chest pain: Pleuritic with respiratory distress
- No buboes: In primary pneumonic form
- Rapid progression: Death within 2-4 days untreated
⚠️ Warning: Pneumonic plague patients become highly contagious within 24 hours of symptom onset, requiring immediate respiratory isolation and contact tracing for all exposed individuals
Understanding bioterrorism recognition patterns enables healthcare providers to serve as the critical first detectors in the public health surveillance system, where early identification saves lives and prevents widespread casualties.
🎯 Recognition Patterns: Bioterrorism Clinical Signatures
🔬 Laboratory Diagnostics: Rapid Threat Identification
LRN Laboratory Levels create a hierarchical system ensuring appropriate testing capabilities while maintaining biosafety standards:
-
Sentinel Laboratories (>25,000 facilities)
- Rule-out testing using standard protocols
- Rapid referral of suspicious specimens
- Basic biosafety (BSL-2) capabilities
- No specialized bioterrorism testing
- Clinical laboratories in hospitals
- Commercial reference laboratories
- Public health laboratories (local level)
-
Reference Laboratories (>150 facilities)
- Confirmatory testing for Category A agents
- Advanced biosafety (BSL-3) capabilities
- Rapid turnaround (<4 hours for critical agents)
- 24/7 response capability
- State public health laboratories
- Selected federal laboratories
- Military laboratories
-
National Laboratories (<10 facilities)
- Definitive identification and characterization
- Highest biosafety (BSL-4) for select agents
- Forensic analysis capabilities
- Strain typing and antimicrobial susceptibility
- CDC laboratories
- USAMRIID (US Army Medical Research Institute)
- Selected academic centers
Rapid Diagnostic Methods prioritize speed over specificity for initial screening, with results available within 2-4 hours to guide immediate clinical decisions.
| Agent | Rapid Test | Sensitivity | Specificity | Time to Result | Confirmatory Method |
|---|---|---|---|---|---|
| Anthrax | Immunochromatography | >95% | >98% | <30 minutes | PCR + Culture |
| Plague | F1 antigen test | >90% | >95% | <15 minutes | PCR + Culture |
| Smallpox | Electron microscopy | >99% | >99% | <2 hours | PCR + Sequencing |
| Botulism | Mouse bioassay | >95% | 100% | 24-48 hours | ELISA + PCR |
| Tularemia | Antigen detection | >85% | >90% | <1 hour | PCR + Culture |
Anthrax Diagnostics utilize multiple specimen types depending on clinical presentation and disease stage. Blood cultures remain positive in >90% of cases during bacteremic phase.
-
Specimen Collection Priority
- Blood cultures: 2-3 sets before antibiotic therapy
- Pleural fluid: If effusion present (>90% cases)
- Sputum: Gram stain and culture
- Nasal swabs: Environmental exposure assessment only
- CSF: If meningeal signs present (5% cases)
- Stool: For gastrointestinal anthrax
- Skin lesions: Vesicle fluid and tissue biopsy
-
Laboratory Findings
- Gram-positive bacilli in chains (bamboo rod appearance)
- Non-motile, spore-forming under appropriate conditions
- Hemolytic on blood agar with ground glass appearance
- Penicillin sensitive (distinguishes from B. cereus)
- PCR: Protective antigen and lethal factor genes
- Antigen detection: Cell wall polysaccharide
- Toxin assays: Edema factor and lethal factor
⭐ Clinical Pearl: Anthrax blood cultures turn positive within 6-24 hours in >90% of inhalational cases, making blood culture the highest yield rapid diagnostic test
Smallpox Diagnostics require BSL-4 containment for live virus work, with electron microscopy providing rapid presumptive identification within 2 hours.
-
Specimen Collection
- Vesicle fluid: Optimal specimen during vesicular stage
- Scab material: Later stages of illness
- Throat swabs: Early viremia detection
- Blood: PCR during febrile prodrome
- Timing critical: Highest viral loads during first week
- Multiple sites: Different lesion stages if present
- Proper transport: Viral transport medium at 4°C
-
Diagnostic Methods
- Electron microscopy: Brick-shaped virions with surface tubules
- PCR: Species-specific primers for variola virus
- Antigen detection: Orthopoxvirus group-specific
- Sequencing: Definitive species identification
- Sensitivity: PCR >99%, EM >95%, Antigen >90%
- Turnaround: EM <2 hours, PCR <4 hours, Sequencing <24 hours
Plague Diagnostics emphasize rapid identification due to 24-hour treatment window for optimal outcomes. F1 antigen detection provides field-deployable testing capability.
