PID: Definition & Etiology - PID's Pesky Pathogens
- Definition: A spectrum of inflammatory disorders of the upper female genital tract, including endometritis, salpingitis, oophoritis, tubo-ovarian abscess, and pelvic peritonitis.
- Common Causative Organisms:
- N. gonorrhoeae, C. trachomatis (📌 Go Chlamydia!)
- Polymicrobial: Anaerobes, Mycoplasma genitalium
- Key Risk Factors:
- Multiple sexual partners, young age (<25 yrs)
- Previous PID, recent IUCD insertion
- Douching, history of STIs
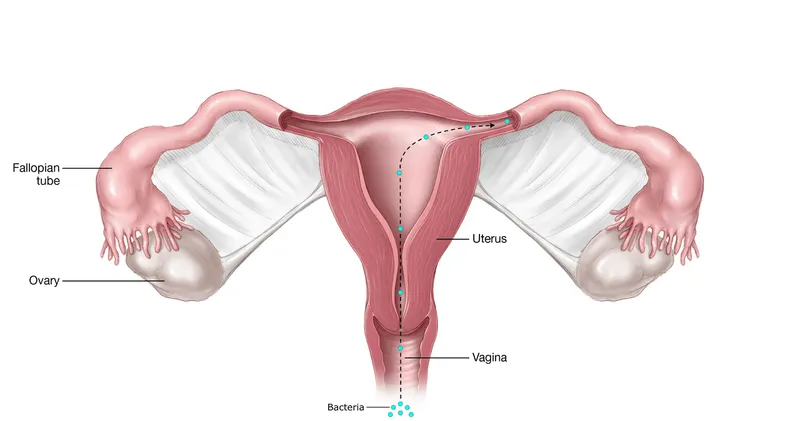
⭐ Polymicrobial infection is common in PID, often involving N. gonorrhoeae, C. trachomatis, and anaerobes.
PID: Clinical Features - PID's Painful Profile
- Common Symptoms:
- Lower abdominal/pelvic pain (often bilateral)
- Abnormal vaginal discharge (e.g., mucopurulent)
- Intermenstrual or postcoital bleeding
- Dyspareunia
- Fever
- Key Signs:
- Cervical motion tenderness (CMT) - "Chandelier sign"
- Adnexal tenderness (usually bilateral)
- Uterine tenderness
- Fever >38.3°C
- Clinical Spectrum: Can range from asymptomatic/subclinical to severe, acute PID.
⭐ Cervical motion tenderness (CMT), also known as the 'Chandelier sign', is a classic sign of PID but not universally present.
PID: Diagnosis - PID's Clue Hunt
- CDC Minimum Criteria (≥1 for Dx):
- Cervical Motion Tenderness (CMT)
- Uterine tenderness
- Adnexal tenderness
- (Sexually active young women, pelvic pain, no other cause)
- Additional Criteria (↑ specificity):
- Fever >38.3°C; Abnormal discharge
- ↑ WBCs (wet mount); ↑ ESR/CRP
- Positive GC/CT NAAT
- Definitive: Endometrial biopsy; TVS/MRI (thick tubes); Laparoscopy.
- Investigations: hCG test, GC/CT NAATs, Wet mount, ESR/CRP, USG (for TOA).
⭐ Initiate empirical PID treatment in sexually active young women with pelvic/lower abdominal pain if no other cause is found AND ≥1 minimum clinical criteria (CMT, uterine/adnexal tenderness) present on pelvic exam.
PID: Management - PID's Treatment Triumph
Goals: Eradicate infection, relieve symptoms, prevent sequelae.
Hospitalize if: Surgical emergency, pregnancy, severe illness/TOA, oral intolerance, outpatient failure.
Treatment Regimens (CDC):
| Type | Regimens |
|---|---|
| Outpatient | Ceftriaxone 500mg IM (or 1g if >150kg) ONCE + Doxycycline 100mg PO BID x14d ± Metronidazole 500mg PO BID x14d. |
| Inpatient | Cefotetan 2g IV q12h OR Cefoxitin 2g IV q6h, PLUS Doxycycline 100mg PO/IV q12h. Alt: Clindamycin 900mg IV q8h PLUS Gentamicin (LD 2mg/kg, MD 1.5mg/kg) q8h. |
- Notify & treat all sexual partners (within past 60 days).
- Abstain from intercourse until therapy completed & symptoms resolved.
⭐ All sexual partners of a patient with PID from the preceding 60 days should be evaluated, tested, and presumptively treated for chlamydia and gonorrhea, regardless of test results.
PID: Complications - PID's Lingering Legacy
- Short-term:
- Tubo-ovarian abscess (TOA)
- Fitz-Hugh-Curtis syndrome (perihepatitis; RUQ pain, 'violin-string' adhesions)
- Sepsis
- Long-term:
- Infertility (tubal; risk ↑ with episodes)
- Ectopic pregnancy (risk ↑ 6-10 fold)
- Chronic pelvic pain, dyspareunia
- Hydrosalpinx
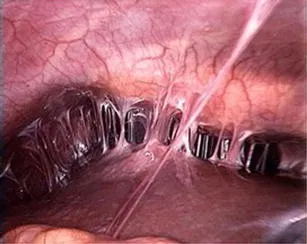
⭐ Fitz-Hugh-Curtis syndrome, characterized by perihepatitis and 'violin-string' adhesions between the liver capsule and peritoneum, is a known complication of PID, typically caused by C. trachomatis or N. gonorrhoeae.
High‑Yield Points - ⚡ Biggest Takeaways
- PID is most commonly caused by Chlamydia trachomatis & N. gonorrhoeae.
- Key diagnostic signs: Cervical motion tenderness (CMT), uterine, or adnexal tenderness.
- Laparoscopy is gold standard for diagnosis, but clinical criteria are usually sufficient.
- Standard outpatient treatment: Ceftriaxone IM + Doxycycline oral ± Metronidazole oral.
- Fitz-Hugh-Curtis syndrome: Perihepatitis (violin-string adhesions) is a specific complication.
- Major sequelae include infertility, ectopic pregnancy, and chronic pelvic pain.
- Tubo-ovarian abscess (TOA) is a serious complication requiring prompt management_._
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

