RA Basics - Joint Under Siege
- Chronic, systemic autoimmune inflammatory disorder causing symmetrical, erosive polyarthritis.
- Epidemiology: ~1% global (India ~0.75%); F:M 3:1; peak onset 30-50 yrs.
- Risk Factors:
- Genetic: HLA-DR4 (Shared Epitope), PTPN22.
- Environmental: Smoking (major!), infections (P. gingivalis, EBV).
- Pathogenesis:
- T/B cell dysregulation → autoantibodies (RF, ACPA).
- Key cytokines (TNF-α, IL-1, IL-6) drive synovitis, pannus formation, leading to cartilage & bone erosions.

⭐ Smoking is the most significant modifiable environmental risk factor for developing RA, especially seropositive RA (ACPA+).
RA Signs - The Body's Complaint
- Articular (Joints):
- Symmetrical polyarthritis (MCP, PIP, MTP, wrists). Spares DIPs.
- Morning stiffness > 1 hour, eases with activity.
- Pain, swelling, tenderness.
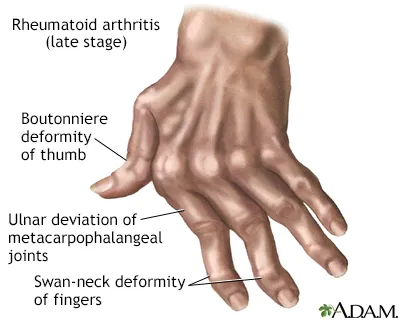
- Late deformities: Swan neck, Boutonnière, ulnar deviation.
- Atlantoaxial subluxation (C1-C2).
- Extra-articular Manifestations:
- Systemic: Fever, fatigue, weight loss.
- Rheumatoid nodules (extensor surfaces).
- Pulmonary: Pleurisy, nodules, ILD. Caplan syndrome (RA + pneumoconiosis).
- Cardiac: Pericarditis, ↑CV risk.
- Ocular: Scleritis, episcleritis, Sjogren's.
- Heme: Anemia of chronic disease.
- 📌 Felty's Syndrome: RA + Splenomegaly + Neutropenia.
- Vasculitis (nail-fold infarcts).
- Neuro: Carpal tunnel syndrome.
⭐ Felty's syndrome (RA, splenomegaly, neutropenia) is a classic triad associated with severe, long-standing RA and increased risk of infections.
RA Detective - Cracking the Case
- 2010 ACR/EULAR Criteria: Score ≥ 6/10 for diagnosis.
- Key domains:
- Joints: Number & size (small > large).
- Serology: RF, Anti-CCP (ACPA) levels.
- Acute Phase Reactants: ESR, CRP.
- Symptom Duration: ≥ 6 weeks.
- Key domains:
- Key Investigations:
- Serology:
- Rheumatoid Factor (RF): Positive in ~70-80%; not specific.
- Anti-CCP (ACPA): Highly specific (~95%); often positive early.
⭐ Anti-CCP antibodies are more specific for RA than RF and may predict more severe, erosive disease.
- Inflammatory Markers: ↑ ESR, ↑ CRP (correlate with disease activity).
- Imaging:
- X-rays (Hands & Feet): Periarticular osteopenia, joint space narrowing, marginal erosions (characteristic but late).
- Ultrasound/MRI: Detect synovitis, early erosions.
- Synovial Fluid Analysis: Inflammatory (WBC 2,000-50,000/µL, >50% PMNs, sterile, poor mucin clot).
- Serology:
RA Battle Plan - Taming the Flame
Goal: Remission or Low Disease Activity (LDA). Employ Treat-to-Target (T2T) strategy. Monitor disease activity (DAS28, CDAI) every 1-3 months.
-
Non-Pharmacological:
- Patient education, physiotherapy, occupational therapy.
- Lifestyle: Smoking cessation, weight management, joint protection.
-
Pharmacological:
- Bridge Therapy: Glucocorticoids (low-dose, short-term, e.g., Prednisolone ≤10 mg/day), NSAIDs for symptom relief.
- csDMARDs (Conventional Synthetic):
- Methotrexate (MTX): Anchor drug. Start within 3 months of diagnosis. Dose: 7.5-25 mg/week. Folic acid supplementation (1-5 mg/day or 5 mg/week 24-48h post-MTX).
- Alternatives/Adjuncts: Leflunomide (LEF), Sulfasalazine (SSZ), Hydroxychloroquine (HCQ - mild RA/combo).
- bDMARDs (Biologic): If csDMARDs fail (inadequate response after 3-6 months of optimal therapy).
- TNF-α inhibitors: Etanercept, Infliximab, Adalimumab.
- Others: Rituximab (anti-CD20), Tocilizumab (anti-IL6R), Abatacept (CTLA4-Ig).
- ⚠️ Screen for latent TB, HBV, HCV before initiating.
- tsDMARDs (Targeted Synthetic - JAK inhibitors): Tofacitinib, Baricitinib, Upadacitinib. Oral. For csDMARD/bDMARD failure/intolerance.
⭐ Methotrexate (MTX) is the cornerstone DMARD; initiation within 3 months of RA diagnosis is crucial for better prognosis.

High‑Yield Points - ⚡ Biggest Takeaways
- Symmetrical polyarthritis of small joints (MCP, PIP) with morning stiffness > 1 hour.
- Key serology: Rheumatoid Factor (RF) and highly specific Anti-CCP antibodies.
- Common extra-articular features: rheumatoid nodules, interstitial lung disease, vasculitis.
- X-ray shows juxta-articular osteoporosis, erosions, and joint space narrowing.
- Early DMARD (e.g., Methotrexate) therapy is crucial to prevent joint damage.
- Felty's syndrome: RA triad of arthritis, splenomegaly, and neutropenia.
- Caplan syndrome: RA with pneumoconiosis and intrapulmonary nodules.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