-
Specimen Types by Clinical Form
- Pneumonic: Sputum, blood cultures, pleural fluid
- Bubonic: Bubo aspirate, blood cultures
- Septicemic: Blood cultures (multiple sets)
- Pharyngeal: Throat swabs, blood cultures
- Timing: Before antibiotic administration when possible
- Volume: Large volumes increase yield
- Transport: Standard bacterial transport media
-
Laboratory Characteristics
- Gram-negative coccobacilli with bipolar staining
- Non-motile at 37°C, motile at 22°C
- Catalase positive, oxidase negative
- Growth: 48-72 hours on blood agar
- F1 antigen: Rapid immunochromatography (<15 minutes)
- PCR: Multiple gene targets for confirmation
- Phage lysis: Species confirmation method
💡 Master This: Plague diagnosis requires immediate processing - F1 antigen testing provides results within 15 minutes with >90% sensitivity, enabling rapid treatment decisions before 24-hour window closes
Botulism Diagnostics rely on toxin detection rather than organism identification, with mouse bioassay remaining the gold standard despite 24-48 hour turnaround time.
- Specimen Collection Strategy
- Serum: Toxin detection during acute phase
- Stool: Organism and toxin detection
- Gastric contents: Early presentation (<24 hours)
- Food samples: Environmental source identification
- Timing: Earlier collection increases yield
- Volume: Large specimens improve sensitivity
- Storage: Refrigerated transport, avoid freezing
Understanding bioterrorism laboratory diagnostics enables healthcare providers to optimize specimen collection and interpretation while coordinating with public health authorities for appropriate response escalation.
🔬 Laboratory Diagnostics: Rapid Threat Identification
⚕️ Clinical Management: Life-Saving Interventions
Anthrax Management focuses on early antibiotic therapy and supportive care for systemic toxicity. Post-exposure prophylaxis requires 60-day antibiotic courses due to spore persistence in lung tissue.
-
Inhalational Anthrax Treatment
- First-line therapy: Ciprofloxacin 400mg IV q12h + Clindamycin 900mg IV q8h
- Alternative: Doxycycline 100mg IV q12h + Rifampin 300mg PO q12h
- Duration: 60 days total (IV → PO when stable)
- Adjunctive: Antitoxin therapy if available
- Pediatric dosing: Ciprofloxacin 10-15mg/kg q12h
- Pregnancy: Ciprofloxacin preferred over doxycycline
- Resistance: Penicillin resistance possible in engineered strains
-
Post-Exposure Prophylaxis (PEP)
- Ciprofloxacin 500mg PO q12h × 60 days
- Doxycycline 100mg PO q12h × 60 days
- Amoxicillin 500mg PO q8h × 60 days (if susceptible)
- Vaccination: 3 doses at 0, 2, 4 weeks if available
- Mass prophylaxis: >10,000 people may require PEP
- Compliance: 60-day regimen shows <50% completion
- Monitoring: Weekly clinical assessment recommended
📌 Remember: ANTHRAX Rx - Antibiotics early (IV combo), Never delay for culture, Toxin therapy if available, High-dose long-duration, Resistance possible, Adjunctive supportive care, eXtended prophylaxis (60 days)
Smallpox Management emphasizes supportive care and infection control, as no specific antiviral therapy has proven efficacy. Vaccination within 4 days of exposure provides >90% protection.
| Intervention | Timing | Efficacy | Duration | Special Considerations |
|---|---|---|---|---|
| Vaccination | <24 hours post-exposure | >95% protection | Lifelong immunity | Contraindicated in immunocompromised |
| Vaccination | 1-3 days post-exposure | >90% protection | Lifelong immunity | Modified disease possible |
| Vaccination | 4-7 days post-exposure | >50% protection | Variable immunity | May modify severity |
| Cidofovir | Any time | Unproven efficacy | Variable | Experimental use only |
| VIG | Complications | Limited benefit | Temporary | Severe adverse events |
- Fluid management: Capillary leak and third-spacing
- Pain control: Severe pain from skin lesions
- Secondary infection: Bacterial superinfection prevention
- Nutrition: Oral lesions impair feeding
- Isolation: Airborne and contact precautions
- Eye care: Corneal involvement in >10% cases
- Psychological: Disfigurement and mortality fears
⭐ Clinical Pearl: Smallpox vaccination provides maximum benefit when administered within 24 hours of exposure, but partial protection occurs up to 4 days post-exposure, making rapid contact tracing critical
Plague Management requires immediate antibiotic therapy within 24 hours of symptom onset to prevent mortality >90%. Respiratory isolation prevents person-to-person transmission.
