SLE Introduction & Pathophysiology - The Immune Betrayal
- Definition: Chronic, multisystem autoimmune inflammatory disease.
- Epidemiology: F:M ratio ~9:1; peak onset 15-45 years.
- Predisposition: Genetic (HLA-DR2, HLA-DR3), environmental triggers (UV, drugs, infections).
- Pathophysiology: Autoimmunity due to loss of self-tolerance.
- Autoantibody production: ANA (screening), anti-dsDNA & anti-Sm (specific).
- Immune complex deposition (Type III hypersensitivity) & Type II cytotoxic reactions.
- Complement activation leading to tissue inflammation & damage.
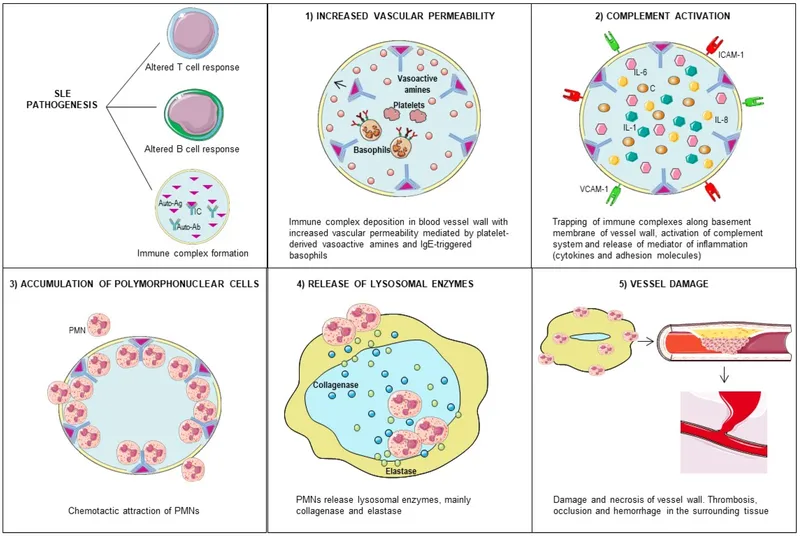
⭐ SLE is characterized by the loss of self-tolerance and production of autoantibodies against nuclear antigens.
SLE Clinical Spectrum - Rash to Renal
- Constitutional: Fever, fatigue, weight loss.
- Mucocutaneous:
- Malar rash (spares nasolabial folds).
- Discoid lupus.
- Photosensitivity.
- Oral ulcers (painless).
- Alopecia (non-scarring).
- Musculoskeletal: Non-erosive arthritis (Jaccoud's arthropathy), arthralgia, myalgia.
- Serositis: Pleuritis, pericarditis.
- Hematological: Anemia (of chronic disease, hemolytic), leukopenia, lymphopenia, thrombocytopenia.
- Renal (Lupus Nephritis): Proteinuria, hematuria. Classes I-VI (biopsy-based).
- Class I: Minimal mesangial LN
- Class II: Mesangial proliferative LN
- Class III: Focal LN (<50% glomeruli)
- Class IV: Diffuse LN (>50% glomeruli) - most common & severe
- Class V: Membranous LN
- Class VI: Advanced sclerosing LN (>90% sclerosed glomeruli)
- Neuropsychiatric (NPSLE): Seizures, psychosis, cognitive dysfunction, stroke.
- Cardiovascular: Libman-Sacks endocarditis (verrucous, non-bacterial, on mitral/aortic valves).
⭐ Malar rash (butterfly rash) characteristically spares the nasolabial folds.
📌 SOAP BRAIN MD (Mnemonic for SLE criteria - not exhaustive for clinical spectrum but helpful)
- Serositis
- Oral ulcers
- Arthritis
- Photosensitivity
- Blood disorders
- Renal disorder
- ANA positive
- Immunologic disorder (anti-dsDNA, anti-Sm, antiphospholipid Ab)
- Neurologic disorder
- Malar rash
- Discoid rash
SLE Diagnosis & Labs - Unmasking SLE
- 2019 EULAR/ACR Classification Criteria:
- Entry criterion: ANA $\ge$ 1:80.
- Additive weighted criteria from clinical & immunological domains; score $>$ 10 points needed for classification.
Key Autoantibodies in SLE:
| Antibody | Significance | Association(s) |
|---|---|---|
| ANA | Screening (entry criterion) | Sensitive, not specific |
| Anti-dsDNA | Specific, monitors activity, lupus nephritis | Lupus nephritis, disease activity |
| Anti-Sm | Highly specific | Diagnostic marker |
| Anti-Ro (SSA) | Neonatal lupus, Sjogren's, photosensitivity | SCLE, congenital heart block, Sjogren's |
| Anti-La (SSB) | Neonatal lupus, Sjogren's | Sjogren's, less common than Anti-Ro |
| Antiphospholipid Abs | Thrombosis, pregnancy morbidity | Antiphospholipid Syndrome (APS) |
* ↓C3, ↓C4 (complement consumption, active disease)
* ↑ESR (inflammation, non-specific)
⭐ Anti-Sm antibody is the most specific antibody for SLE.
SLE Management & Complications - Calming the Storm
Goals: Achieve remission, prevent flares & organ damage.
- General Measures: Sun protection, lifestyle. HCQ for ALL (unless contraindicated).
⭐ Hydroxychloroquine (HCQ) is recommended for all SLE patients unless contraindicated, as it reduces flares and improves survival.
- Pharmacological Therapy (Severity-based):
- Mild: NSAIDs, low-dose corticosteroids.
- Moderate/Severe: Corticosteroids (high-dose/pulse), Immunosuppressants (Mycophenolate Mofetil - MMF, Azathioprine - AZA, Cyclophosphamide - CYC), Biologics (Belimumab for refractory).
- Lupus Nephritis Management:
- Induction: MMF or CYC + high-dose steroids.
- Maintenance: MMF or AZA.
- Drug-Induced Lupus: 📌 Hydralazine, Procainamide, Isoniazid (HPI). Anti-histone Abs characteristic.
- SLE & Pregnancy: HCQ safe. Plan conception during remission (≥6 months).
- Key Complications: Lupus Nephritis, accelerated atherosclerosis, infections, osteoporosis, AVN.
Treatment Algorithm:
High-Yield Points - ⚡ Biggest Takeaways
- SLE is a multisystem autoimmune disease predominantly affecting young females.
- ANA is a sensitive screening test; anti-dsDNA and anti-Sm antibodies are highly specific.
- Characteristic skin manifestations include malar rash (butterfly rash) and discoid rash.
- Lupus nephritis is a major cause of morbidity; renal biopsy is crucial for prognosis and management.
- Drug-induced lupus (e.g., hydralazine, procainamide) is often associated with anti-histone antibodies.
- Coexisting Antiphospholipid Syndrome (APS) significantly ↑ risk of thrombosis and recurrent fetal loss.
- Hydroxychloroquine (HCQ) is a cornerstone for long-term management in most patients.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