-
Pneumonic Plague Treatment
- First-line: Streptomycin 1g IM q12h × 10 days
- Alternative: Gentamicin 5mg/kg IV q24h × 10 days
- Oral option: Doxycycline 100mg PO q12h × 10 days
- Severe cases: Chloramphenicol for meningeal involvement
- Pediatric: Gentamicin 2.5mg/kg q8h
- Pregnancy: Gentamicin preferred
- Duration: Minimum 10 days or 3 days after fever resolution
-
Post-Exposure Prophylaxis
- Doxycycline 100mg PO q12h × 7 days
- Ciprofloxacin 500mg PO q12h × 7 days
- Close contacts: Face-to-face within 2 meters
- Healthcare workers: Unprotected exposure to respiratory secretions
- Monitoring: Daily temperature checks × 7 days
- Isolation: Until 48 hours of effective therapy
- Compliance: >95% completion rates with 7-day regimens
Botulism Management focuses on supportive care and antitoxin administration, with mechanical ventilation required in >60% of cases due to respiratory paralysis.
-
Antitoxin Therapy
- HBAT (Heptavalent Botulism Antitoxin): 1 vial IV (covers types A-G)
- Timing: Maximum benefit within 24 hours of symptom onset
- Efficacy: Reduces mortality from 60% to <5%
- Duration: Single dose usually sufficient
- Pediatric: BIG-IV (Botulism Immune Globulin) for <1 year
- Allergic reactions: <1% with HBAT
- Availability: CDC Strategic National Stockpile
-
Respiratory Support
- Mechanical ventilation: >60% of severe cases
- Duration: Weeks to months for recovery
- Weaning: Gradual as nerve terminals regenerate
- Complications: Ventilator-associated pneumonia, DVT
- Monitoring: Vital capacity and negative inspiratory force
- Tracheostomy: Early consideration for prolonged ventilation
- Rehabilitation: Physical therapy during recovery
💡 Master This: Botulism recovery requires 2-6 months for complete neurological recovery as nerve terminals regenerate, making long-term supportive care and rehabilitation essential components of management
Tularemia Management responds well to appropriate antibiotics with mortality <2% when treated promptly, compared to 35% mortality if untreated.
- Pneumonic Tularemia Treatment
- First-line: Streptomycin 1g IM q12h × 10 days
- Alternative: Gentamicin 5mg/kg IV q24h × 10 days
- Oral therapy: Doxycycline 100mg PO q12h × 14-21 days
- Severe cases: Chloramphenicol if CNS involvement
- Relapse rates: Higher with bacteriostatic antibiotics
- Duration: Longer courses (14-21 days) reduce relapse
- Monitoring: Clinical response within 48-72 hours
Understanding bioterrorism clinical management enables healthcare providers to deliver life-saving interventions while coordinating with public health authorities for comprehensive outbreak response and community protection.
⚕️ Clinical Management: Life-Saving Interventions
🛡️ Public Health Response: Coordinated Defense Systems
Strategic National Stockpile (SNS) maintains emergency supplies sufficient to protect millions of Americans during bioterrorism events. 12-hour deployment capability ensures rapid availability of antibiotics, vaccines, and medical supplies.
-
SNS Components
- Push Packages: 12-hour deployment anywhere in US
- Vendor Managed Inventory: 24-48 hour specialized supplies
- CHEMPACK: Nerve agent antidotes pre-positioned
- Pediatric supplies: Age-appropriate formulations
- 50-ton packages: Sufficient for >500,000 people
- Multiple locations: Geographically distributed warehouses
- Transportation: Military and commercial aircraft
- Security: Armed escorts during transport
-
Mass Prophylaxis Operations
- Dispensing sites: >1,000 people per hour capacity
- Points of Distribution (PODs): Community-based locations
- Closed PODs: Workplace and school-based distribution
- Special populations: Homebound, institutionalized individuals
- Staffing: >100 personnel per large POD
- Throughput: Target 1,000+ people per POD per hour
- Duration: Operate 12+ hours daily for multiple days
📌 Remember: SNS DEPLOY - Strategic stockpile, National coordination, Supplies pre-positioned, Deployment 12-hour, Emergency distribution, Push packages ready, Local POD setup, Operations sustained, Year-round maintenance
Surveillance Systems provide early warning capabilities through syndromic monitoring and laboratory networks. BioSense and ESSENCE systems monitor emergency department visits for unusual patterns.
| Surveillance System | Data Source | Detection Time | Coverage | Sensitivity |
|---|---|---|---|---|
| BioSense | ED visits, lab orders | <24 hours | >4,000 facilities | >85% |
| ESSENCE | Military facilities | <12 hours | >300 sites | >90% |
| LRN | Laboratory results | <4 hours | >150 labs | >95% |
| NEDSS | Reportable diseases | <24 hours | All states | >80% |
| PulseNet | Foodborne pathogens | <48 hours | >80 labs | >90% |
- Respiratory syndrome: >20 cases in 24 hours
- Neurological syndrome: >5 cases with paralysis
- Hemorrhagic syndrome: >10 cases with bleeding
- Vesicular syndrome: >3 cases with rash
- Geographic clustering: Same zip code or facility
- Temporal clustering: Onset within 48 hours
- Demographic patterns: All age groups affected
- Severity: Higher hospitalization rates
⭐ Clinical Pearl: Syndromic surveillance detects bioterrorism events an average of 2-4 days earlier than traditional disease reporting, providing critical early warning for response activation
Quarantine and Isolation measures protect communities while balancing individual rights with public safety. Legal authorities vary by jurisdiction and disease characteristics.
-
Isolation (Sick individuals)
- Smallpox: Airborne and contact precautions
- Pneumonic plague: Droplet precautions × 48 hours of therapy
- VHF: Contact precautions with enhanced PPE
- Anthrax: No isolation required (not contagious)
- Duration: Until non-infectious or disease ruled out
- Location: Hospital, home, or designated facility
- Monitoring: Daily clinical assessment
- Support: Medical care, food, psychological services
-
Quarantine (Exposed individuals)
- Smallpox contacts: 17-day monitoring period
- Plague contacts: 7-day monitoring with prophylaxis
- VHF contacts: 21-day monitoring period
- Mass quarantine: Rarely indicated or effective
- Legal basis: State police powers and federal authority
- Enforcement: Voluntary compliance preferred
- Essential services: Healthcare workers, utilities, food
- Economic impact: Billions in lost productivity
Risk Communication maintains public trust and compliance during high-stress situations. Clear, consistent, and frequent messaging prevents panic and misinformation.
-
Communication Principles
- Transparency: Acknowledge uncertainties honestly
- Timeliness: Regular updates every 2-4 hours
- Accuracy: Fact-based information only
- Empathy: Acknowledge fears and concerns
- Multiple channels: Media, websites, social media
- Language: Appropriate literacy levels (6th grade)
- Cultural competence: Multilingual materials
- Spokesperson: Consistent and credible individual
-
Message Content
- What happened: Basic facts without speculation
- Health risks: Specific to exposed populations
- Protective actions: Clear instructions for public
- Resources: Where to get help and information
- Avoid: Technical jargon, conflicting information
- Emphasize: Effective treatments available
- Update: As situation evolves
- Counter: Rumors and misinformation quickly
Decontamination Operations remove biological agents from people, equipment, and environments. Personal decontamination takes priority over environmental cleanup.
-
Personal Decontamination
- Soap and water: Effective for most agents
- 0.5% hypochlorite: Anthrax spores and VHF
- Clothing removal: Removes >90% of contamination
- Eye irrigation: Copious saline for 15+ minutes
- Timing: Immediate after exposure recognition
- Location: Outdoor or well-ventilated areas
- Privacy: Maintain dignity during disrobing
- Medical: Treat injuries before decontamination
-
Environmental Decontamination
- Anthrax spores: Chlorine dioxide gas or VHP
- Vegetative bacteria: Standard disinfectants
- Viruses: Bleach solutions (1:10 dilution)
- Large areas: May require months to years
- Cost: Billions for large-scale cleanup
- Verification: Environmental sampling required
- Re-entry: Only after clearance testing
- Waste: Hazardous disposal requirements
💡 Master This: Effective public health response requires seamless coordination between clinical care, laboratory diagnostics, epidemiological investigation, and community protection measures, with success measured in lives saved rather than resources expended
Understanding public health response systems enables healthcare providers to function effectively within the broader emergency management framework while maintaining focus on individual patient care during bioterrorism events.
🛡️ Public Health Response: Coordinated Defense Systems
🎯 Biodefense Mastery: Your Clinical Command Arsenal
Essential Recognition Matrix - 30-Second Assessment Tool
| Agent | Key Clue | Timeline | Mortality Untreated | Treatment Window | Contagious |
|---|---|---|---|---|---|
| Anthrax | Widened mediastinum | 1-6 days | >80% | <24 hours | No |
| Smallpox | Centrifugal rash | 7-17 days | 30% | <4 days PEP | Yes |
| Plague | Hemoptysis + shock | 1-6 days | 100% | <24 hours | Yes |
| Botulism | Descending paralysis | 12-72 hours | 60% | <24 hours | No |
| Tularemia | Pneumonia + toxicity | 3-5 days | 35% | <48 hours | No |
| VHF | Fever + bleeding | 2-21 days | 50-90% | <72 hours | Variable |
Critical Drug Dosing - Emergency Reference
-
Anthrax Treatment
- Adult: Ciprofloxacin 400mg IV q12h + Clindamycin 900mg IV q8h
- Pediatric: Ciprofloxacin 10-15mg/kg IV q12h (max 400mg)
- Pregnancy: Ciprofloxacin preferred over doxycycline
- PEP: Ciprofloxacin 500mg PO q12h × 60 days
-
Plague Treatment
- Adult: Streptomycin 1g IM q12h or Gentamicin 5mg/kg IV q24h
- Pediatric: Gentamicin 2.5mg/kg IV q8h
- PEP: Doxycycline 100mg PO q12h × 7 days
-
Botulism Treatment
- HBAT: 1 vial IV (contact CDC immediately)
- Pediatric <1 year: BIG-IV (Botulism Immune Globulin)
⭐ Clinical Pearl: "When in doubt, treat" - Empirical therapy for suspected bioterrorism saves more lives than waiting for confirmation, especially for anthrax and plague with <24-hour treatment windows
Isolation Precautions - Immediate Implementation

-
Airborne Precautions (Smallpox)
- Negative pressure room (>12 air changes/hour)
- N95 respirator minimum (PAPR preferred)
- Door closed at all times
- Limit visitors and healthcare workers
-
Droplet Precautions (Pneumonic Plague × 48 hours)
- Surgical mask for patient and staff
- Private room (negative pressure not required)
- 3-foot separation from other patients
- Continue until 48 hours effective therapy
-
Contact Precautions (VHF)
- Gown and gloves for all contact
- Enhanced PPE for high-risk procedures
- Dedicated equipment when possible
- Environmental cleaning with appropriate disinfectants
Specimen Collection Priorities - Maximum Yield Strategy
-
Before Antibiotics (when possible)
- Blood cultures (2-3 sets) for anthrax, plague, tularemia
- Respiratory specimens for pneumonic forms
- Vesicle fluid for smallpox (if vesicular stage)
-
After Treatment Started
- Serum for toxin detection (botulism)
- Stool for organism recovery (botulism)
- Throat swabs for smallpox (early stages)
💡 Master This: Bioterrorism response success depends on simultaneous execution of clinical care, infection control, laboratory coordination, and public health notification - no single intervention alone prevents mass casualties
Emergency Contact Network - 24/7 Activation
-
Immediate Notifications (<30 minutes)
- Hospital infection control and administration
- Local health department (reportable diseases)
- Hospital laboratory (specimen processing)
- Emergency management (if multiple cases)
-
Rapid Escalation (<2 hours)
- State health department (Category A agents)
- CDC Emergency Operations (1-770-488-7100)
- FBI (if suspected intentional)
- Local emergency management (resource coordination)
Mass Casualty Triage - Bioterrorism Modifications
-
Immediate (Red)
- Treatable within therapeutic window
- High survival probability with intervention
- Examples: Early anthrax, plague with <24h symptoms
-
Delayed (Yellow)
- Stable or outside therapeutic window
- Supportive care beneficial
- Examples: Late-stage disease, mild symptoms
-
Expectant (Black)
- Beyond therapeutic window with poor prognosis
- Comfort care only
- Examples: Untreated plague >48h, advanced VHF
Understanding bioterrorism mastery tools enables healthcare providers to respond effectively during high-stress situations while maintaining clinical excellence and coordinating seamlessly with public health authorities for optimal patient and community outcomes.
🎯 Biodefense Mastery: Your Clinical Command Arsenal
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more
Have doubts about this lesson?
Ask Rezzy, your AI Study Mate, to explain anything you didn't understand
Everything you need for NEET-PG prep
Get full Oncourse access with lessons, practice questions, flashcards and AI study tools.
Scan to download app
























